
Healthy Tides
Healthy Tides is a free email newsletter for parents and caregivers of babies, children and teens. Subscribe to receive health and safety information and Seattle Children's news six times each year.
Featured Articles
Subscribe to get our newsletter in your inbox!
Latest Articles
Search Results
-

The Breakthrough Cancer Treatment and Relentless Determination That Changed Ino’s Life
Read Ino’s inspiring cancer journey and discover how cutting-edge treatments and pediatric clinical trials are providing hope, compassionate care and life-saving cures to children, teens and young adults across the Pacific Northwest.
-

Your Child’s Mental Wellness: 5 Actions You Can Take
Support your child or teen’s mental wellness with these 5 easy actions from the experts at Seattle Children’s.
-

Sneaky Sodium is Hard on the Heart
Learn where sodium hides, how to reduce sodium intake and why it matters to your child or teen’s health.
-

Care Without Barriers – Seattle Children’s Pilots Spanish-Language O.R.
Seattle Children’s held its first ever all-Spanish-speaking operating room (O.R.) day where patients and families received care at every step in their native language from surgeons, nurses, and other staff members who are fluent in Spanish. Learn more about language-concordant care.
-

Home Is Where Shirley’s Heart Expert Is
Diagnosed by Seattle Children's prenatal specialists before birth, Shirley underwent open-heart surgery when she was just five days old. Now she's an active 8-year-old who has heart check-ups at Seattle Children's South Sound Cardiology Clinic, saving her family time with expert care close to home.
-

Athletic trainers aren’t just for the pros. Learn the many ways they support young athletes.
-

Sleepwalking and Sleep Terrors During Childhood
Dr. Maida Chen explains two sleep issues that can impact your whole household and shares how to best handle them.
-

Seasonal Allergies or Something More? Seattle Children’s Helps Parents Distinguish the Difference
Stuffy nose, sneezing, and itchy or watery eyes are a few indications that a child may be suffering from allergies. These symptoms are most often triggered during the spring and summer months but it can sometimes be tough to differentiate the cause among other illnesses that tend to spread this time of year.
-
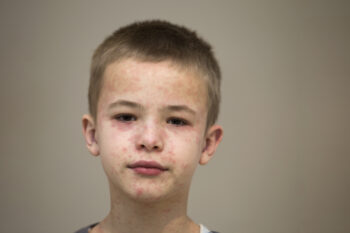
How to Protect Your Family and Community During a Measles Outbreak
Learn about measles from Dr. Danielle Zerr. Understand symptoms, risks and vaccination importance to protect your family and community.
-

Tweens, Teens and Young Adults Need Checkups Too
Dr. Cora Collette Breuner explains the importance of these adolescent and young adult wellness visits and provides the advice for parents.
-

From Star Athlete to Head Coach: How Lyla’s Medical Experience Inspires a Team Culture of Safety
Lyla’s medical experience inspires a team culture of safety. Read her story and get injury prevention tips.
-

Child Life Specialist Shares Tricks of the Trade to Help Kids Cope
Learn how to maximize your child or teen's coping and minimize their stress during medical procedures, from needle pokes to surgery.
-

The Sick Day Guessing Game: Cold, Flu, RSV or COVID-19?
Get advice for preventing and treating colds, flu, RSV and COVID-19.
-

If you’re a parent, you may be wondering how this change could impact your kids as they adjust to school schedules, weekend activities and most importantly, their sleep and health management.
-

Dr. Tony Woodward, chief of Emergency Medicine at Seattle Children’s, offers tips for how to safely celebrate what many kids consider to be the best holiday.
-
Fire Escape Plans: Could Your Family Get Out in Two Minutes?
This National Fire Prevention Week, Seattle Children's urges families to make and practice a home fire escape plan. Get tips and resources to do this important safety planning.
-

A Gift of Life, Health and Hope for Hailee After Life-Altering Diagnosis
Discover how Hailee’s life was transformed through community generosity and compassionate care at Seattle Children’s Hospital.
-

Miracle Babies: A 700-Mile Journey to Face the Odds
A referral to the Maternal Fetal Intervention and Surgery Program at Seattle Children’s started a journey that would save their babies’ lives.
-

My Journey From Sickle Cell Disease to Healing
John Masembe shares how having sickle cell shaped his life and brought him back to Seattle Children’s Sickle Cell Disease Program at OBCC as a team member.
-

Getting Beyond ‘How was your day?’
Getting children, tweens and teens to fill you in on their day isn't always easy. Get tips for how to engage your child in meaningful conversation.
-

From Patient to Mother: Two Generations of Care
New mom finds support and care at OBCC. Learn how this clinic helped a preemie thrive.
-

How to Handle a Difficult Prenatal Diagnosis
Seattle Children's Hospital genetics counselor, Kiana Siefkas, offers parents advice to help cope with an unexpected prenatal test result.
-

Seattle Children’s Shares Advice on Reducing Back-to-School Worries
Co-directors of the Mood and Anxiety Program at Seattle Children’s offer ways parents and caregivers can help reduce worries in children as they head back to school.
-

