Treacher Collins Syndrome
Contact the Craniofacial Center
What is Treacher Collins syndrome?
Treacher Collins syndrome is a rare, condition that affects how the face develops — especially the cheekbones, jaws, ears and eyelids. These differences often cause problems with breathing, swallowing, chewing, hearing and speaking. Children with this have typical intelligence and ability to learn. Hearing loss may affect learning in some kids.
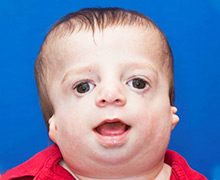
Treacher Collins syndrome is present when a baby is born (congenital), and it varies widely from child to child.
Children with this condition need coordinated care by providers from many areas of healthcare. At Seattle Children’s Craniofacial Center, we take an interdisciplinary approach to treating your child and supporting your family. Our team of experts covers 19 different specialties.
Treacher Collins syndrome happens in about 1 in 50,000 newborns worldwide. The condition is also called mandibulofacial dysostosis or Franceschetti-Zwalen-Klein syndrome.
What causes Treacher Collins syndrome?
Treacher Collins syndrome happens because of a change (mutation) in a that affects how a baby’s face develops before birth.
About 60% of children with Treacher Collins syndrome have it because of a new genetic change that was not inherited from either parent. Other times, a parent passes the genetic change to a child.
Treacher Collins Syndrome Care at Seattle Children's
What are the symptoms of Treacher Collins syndrome?
Most children with Treacher Collins syndrome have these symptoms:
- A very small lower jaw and chin (micrognathia)
- A very small upper jaw (maxillary hypoplasia)
- Small cheekbones
- Ears that are very small (microtia), are not the typical shape or are missing
- Eyes that slant downward
- A notch in their eyelids (coloboma)
Some children with Treacher Collins syndrome also have:
- Hearing loss caused by problems with the ear canal or the 3 bones in the middle ear that transmit sound. At least half of children with Treacher Collins syndrome have hearing problems.
- An opening in the roof of their mouth (cleft palate).
- An airway that is so small it causes serious breathing problems.
How is Treacher Collins syndrome diagnosed?
To diagnose this condition after birth, our team will examine your child carefully. An exam may be all that is needed for diagnosis.
Your child’s doctor may take or to make plans for treatment.
Rarely, doctors are able to diagnose Treacher Collins syndrome before a baby is born if they can see the facial differences during an .
Genetic counseling and testing
Our Craniofacial Genetics Clinic helps identify conditions caused by changes in genes. Our and help you understand the pros and cons of genetic testing. They can explain test results and your chance of having a child with Treacher Collins syndrome in a future pregnancy.
Treacher Collins syndrome may affect some members of your family more severely than others. Genetic counseling can help you make informed decisions about family planning and your child’s treatment.
How is Treacher Collins syndrome treated?
There is no single care plan for children with Treacher Collins syndrome. The treatments and timing we recommend depend on your child’s specific needs. Our specialists provide a wide range of services to help with feeding, cleft palate, breathing, jaw size, cheekbones, hearing, eyelids, ears, speech and how the jaws and teeth align.
Our goal is to reduce the number of steps in your child’s treatment by improving the outcome of each step.
3-D imaging is a powerful tool to help us predict future growth. Our surgery and orthodontic corrections take into account continued growth of your child’s bones. This way, when your child is finished growing, their bones are in the desired position.
-
Feeding and cleft palate repair
Babies with Treacher Collins often are born with a very small jaw. About 25% of children with the syndrome have an opening in the roof of their mouth (cleft palate).
These differences in the face often cause problems with breast and bottle-feeding. We help you with feeding techniques during your baby’s first months.
We will check regularly to make sure that your baby is gaining weight. A may see you in the clinic to help you with your child’s diet.
If your child has cleft palate, our surgeon will talk with you about repairing the roof of their mouth. Usually this happens at about 12 to 16 months of age.
