3-D Imaging
What is 3-D imaging?
3-D imaging uses special cameras, advanced software and fast computers to make detailed pictures of your child’s face or head. Your child’s healthcare team uses the detailed views to accurately diagnose your child and help guide their treatment.
At Seattle Children’s, we use:
- 3-dimensional and advanced software to build precise maps of the bones and muscles of your child’s face and head. To make the images, your child lies on a bed that moves through the CT scanner. The entire scan only takes about 15 seconds.
- A 3dMD camera system to get a 3-D map of the outside of a child’s face or head. The system has 5 cameras that capture much more detailed information than a regular photograph. Unlike an X-ray, the 3dMD system does not use radiation to make an image.
With both of these 3-D technologies, data is fed into a fast computer. Powerful software merges the many viewpoints into a single 3-D image. The system creates realistic color images with depth, context and detail of your child’s face and head.
Why choose Seattle Children’s?
We are the only children’s hospital in the region using a 3dMD system to create clinically accurate 3-D surface images of children with conditions that affect the skull and facial bones, such as craniosynostosis and craniofacial microsomia.
The 3-D CT scan images that can be made at Seattle Children’s help doctors understand where bones have developed abnormally.
Our team is experienced using these detailed images to:
- Diagnose your child’s condition with greater precision
- Plan the best treatment for them
- Guide surgery in the operating room
- Evaluate the results of treatment
How can 3-D imaging help my child?
-
Fast, accurate scans with less radiation
We use very low-dose, high-speed CT scan imaging compared to conventional CT scanners. This lets us get the best image with the lowest possible radiation exposure. It also means your child needs to stay still for a shorter amount of time during the scan.
In a published study, we showed how we reduced the number of full-dose CT scans by 42% in a 1-year period. The low-dose scans used one-half or less radiation than a standard CT scan of the head. Even with less radiation, images were of a high enough quality to make the diagnosis.
With our high-speed scanner, CT exams that once took many minutes now take less than 10 seconds. This makes it less likely that your child will move during imaging so there is less need to:
- Give your child medicine to prevent them from moving
- Repeat imaging because of movement during the scan
The high-speed CT scanner also lets doctors capture activity in the body that lasts a very short time. One example is CT scanning that requires injecting a dye to highlight blood vessels as the dye passes through them. The dye remains in one place for only a few seconds before it flows away. Conventional CT technology is too slow to make a picture of the blood vessels before the dye disappears. By capturing 16 cross-sectional images (slices) per half-second, the high-speed scanner gets the job done.
-
More effective craniofacial surgery
Some children with craniofacial conditions need surgery to move bones of their face or head. Using 3-D imaging and advanced software lets the team:
- Predict your child’s future growth and plan for the desired position of bones at adulthood
- Create physical models that are so realistic surgeons can practice upcoming operations
- Plan the exact steps in complex surgeries and refer to the plan in the operating room
- Make surgeries faster and more efficient, which shortens the time your child is under anesthesia
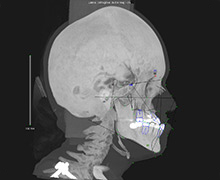
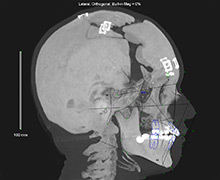
Before (left): Our team used 3-D CT scans to create this image of a child’s head and face before surgery.
After (right): This image shows changes in the girl’s bones after surgery to move her forehead and face forward.
-
Making treatment choices clearer
The detail in 3-D images makes it easier for doctors to show you how treatment is likely to improve your child’s condition.
Seeing a 3-D image of the expected results for your child can help as you make decisions about their treatment.
-
Predicting how facial implants will affect appearance
Some children need implants to help make their bones and tissue look more typical. Facial implants are artificial, bonelike structures. Doctors insert them under your child’s skin to support the face and correct its shape.
Our doctors use 3-D images to decide where to use implants and predict how they will affect your child’s appearance.
In some cases, 3-D images and computer-assisted design (CAD) technology help the team design implants that are custom-made for your child’s face.
-
Evaluating treatment for “water on the brain” (hydrocephalus)
Build-up of fluid in the skull can be life threatening and can occur in children with craniosynostosis. The fluid build-up is called hydrocephalus, or “water on the brain.”
Most of the time, surgeons place a shunt in the skull to drain the extra fluid and prevent brain damage. With traditional imaging, doctors were less able to know that the shunt was working right. Using 3-D imaging technology, Seattle Children’s doctors have created a very accurate way to measure fluid in the brain.
-
Measuring treatment results
After surgery, we use 3-D imaging to measure your child’s results. This lets us improve surgical techniques and invent new ones.
Knowing which treatments have the best results helps us choose the right procedure for your child.
Research to Improve Craniofacial Care
Many of our doctors use 3-D images in their research to:
- Measure how severe a cleft is and how much surgery has changed it. Dr. Raymond Tse’s goal is to help surgeons decide on the best treatment for each child.
- Develop tools to measure how craniofacial microsomia and other conditions change facial features.
- Create a searchable library of 3-D images of children before and after surgery for craniosynostosis. Accurately measuring the changes in a child’s skull and face will help providers show which surgeries have the best results for specific conditions.
- Study how changes in genes disrupt typical development of the roof of the mouth (palate). Kai Yu combines mouse models and 3-D imaging to understand how the palate forms.
- Study obstructive sleep apnea in babies with craniofacial conditions, including Robin sequence. A team led by Kelly Evans aims to use 3-D images to determine the severity of a child’s breathing problem and decide which treatment will help the most.
Contact Us
To make an appointment, you or your child’s doctor can call the Craniofacial Center at 206-987-2208.
We encourage you to talk with your primary care provider about coming to Seattle Children’s specialists. This helps coordinate your care.
Providers, please see how to refer a patient.
