Tetralogy of Fallot
Contact the Heart Center
What is tetralogy of Fallot?
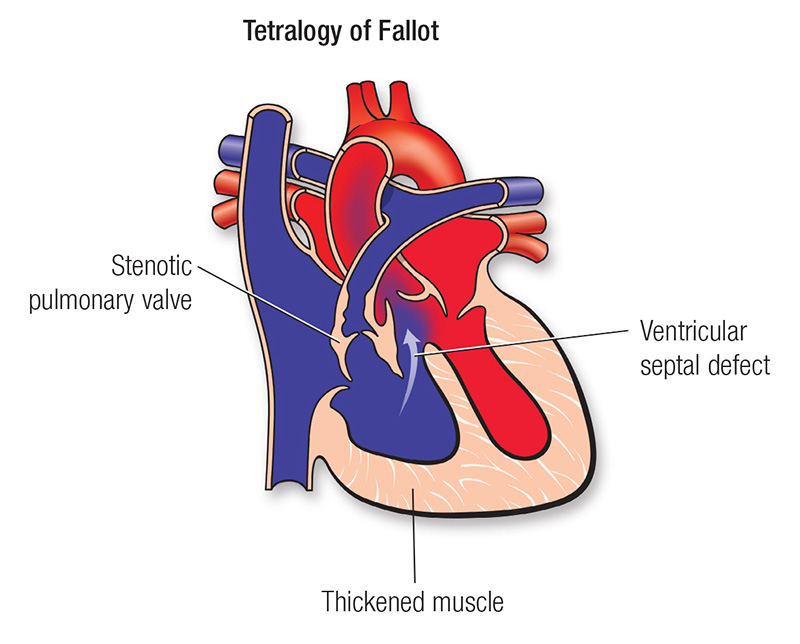
The 4 features of tetralogy of Fallot are as follows: Hole between the right and left ventricles, narrowed pulmonary valve, thickened right ventricle wall and aorta that leaves the heart from a different spot than normal. From heart.org. ©2009, American Heart Association, Inc.
Tetralogy of Fallot (pronounced teh-TRAHL-ah-jee of fah-LOH) is a rare, congenital condition that changes the normal flow of blood through your baby’s heart.
In medicine, “tetralogy” means a set of 4 things that happen together.
This condition involves 4 heart defects:
- There is a large hole in the septum, or wall, between the right and left ventricles. This is called a ventricular septal defect (VSD). It allows oxygen-poor blood to mix with oxygen-rich blood in the ventricles.
- The pulmonary valve is narrowed. This is called pulmonary stenosis. It limits blood flow from the right ventricle to the lungs. It forces some oxygen-poor blood through the VSD into the aorta.
- The muscle wall of the right ventricle is thickened. This is called right ventricular hypertrophy. It happens because the right ventricle has to work harder to try to get blood through the narrow pulmonary valve.
- The aorta leaves the heart from a different spot than normal. It leaves from right over the VSD. This is called overriding aorta. Normally, the aorta leaves the heart from the left ventricle.
Together, these 4 defects limit the flow of oxygen-poor blood from your baby’s heart to their lungs, where the blood should pick up oxygen. Instead, oxygen-poor blood leaves the heart and goes out to the rest of your baby’s body.
The 4 features of tetralogy of Fallot are as follows: Hole between the right and left ventricles, narrowed pulmonary valve, thickened right ventricle wall and aorta that leaves the heart from a different spot than normal.
Tetralogy of Fallot occurs in about 5 of every 10,000 babies. Some children with this problem are born with other conditions too, such as Down syndrome or DiGeorge syndrome.
Heart Center at Seattle Children's
Symptoms of Tetralogy of Fallot
The main effect of tetralogy of Fallot is that your baby’s blood does not carry as much oxygen as it should. A low oxygen level can make the baby’s skin, lips and fingernails look blue or purple tinged. This is called cyanosis.
Cyanosis can range from mild to severe. It depends on how much oxygen-poor (blue) blood makes it to your baby’s lungs and how much goes out to their body. Some babies with this condition appear bluish at birth. Some do not, but they may become cyanotic later as their pulmonary stenosis gets worse.