-
Easing breathing
Babies with very undersized facial bones may have breathing problems. If this is the case for your baby, your child’s doctors will discuss the options to manage and correct the cause.
Options may include:
- Putting your baby in a position that helps them breathe more easily
- Surgery to make the jaw longer and move it forward
- Surgery on the inside of the nose to fix a blocked airway
- Placing a breathing tube in the windpipe (tracheostomy) for severe breathing problems
- Using an
Sometimes children have trouble breathing while they sleep (). Over time, this may lead to problems with how their heart and lungs work. It also can play a part in problems with learning and behavior.
We will ask questions during clinic visits to check if this may be a problem. To better understand their breathing patterns, we may do an overnight sleep study (polysomnogram) in our sleep lab.
The treatment options and timing will depend on your child.
-
Enlarging the jaw
There are several options for surgery to change the shape of the jaw and improve how it works. Often, children need a series of operations done in stages.
Counterclockwise craniofacial distraction osteogenesis (C3DO)
For children who have had a breathing tube in their windpipe (tracheostomy), we may recommend counterclockwise craniofacial distraction osteogenesis (C3DO). Usually, this surgery happens when your child is 6 to 10 years old.
Seattle Children’s Craniofacial Center is the first to use C3DO to improve breathing and correct jaw rotation in children with Treacher Collins syndrome. The goal is to allow a child to breathe without a tube in their windpipe. Surgeons around the world are adopting our approach.
This approach may work better than the standard treatment for Treacher Collins syndrome. C3DO gets better results for children by combining 2 procedures that are usually done separately.
Bone graft
Surgeons use a bone graft instead of distraction if the joint between your child’s jawbone and skull (temporomandibular joint) is not stable.
- Surgeons use a piece of bone from your child’s rib to lengthen the jawbone or make a new jaw joint.
- They take the bone graft from a single rib through a small incision on your child’s chest.
- After surgery, the new bone in the jaw will become hard and strong. The bone that was taken from the rib will often grow back.
- Doctors first consider this option when your child is 4 to 7 years old.
-
Rebuilding cheekbones
Undersized or missing cheekbones can usually be rebuilt with bone grafts.
- Surgeons take the bone grafts from your child’s skull. The skull is a good source of the strong bone needed to replace the cheeks.
- If your child has subcranial rotation distraction, we do surgery on their cheekbones when we remove the distraction devices.
- If your child does not have subcranial rotation distraction, surgeons usually rebuild the cheekbones when your child is 8 to 10 years old. Less often, cheekbone surgery happens during the teen years, after surgery to align the jaw.
In some children with Treacher Collins syndrome, the skin over their cheekbones is very thin and sometimes slightly darker than the rest of their skin. We may recommend padding the skin in this area before surgery on the cheekbones.
- The surgeon takes fat from your child’s belly and injects it under the skin that covers their cheekbones.
- This is a common procedure used for cosmetic reasons in adults. It is very successful in treating the cheekbone skin in children with Treacher Collins syndrome.
- The treatment usually takes 2 or 3 steps. The steps happen 6 to 12 months apart.
- Each step takes about 1 hour. Your child will likely be able to go home after the surgery, without spending the night in the hospital.
-
Managing hearing problems
At least half of children with Treacher Collins syndrome have hearing loss. It may happen because:
- Sound is blocked from reaching the inner ear (conductive hearing loss). This may be caused by very narrow or missing ear canals.
- Problems with the 3 bones in the middle ear that transmit sound.
Most often, your baby’s care team will screen their hearing in the hospital soon after birth or within a few days. If problems are found, we do further testing. A specialist trained to test hearing in infants and children () will perform the tests.
As your child grows, they will have other hearing tests based on their ear health and how well they hear.
Our ear, nose and throat specialist () and audiologist will talk with you and your child about your child’s hearing, such as:
- Whether they need hearing aids
- How to prevent further hearing loss
- The best place to sit in the classroom when your child reaches school age
The small size of the outer ear may make it hard for your child to wear hearing aids. One option might be bone-anchored hearing aids that are attached to the skull with a small screw.
