Myelomeningocele
Contact the Neurosciences Center
What is myelomeningocele?
Myelomeningocele (my-elo-men-IN-go-seal) is a defect of the backbone (spine), spinal cord and spinal canal. Myelomeningocele (also called MMC) is the most serious form of spina bifida. In spina bifida, as a fetus grows during pregnancy, the coverings of the spinal cord do not close around the spinal cord as they should. This leaves the spinal cord open and unprotected.
This is how myelomeningocele forms in a developing baby during pregnancy:
- The coverings of the spinal cord do not form the normal way.
- A small sac containing parts of the spinal cord and nerves pushes through the opening(s) and sticks out the fetus’s back.
- Myelomeningocele can happen anywhere along the spinal cord. It is most common in the lower back.
- Nerves below the level of the MMC are damaged. This can affect your baby’s sensation, movement, and bladder and bowel control.
- Myelomeningocele higher in the spine may cause more severe symptoms.
Doctors do not know the exact cause of MMC. Research suggests that genes and nutrients during pregnancy play a role. Getting enough folic acid early in pregnancy can help prevent spina bifida. This B vitamin helps the baby’s neural tube grow properly into the brain and spinal cord.
Neurosciences Care at Seattle Children's
What are the symptoms of myelomeningocele?
In a baby with myelomeningocele, a sac holding parts of the spinal cord pushes out through their back. Myelomeningocele is most common in the lower back. The higher the MMC is on your baby’s spinal cord, the more nerve damage it causes.
Your child may have:
- Problems moving parts of the body below the opening in the back
- Lack of sensation in their legs and feet
- Poor or no bowel and bladder control
- Twisted or abnormal legs and feet, such as clubfoot
- A buildup of cerebrospinal fluid (CSF) in the head (hydrocephalus)
- Problems with how the back of the brain formed (Chiari 2 malformation)
- Learning differences or delayed developmental milestones
How is MMC diagnosed?
Most often, myelomeningocele is found during prenatal ultrasound scans. You may have other imaging (such as an ) to confirm the diagnosis.
If a doctor confirms your fetus has myelomeningocele, they may refer you to our Fetal Center. Our team will check your baby’s health and do imaging studies such as MRI (magnetic resonance imaging) and ultrasound. After a full assessment, we will advise you on what to expect.
Sometimes MMC is not diagnosed until after a baby is born, when the sac holding the spinal cord is seen pushing through the baby’s back. Your baby would then be transferred to a pediatric-focused center for next steps, such as surgery.
How is myelomeningocele treated?
Our Fetal Center team will work with your birth hospital to plan for a safe delivery and the special care your baby will need at birth. We’ll arrange your baby’s safe transfer to Seattle Children’s after they are born.
Surgery to repair the defect in your baby’s spinal cord is just the first step in their treatment. Your child’s NICU and neurosurgery teams will work closely with other experts at Seattle Children’s to assess all your child’s needs
Outlook for babies born with MMC
Each child is different. MMC - the most severe form of spina bifida - may affect your child their whole life. The location of the MMC on the spine matters. Myelomeningocele higher in the spine causes more severe symptoms. Spina bifida may affect your child’s mobility, bowel and bladder function, or sensation. Some children have other complex problems, such as spinal deformities, problems with how the lower part of the body develops (caudal regression), hydrocephalus, tethered spinal cord, Chiari malformation or syringomyelia.
Our Spina Bifida Program provides coordinated care from birth through 21 years. We will tailor treatment for your child and family. Depending on their conditions, your child may receive care from experts in Neurodevelopment, Neurosurgery, Nutrition, Orthopedics, Rehabilitation Medicine, Urology, Reconstructive Pelvic Medicine, Gastroenterology and Social Work. Our team will be with your family along this journey to help at each visit and prepare for the future. Each child is unique and will show us what they can do over time.
Surgery to Repair Myelomeningocele
Fetal surgery
In some cases, neurosurgeons can close the spinal defect during pregnancy. The surgery is done around the 24th week of pregnancy. The options are called fetoscopic myelomeningocele repair or in utero open MMC repair. Seattle Children’s does not offer fetal closure at this time, but may offer this surgery in the future.
If you choose to have your baby’s MMC repaired during pregnancy at another hospital, we will work with that hospital to coordinate your baby’s care. Some women deliver their baby at the center that performed fetal surgery. Others return to Seattle for delivery and then the baby transfers to Seattle Children’s right after birth. Regardless of delivery location, Seattle Children’s can provide your baby’s ongoing health care related to spina bifida.
Surgery after birth
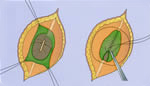 Closing the spinal cord defect in spina bifida.
Closing the spinal cord defect in spina bifida.We work closely with your birth hospital to safely transfer your baby to Seattle Children’s soon after they are born. Within your baby’s first 48 hours of life, the neurosurgeons and plastic surgeons work as a team to repair the myelomeningocele in the operating room. This:
- Protects the spinal cord
- Limits the risk of infection
- Prevents more damage to the spinal cord but does not restore damaged nerves
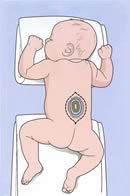
The child is in position for the repair of his spina bifida.