Your baby may also have trouble feeding and gaining weight normally, which doctors call failure to thrive.
-
Tet spells
Some babies with tetralogy of Fallot have episodes called tet spells, when they suddenly turn bluish and may faint. These spells are serious.
A tet spell may be caused by activities that change the pressure in your baby’s heart and increase the flow of oxygen-poor blood to their body. These may include crying, pooping or kicking their legs after waking up.
Your child’s doctor will talk with you about what do to if this happens to your child. They will show you how to put your baby’s legs in a position that adjusts the pressure and blood flow in your baby’s heart.
Tet spells happen most often in babies between 2 and 4 months old.
Diagnosing Tetralogy of Fallot
Sometimes doctors are able to diagnose tetralogy of Fallot in a developing baby before birth. They might first see something different about your baby’s heart on standard prenatal ultrasound. To learn more about your baby’s heart, you might have a fetal echocardiogram (an ultrasound done to check the heart more closely). Seattle Children’s Fetal Center team cares for pregnant women and their families when their developing baby has a known or suspected problem.
To diagnose this condition after your baby is born, your child’s doctor will examine your child and use a stethoscope to listen to their heart. In children with tetralogy of Fallot, doctors almost always hear a heart murmur – the sound of blood moving in the heart in a way that is not normal. Often, doctors detect tetralogy of Fallot during standard newborn screenings for serious heart problems.
The doctor will ask for details about your child’s symptoms, their health history and your family health history.
Your child will also need tests that give us information about how their heart looks and works. These may include:
- Echocardiography
- Electrocardiography
- Chest X-ray
- MRI (magnetic resonance imaging) of the heart
- Cardiac catheterization
Treatment Options for Tetralogy of Fallot
In recent years, the diagnosis and treatment of tetralogy of Fallot have improved greatly. Now, about 90% of children with this condition grow to adulthood and lead active lives.
Tetralogy of Fallot must be repaired with open heart surgery, either soon after birth or later in infancy. The timing depends on how severe your baby’s condition is.
After surgery, your child will need lifelong care and follow-up to check how well their right ventricle and pulmonary valve work and whether they need any further treatment.
-
Repairing heart defects with surgery
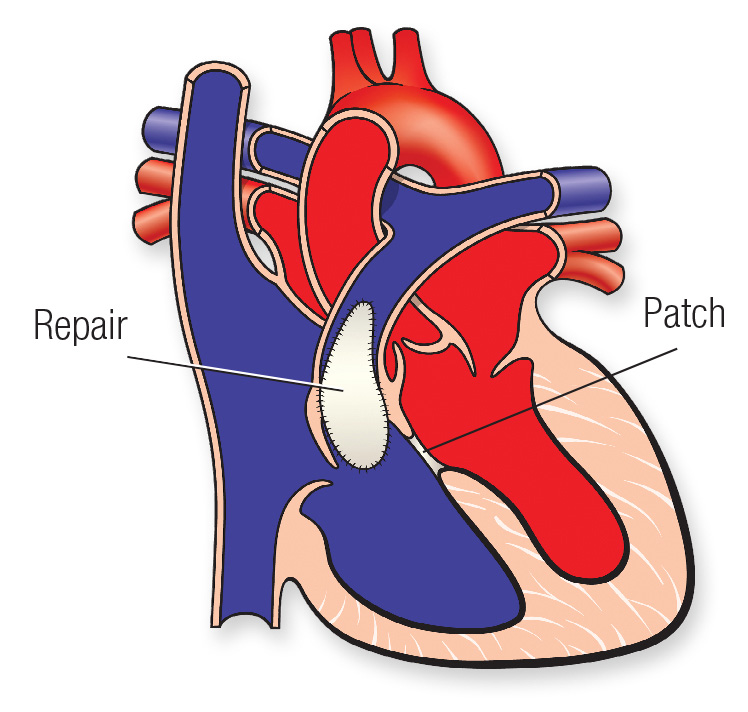 Surgery involves patching the hole between the right and left ventricles and opening up the narrow pulmonary valve. From heart.org. ©2009, American Heart Association, Inc.
