Microtia and Aural Atresia
Contact Otolaryngology
What are microtia and aural atresia?
In microtia (my-KRO-sha), a child is born with a very small or missing ear. Microtia varies from child to child. Most often it affects just 1 ear, but sometimes both ears are affected.
In 70% of children with microtia, the ear canal is missing. This is called aural atresia. It causes hearing loss.
About 10% of children with microtia also have problems that affect the heart, eye, kidney, spine or face. Small or missing ears are associated with conditions such as craniofacial microsomia and Treacher Collins syndrome.
Symptoms of Microtia and Aural Atresia
Your child may be born with an outer ear that is very small or is missing parts. Some children are born without an ear (called anotia). Microtia usually involves 1 side, though both ears may be affected.
In 70% of children with microtia, the ear canal is missing. Without an ear canal, sound cannot be carried to the inner ear and hearing nerve. This is called conductive hearing loss.
Otolaryngology at Seattle Children's
Diagnosing Microtia and Aural Atresia
If your child is born with small or missing ears, the doctor will look for problems with their ear canal and check your baby’s hearing.
The doctor will check your child’s other ear for problems. Because some children with microtia also have problems with other body systems, the doctor will do a careful exam.
Rarely, microtia and related conditions are diagnosed before a baby is born if an ultrasound during pregnancy shows ear differences.
Our Approach to Microtia and Aural Atresia Treatment
- Our team of specialists fully assesses your child to understand the extent of their microtia and atresia.
- We work closely with your child and family so you know all the options and the best timing and order of procedures. Careful planning is key to the best care, because surgery to rebuild the outer ear can affect options to treat hearing loss.
- In your child’s early years, our team’s focus is to assess and treat any hearing loss. This is especially important if both ear canals are missing. We monitor your child’s speech and language as they grow.
- We do not rush to rebuild your child’s ear, because we feel it is important for your child to have a say in the choices made. Most children are mature enough to take part in treatment decisions by age 7. We take the time to show you and your child all options and support your family in the choices you make.
- Deciding the best option for your child’s microtia depends on many factors. These include the size of the small ear, whether it is possible to surgically create an ear canal and what you and your child prefer.
- Treatment options for microtia include:
- Surgery to build a new ear using your child’s rib cartilage
- Surgery to implant an ear made of special plastic
- Wearing a removable (prosthetic) ear
- Leaving the ear as it is
- Options for hearing loss include:
- Surgery to create an ear canal and eardrum
- A range of hearing devices
- If your child has related health problems, they will see other specialists as needed. About 10% of children with microtia have facial gaps (clefts) or problems affecting their heart, eye, kidney or spine. Every year our Craniofacial Center cares for hundreds of children with conditions such as craniofacial microsomia (CFM) and Treacher Collins syndrome.
Treating Hearing Loss
See photos and details of device options for hearing loss (PDF).
-
Assessing hearing and speech
From babyhood to young adult years, we monitor your child’s hearing and speech development.
We start testing your child’s hearing very early. Most children with microtia have some hearing loss in their small ear. The hearing test will also tell us about the hearing in your child’s non-affected ear.
Children with normal hearing in 1 ear often develop normal speech and language. But even hearing loss in 1 ear can make it harder for young children as they learn speech and language.
There are 2 main types of hearing tests:
- BAER (brainstem auditory evoked responses) testing measures your child's physical response to quiet sounds. We use this if your child is not able to cooperate with behavioral testing.
- Behavioral testing (audiogram) measures how your child behaves in response to speech and other sounds. We tailor the test to your child's age and development, starting as young as 6 months.
We may suggest other tests, based on your child’s age. Your child’s audiologist and otolaryngologist will discuss the options for hearing management, based on the results of the hearing tests.
Read about:
- Newborn Hearing Screening (PDF) (Spanish)
- BAER and EOAE Testing (PDF) (Spanish)
- BAER and EOAE Hearing Tests Under Anesthesia (PDF) (Arabic) (Spanish)
- My Visit to the Audiology Clinic (PDF)
- Conductive Hearing Loss (PDF) (Spanish)
-
Headband hearing device
If your child has a hearing loss, we fit them with a headband hearing device that transfers sound waves through the bones in their skull to the inner ear. This is called a bone conduction sound processor (BCSP).
Your child will start wearing the headband in their first months of life because hearing is so important for speech and language development. Thanks to generous donors, we offer families a free 1-month trial of the device.