During surgery:
- First, the neurosurgeon closes the covering around the spinal cord.
- Next, the neurosurgeon and plastic surgeon close the muscles and fascia over the spinal cord.
- Finally, they close the skin over the open area.
Treating Related Conditions
Some children with myelomeningoceles have other conditions that need treatment, such as:
- Hydrocephalus, where too much cerebrospinal fluid collects in their head and puts pressure on their brain. Most often, neurosurgeons place a tube (called a shunt) in the skull to drain CSF to another part of the body, where it is absorbed.
- Tethered spinal cord, where the spinal cord is pulled down and stuck to the spinal canal instead of floating freely inside it.
- Chiari malformation, a problem with the way parts of the brain are shaped and how they sit in the skull. Parts of the brain hang down through the opening in the base of the skull into the upper neck.
- Syringomyelia, a cyst in the center of the spinal cord that is filled with fluid. This can put pressure on the spinal cord and cause nerve damage.
Ongoing Myelomeningocele Care
Our Spina Bifida Program cares for children born with spina bifida from birth through 21 years of age. We design a treatment plan just for your child, to meet their needs over the long term.
Seattle Children’s is designated as a Clinic Care Partner by the Spina Bifida Association (SBA), the national leader in providing research, education, support, clinical care and advocacy to all those affected by spina bifida. The SBA Clinic Care Partner program identifies clinics with the best outcomes for people with spina bifida. As an SBA Clinic Care Partner, we follow best practices and provide the best care possible to help the children and young adults we treat have fulfilling lives.
MMC can affect your child’s movement, sensation, bowel and bladder control, or learning.
- Our Neurodevelopmental experts work with your child to help manage any they may have. Our multidisciplinary team works together to help your child thrive at home, in school and in your community.
- Nerve damage often limits movement. If your child has mobility problems, our Orthopedics, Orthotics and Rehabilitation Medicine specialists will work with your child to meet their needs. Treatment options include orthopedic surgery, physical therapy, occupational therapy and aids like braces, crutches or wheelchairs.
- Some children born with myelomeningocele have differences in their legs, feet, hips or spine. Your child may have orthopedic surgery for problems like clubfoot, curved spine (scoliosis), contracted muscles or dislocated hips.
- Most children with myelomeningocele develop hydrocephalus and need a shunt. Our Neurosurgery team will keep watch over your child to make sure the shunt keeps working well all during childhood.
- In many kids with spina bifida, their bladder does not work normally, because their spinal cord and the nerves that control the bladder did not form correctly before birth. This can affect how their kidneys work, their ability to pee and their quality of life. Seattle Children’s takes part in a nationwide study (UMPIRE) to evaluate the best ways to manage bladder and kidney issues for newborns and young children with spina bifida.
- To address bowel and bladder issues, your child may see specialists in Neurodevelopment, Rehabilitation Medicine, Urology or Gastroenterology.
As they reach adulthood, we help your child transition to a provider who cares for adult patients.
Why choose Seattle Children's for myelomeningocele care?
 Seattle Children’s has been a leader for 50 years in providing complete, coordinated care for children with myelomeningoceles.
Seattle Children’s has been a leader for 50 years in providing complete, coordinated care for children with myelomeningoceles.
- If myelomeningocele is detected during pregnancy, specialists at our Fetal Center will assess your baby’s health to prepare for their birth and care. If you choose to have fetal surgery during pregnancy, we will coordinate care with the hospital of your choice.
- We work closely with your birth hospital and are national leaders in safely moving fragile newborns. Within 1 to 2 days after birth, our skilled neurosurgeons will repair your baby’s spinal defect.
- Our Level 4 (IV) Neonatal Intensive Care Unit (NICU) team is skilled and equipped to care for the sickest newborns. We provide specialized care in our Neuro NICU — the only neonatal neurocritical care program in Washington, Wyoming, Alaska, Montana and Idaho.
- Children with this form of spina bifida often need care for other complex problems. We have a great deal of experience caring for these conditions, such as spinal deformities, hydrocephalus, tethered spinal cord, Chiari malformation and syringomyelia.
- Nerve damage from MMC can affect your child their entire life. Our Spina Bifida Program provides ongoing medical and developmental care to children from birth through 21 years of age. Our team includes experts in Neurodevelopment, Neurosurgery, Nutrition, Orthopedics, Rehabilitation Medicine, Urology and Social Work.
- Your child will benefit from innovations developed at Seattle Children’s to make treatments safer and more effective. Our patients have the option to take part in clinical trials of promising new therapies. Learn about participating in clinical trials at Seattle Children’s.
"Out of all the priceless gifts our care teams have given us, there’s one that sustains us: the simple belief that our son has boundless potential.” - Whitney Stohr, mom of Malachi, who was diagnosed with myelomeningocele during pregnancy. Today, he’s thriving. Read Malachi's story.
Contact Us
If you would like an appointment, ask your obstetrician or maternal-fetal medicine doctor for a referral. If you have a referral, call 206-987-2016 to make an appointment.
Providers, see how to refer a patient.
If you have questions, contact us at 206-987-2016 or 844-935-3467 (toll free).
Paying for Care
Learn about paying for care at Seattle Children’s, including insurance coverage, billing and financial assistance.