Surgery involves patching the hole between the right and left ventricles and opening up the narrow pulmonary valve. From heart.org. ©2009, American Heart Association, Inc.Most children have a single surgery while they are still babies. Surgeons close the VSD with a patch and open the narrow pulmonary valve. Once the VSD is closed, the position of the aorta is not a problem.
Babies who have surgery usually do well. See our statistics and outcomes for tetralogy of Fallot repair.
Later in life, some children with tetralogy of Fallot need another procedure to put in a new pulmonary valve. This may be done by surgery or, more recently, by cardiac catheterization.
-
Reducing cyanosis
If your newborn has severe cyanosis, your child’s doctor may give the baby liquids through a vein (intravenously, or by IV) and medicines that help improve blood flow.
-
Managing tet spells
If your baby or child has tet spells, your child’s doctor will show you how to place your child in a knees-to-chest position. This adjusts the pressure and blood flow in their heart.
If tet spells happen often, typically this means it is important for your child to have surgery soon. We will make sure you understand what to watch for, what to do and when to call your child’s doctor about concerns like tet spells.
-
Improving blood flow to the lungs
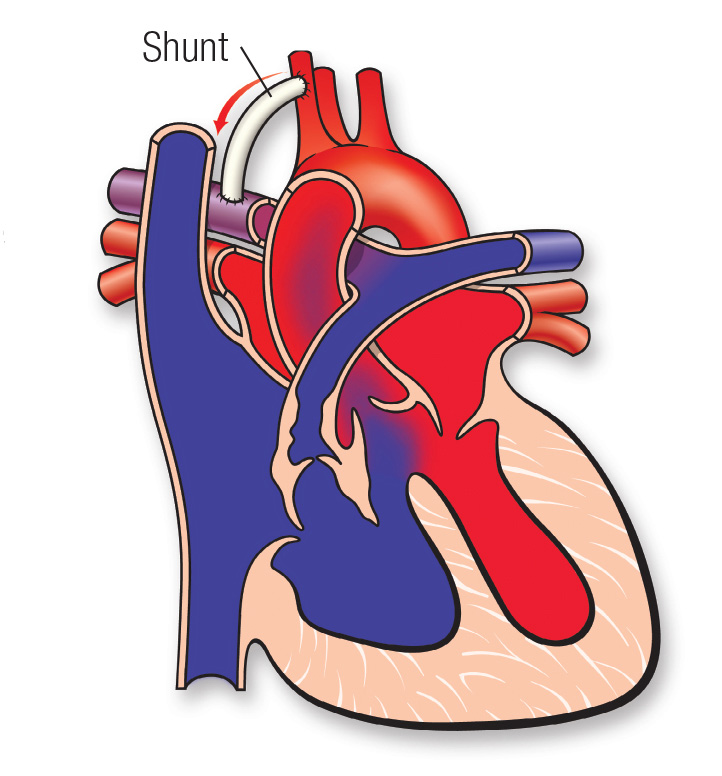 If needed, surgeons can place a tube called a shunt to improve blood flow to your child’s lungs. The shunt directs some blood from the aorta to the right pulmonary artery. From heart.org. ©2009, American Heart Association, Inc.
If needed, surgeons can place a tube called a shunt to improve blood flow to your child’s lungs. The shunt directs some blood from the aorta to the right pulmonary artery. From heart.org. ©2009, American Heart Association, Inc.Some babies have arteries in their lungs that are too small to receive much blood. Before these babies can have heart surgery, they may need treatment to increase blood flow to their lungs so their arteries will get bigger. Doctors have 2 ways to do this:
- Surgery to place a shunt that directs more blood to the lungs
- Cardiac catheterization to put a stent in the ductus arteriosus (Learn more about patent ductus arteriosus stenting.)
Later, these children have a separate surgery to correct their heart defects.