Most children wear the headband hearing device until about age 5.
-
Bone-anchored hearing device
Around age 5, the options for treating hearing loss include a bone-anchored hearing implant. Surgeons place a titanium implant in the skull bone just behind your child’s ear. Attached to the implant is either a magnet under the scalp or a connector that sticks through the skin. In this way, a bone conduction sound processor (BCSP) is held in place on the outside of your child’s head.
This BCSP sends sound waves to the hearing nerve through the bones in your child’s skull.
Often we place the implant during surgery to repair your child’s outer ear. Combining the procedures means less time in the hospital and fewer procedures to recover from.
-
Creating an ear canal
When your child is 5 or 6 years old, we do a CT (computed tomography) scan to examine their middle and inner ear. At that age, the ear is almost fully grown. CT scans help doctors decide if surgery to open the ear canal is likely to improve hearing.
Deciding if this surgery is an option depends on your child’s middle and inner ear structures and their facial nerve. The best timing for this surgery is when a child is 6 to 8 years old.
During the procedure, surgeons open the ear canal, create an eardrum and reposition the ear bones. The goal of this surgery is to greatly improve your child’s hearing and allow them to wear a standard hearing aid if needed.
-
Hearing aids to amplify sound
A variety of hearing aids may help children who have an ear canal but still have trouble hearing. The style used will depend on your child’s age, listening needs and size of their ear canal. Options include:
- The CROS system. Your child wears a microphone on the ear with hearing loss. It sends sound wirelessly to a device in the hearing ear. CROS stands for “contralateral routing of signal,” meaning it sends a signal to the opposite side of the head.
- A traditional hearing aid worn behind the ear (BTE).
- A hearing aid worn in the ear (ITE).
Treating Microtia
If a bone-anchored hearing device is part of your child’s treatment, most likely we will place the implant at the same time we do surgery to repair your child’s outer ear.
See photos and pros and cons of microtia treatment options (PDF).
-
Creating an ear from your child’s rib
We wait until your child is at least 7 years old to offer reconstructive surgery using your child’s own rib cartilage and skin to make a larger ear. Age 7 is the soonest that a child will have enough cartilage and is old enough to take part in the decision.
Because your child’s own tissue is used, their body can heal on its own if the ear is ever injured. This is called “autologous” reconstruction. Our surgeons are very experienced in shaping rib to make the new ear. We use 3D printings of rib cartilage to train and practice. This is the better choice if your child will have surgery to open their ear canal.
The surgery takes 4 hours and involves 2 surgeons. Your child will stay overnight in the hospital. The surgical team collects the rib and makes the new ear that will be implanted. To collect the rib cartilage, we make a cut of less than 1 inch, which is much smaller than most other hospitals can do. We are committed to making a minimal impact on the rib, with a small scar.
After surgery, the ear lies flat against your child’s head. In 2 to 4 months we do a second surgery, using a skin graft from your child’s groin to line the back of the ear and help position it. Your child will be able to go home on the same day as this second surgery.
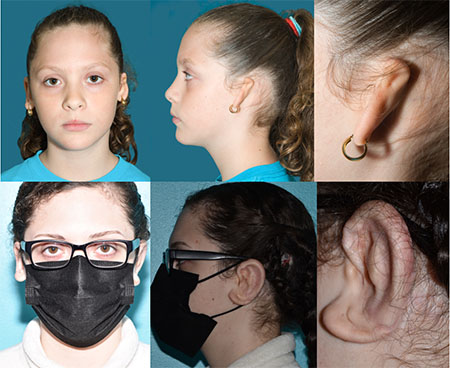
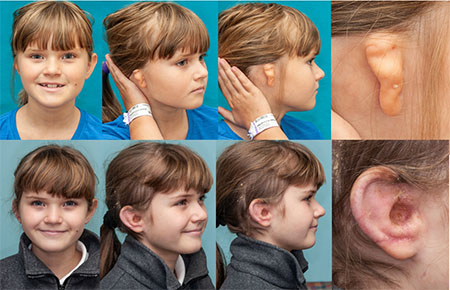
(Top) 10/02/2013 Preoperative photos. (Bottom) 2/23/2021 Six years after left ear reconstruction using patient’s cartilage.