Your child may need a to check their middle and inner ear. We do this at about 4 to 5 years of age, when the ear is nearly done growing. CT scans help doctors decide if surgery could help restore hearing.
-
Repairing eyelids
Sometimes differences in the lower eyelid leave a child’s eye unprotected or at risk for infection or scarring of the eye (corneal exposure). If so, we may recommend surgery to improve how the lid works and change how it looks.
The surgery we recommend depends on your child. Options include:
- Removing a small wedge of the lower eyelid to tighten it (wedge excision)
- Using a small flap of skin from the upper eyelid to better support the lower eyelid (lid switch flap)
- Using a small piece of tendon to raise the lower eyelid (fascial sling)
-
Addressing ear differences
Many children with Treacher Collins syndrome have ears that are not the typical shape or are missing. This is called microtia. Our Otolaryngology program is among a few in the country to offer comprehensive treatment for microtia. Our team is skilled at rebuilding ears using artificial (alloplastic) materials or cartilage from the ribs (autologous). Our options also include a prosthetic ear that your child can put on and take off. Read more about microtia treatment.
-
Improving speech
In some children with Treacher Collins, the muscles in the back of the mouth do not work the typical way. About 25% are born with a .
Both conditions can affect your child’s ability to make speech sounds. Velopharyngeal dysfunction is a type of speech problem.
If you or your child’s doctors have concerns about your child’s speech, your child will see a .
-
Aligning jaws and teeth
Your child will need surgery to align their jaws if they do not fit together well when their bones have finished growing. This is called orthognathic surgery. Usually, the bones finish growing at 16 years for a female and 18 years for a male.
Your child may need to have Le Fort I maxillary advancement surgery, mandibular osteotomy or both procedures.
After surgery on the jaw, your child will wear braces to hold the teeth until they settle into their new position. This takes at least 6 months.
Read more about craniofacial orthodontics.
Why choose Seattle Children’s for Treacher Collins syndrome treatment?
Seattle Children’s Craniofacial Center has treated many children with Treacher Collins syndrome. We have experts in every field your child might need. Our extensive experience with this rare condition helps us continually improve our care so your child gets the best results.
Many of our patients are babies who are newly diagnosed. We also work with children who received their initial care at another hospital. We treat children, teens and young adults up to age 21 and sometimes beyond.
- Team-based care from experts: Your child’s team will include a craniofacial , nurse, and . Based on your child’s needs, they may also receive care from an ear, nose and throat specialist (); craniofacial ; ; ; ; ; and .
- Better results with fewer surgeries: Our approach helps children get the greatest benefit from surgeries early in childhood. As a result, later in life, some surgeries are either not needed or are less extensive. Often, we combine surgery to cut a bone with distraction osteogenesis, which lets us make bigger changes than traditional surgery alone. In some cases, we use counterclockwise craniofacial distraction osteogenesis (C3DO) to get better results by combining 2 procedures that are usually done separately.
- The right treatment at the right time: From the start, we help your baby with breathing and feeding problems. We check your child’s chewing, eyesight, hearing and speech development and recommend treatments for any issues they have. As your child grows, we do surgeries as needed for their jaws, cheekbones, mouth, eyes and ears.
- Support for your whole family: A diagnosis of Treacher Collins syndrome can be scary. We take time to explain your child’s condition. We help you understand your child’s treatment options and make the choices that are right for your family.
- Research to improve your child’s quality of life: Our researchers are investigating long-term outcomes for children with ear and jaw differences and developing a system to describe and rate the physical traits of undersized ears and how severe each case is.
Contact Us
Contact the Craniofacial Center at 206-987-2208 for an appointment, a second opinion or more information.
If you live outside of Washington, Alaska, Montana and Idaho, please contact our coordinator for out-of-area patients at 206-987-0814.
Providers, see how to refer a patient.
Paying for Care
Learn about paying for care at Seattle Children’s, including insurance coverage, billing and financial assistance.