Tetralogy of Fallot at Seattle Children’s
-
The experts you need are here
- Our team of 40+ pediatric cardiologists diagnose and treat this condition in many babies every year – and we provide ongoing care for patients as they grow into young adults.
- Our pediatric cardiac surgeons perform more than 500 procedures yearly. Each has deep experience correcting tetralogy of Fallot in babies and, when needed, replacing a child’s pulmonary valve later in life.
- We also have a pediatric cardiac anesthesia team and a Cardiac Intensive Care Unit ready to care for children who undergo heart surgery.
- Cardiologists at Seattle Children’s are leaders in using new techniques and innovative devices to help hundreds of children each year avoid open-heart surgery. We are able to replace pulmonary valves through cardiac catheterization and hybrid procedures.
Watch Seattle Children’s Heart Warriors: Charlotte (Video. 2:09).
-
Among the nation’s top programs
- Our surgical outcomes are among the best in the nation year after year. See our outcomes for tetralogy of Fallot.
-
Care from before birth through young adulthood
- If your developing baby is diagnosed with tetralogy of Fallot before birth, our Fetal Center team works closely with you and your family to plan and prepare for the care your baby will need.
- Your child’s treatment plan is custom-made. Some babies will need care to help the arteries in their lungs get bigger before their heart can be repaired. Some children who had heart repair as an infant will need their pulmonary valve replaced later in childhood or as young adults. We closely monitor your child’s unique needs to make sure they get the care that’s right for them at every age.
- To meet your child’s long-term healthcare needs, we have a special Adult Congenital Heart Disease Program to transition your child to adult care when they are ready.
-
Support for your whole family
- We are committed to your child’s overall health and well-being and to helping your child live a full and active life.
- Whatever types of care your child needs, we will help your family through this experience. We will discuss your child’s condition and treatment options in ways you understand and involve you in every decision.
- Our child life specialists know how to help children understand their illnesses and treatments in ways that make sense for their age.
- Seattle Children’s has many resources, from financial to spiritual, to support your child and your family and make the journey as smooth as possible.
- Many children and families travel to Seattle Children’s for heart surgery or other care. We help you coordinate travel and housing so you can stay focused on your child.
- Read more about the supportive care we offer.
-
Research to improve care
- Doctors at Seattle Children’s take part in national and international research to study less invasive ways to replace the pulmonary valve, if needed later in life, through cardiac catheterization. With these options, your child may be able to avoid further open heart surgery and recover faster.
Research and Clinical Trials
In the past, some children with tetralogy of Fallot needed open heart surgery later in life to put in a new pulmonary valve. Now, in some cases, we can do this through cardiac catheterization instead.
We use devices called the Melody, Harmony and Alterra transcatheter heart valves. This means we place a new pulmonary valve through a narrow tube directed into your child’s heart. This avoids open heart surgery and leads to quicker recovery.
The Heart Center team at Seattle Children’s took part in an early clinical trial that led to approval of the Melody valve by the U.S. Food and Drug Administration in 2010. Because of this research, we have a long history using Melody valves. We have more experience placing these valves than many other centers. In 2020, we completed a 10-year follow-up study checking outcomes in children who received a Melody valve.
Our doctors have also taken part in clinical trials of new transcatheter pulmonary valves, the Harmony valve and Alterra valve. These provide another option for teens and young adults who had surgery early in life for tetralogy of Fallot and who now need a pulmonary valve placed. Though the Harmony and Alterra valves are new, our Heart Center team has been offering them for years due to our role in research.
Contact Us
Contact the Heart Center at 206-987-2515 for an appointment, second opinion or more information.
Providers, see how to refer a patient.
Related Links
- Adult Congenital Heart Disease Program
- Cardiac Catheterization Procedures
- Fetal Center
- Heart Center
- Heart Surgery
- Hybrid Heart Procedures
- Seattle Children’s Heart Warriors: Charlotte (Video. 2:09)
- Statistics and Outcomes
Paying for Care
Learn about paying for care at Seattle Children’s, including insurance coverage, billing and financial assistance.