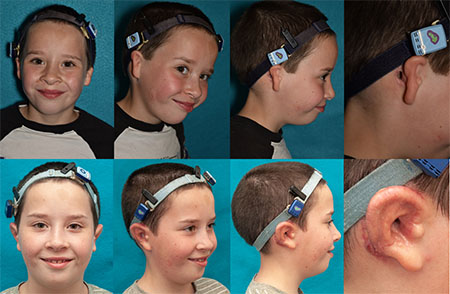
(Top) 4/05/2018 Eight months after creation of right ear canal, before ear reconstruction. (Bottom) 03/15/2021 Four months after elevation of right reconstructed ear.
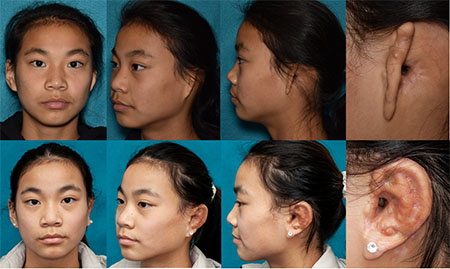
(Top) 05/13/2020 Sixteen months after creation of ear canal. (Bottom) 03/10/2021 Four months after second stage surgery for cartilage reconstruction.
-
Implanting an alloplastic ear
Another option for ear reconstruction uses a premade framework of biocompatible plastic to create a new ear. This is called an alloplastic ear. We offer this option starting about 5 years old, but prefer to wait until age 7, so your child is old enough to help make the decision.
Surgeons make a small cut (incision) on the side of your child’s head to place the plastic ear. During surgery we reshape the ear so it’s a better match for your child’s other ear. We cover the plastic ear with tissue from your child’s head and skin from other parts of their body. This helps it heal without infection.
This single-stage reconstruction surgery takes 6 to 8 hours. Your child will likely stay overnight in the hospital.
Biocompatible means a material can be safely used to repair or replace body parts that are diseased or missing. They may be made of metals, ceramics or plastics called polymers. These natural or synthetic materials are safe to implant in the human body because the body’s immune system does not react against them.
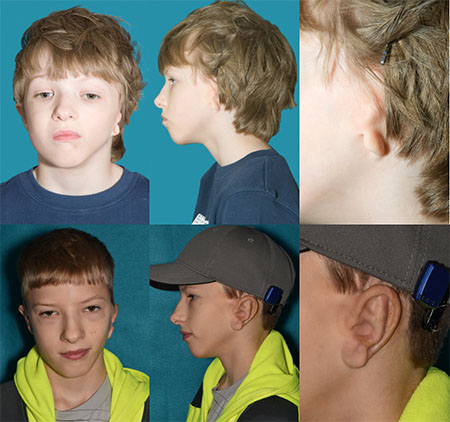
Medpor™ reconstruction: (Top) 4/18/2002 Preoperative photographs. (Bottom) 12/04/2017 One year after reconstruction with Medpor™.
Medpor™ reconstruction. (Top) 7/31/2019 Preoperative photographs (Bottom) 01/04/2021 Four months after reconstruction with Medpor™.
-
Removable synthetic ear (prosthesis)
Instead of surgery, some children choose a synthetic ear that is attached in the morning and removed each night. This is an option starting at about age 6. We make a mold of your child’s other ear to use as a template.
A specialist makes the prosthesis from silicone, a blend of synthetic rubber and plastic.
There are 2 ways to keep the prosthetic ear in place:
- Using special glue to attach the ear over the microtia. No surgery is needed.
- Using magnets and clips to attach the ear to implanted posts. First we do surgery to remove your child’s small ear and place titanium implants in their skull bone. Several months later, we do surgery to attach posts to the implants.
-
Leaving the ear as is
Some families decide to leave their child’s outer ear as it is. If so, we focus on your child’s hearing, so they develop normal speech and language. We support your family in whatever choice you make.
Contact Us
If you would like an appointment, ask your child’s primary care provider to refer you.
If you have a referral or would like a second opinion, contact our Otolaryngology Program at 206-987-2105.
Providers, see how to refer a patient to Otolaryngology.
Related Links
- Otolaryngology Resources
- Treatment Options for Microtia (PDF) (Spanish)
- Conductive Hearing Loss (PDF) (Spanish)
- Device Options for Hearing Loss (PDF) (Spanish)
- Aural Habilitation Therapy (PDF) (Spanish)
- Hearing Loss Clinic (PDF) (Spanish)
- My Visit to the Audiology Clinic (PDF)
Paying for Care
Learn about paying for care at Seattle Children’s, including insurance coverage, billing and financial assistance.