In an immersive therapeutic gaming experience only possible at Seattle Children’s, patients now have a one-of-a-kind opportunity to explore the hospital through the virtual world of Minecraft.
-

Researching the Far-Reaching Effects of Wildfire Smoke – Ways to Protect Kids Against Air Pollutants
Dr. Mary Crocker, pediatric pulmonologist and researcher at Seattle Children’s Research Institute’s Center for Respiratory Biology and Therapeutics, shares insights into her research and the patterns she’s seen reflected in the pediatric community as wildfire conditions continue to change.
-
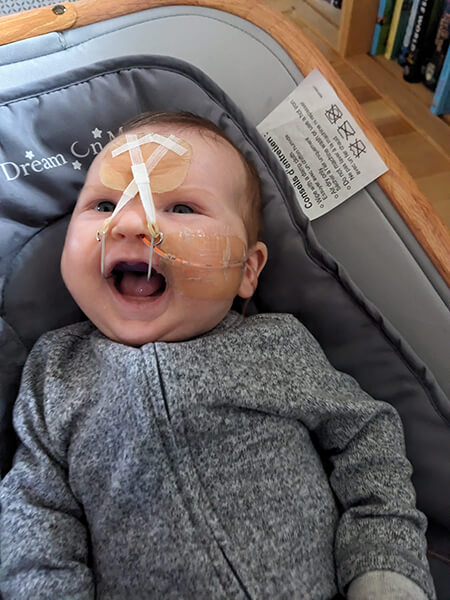
How a Unique Therapy at Seattle Children’s for a Rare Craniofacial Condition Helped Baby Milo Thrive
The orthodontic airway plate (OAP), also called the Tübingen palatal plate, is an oral appliance that is custom-crafted with expertise from an orthodontist and an otolaryngologist (ENT). The OAP is removable and designed to position a baby’s tongue forward and open the airway to help them breathe, feed and grow.
-

Generosity Reflected in a Child’s Life
Seattle Children’s has the most generous financial assistance program in the Washington, Alaska, Montana, Idaho (WAMI) region, providing more than $375 million of care not covered by insurance or Medicaid last year. Community support for the Uncompensated Care Fund is vital.
-

Learn how Seattle Children’s specialized care team left no stone unturned to provide the best leukemia care in the Pacific Northwest for Seeley.
-

Choose Safe Fun for the Fourth of July
Seattle Children’s Dr. Tony Woodward advises on Fourth of July safety. Learn about firework, water and food safety for a fun holiday.
-

It Takes a Village: Siobhan’s Journey With Arthrogryposis and the Power of Community Support
16-month-old Siobhan is a typical toddler in many ways. But her journey hasn't been that of a typical toddler. Diagnosed with arthrogryposis multiplex congenita (AMC), a condition characterized by multiple joint contractures, Siobhan has been treated at Seattle Children’s since she was 4 weeks old.
-

Seattle Children’s Physicians Headed to the Paris 2024 Olympics Answer Top Sports Medicine Questions
Olympic athletes competing at the highest level need the most experienced and dedicated health care providers by their side. That’s where Dr. Brian Krabak and Dr. Monique Burton, of Seattle Children’s, the Odessa Brown Children’s Clinic (OBCC), and the University of Washington (UW), come into play.
-

A Resource for Finding Mental Health Care for Children and Teens
Washington’s Mental Health Referral Service for Children and Teens connects families with mental health and behavioral health providers in your community who accept new patients, work with your insurance and are a good match for your child’s treatment needs.
-

Fatherhood, When Your Son Has Cancer
Dennis Williams shares his experience being a father of a son diagnosed with cancer at Seattle Children's and a message to other families of children with cancer.
-

‘I Have Celiac Disease, and My Life Is Delicious!’
Celiac disease limits what 12-year-old Celia can eat but not what she can achieve. Celia details her life without gluten and how she supports newly diagnosed kids with the disease.
-

Spring Sports Safety – 10 Tips for Staying in the Game
Spring sports are back! Learn about common injuries, preventive measures, and how to keep kids safe while playing baseball, tennis, lacrosse, soccer, and track.
-

Where to Turn When Preparing for Your Child’s Hospital Stay
Social workers can help families with many aspects of a hospital stay, from providing emotional support to more tangible needs like insurance and financial assistance.
-

Craniofacial Experts from Seattle Children’s Make Global Impact for Kids with Cleft Lip and Palate
Seattle Children’s Craniofacial Center experts are looked at locally, regionally and internationally to provide their unique expertise and support in cleft lip and palate care.
-

Animal Safety: Teach Kids Smart Habits Around Animals
Dr. Tony Woodward, Chief of Emergency Medicine at Seattle Children’s Hospital, offers advice and tips to families about keeping kids safe around animals.
-
Layers of Protection for Safe Water Fun
A series or two of swim lessons is not enough. More skills and more attention are needed to help make your family’s time around the water safe and fun.
-

Heart-Healthy Habits for Families
Dr. Jason Deen, a cardiologist at Seattle Children’s, to provide tips for families who want to make heart-healthy choices.
-

Blood Donation: Eight Things to Know
Learn how donating blood can save lives. Quick, easy, and safe process. Find a donation center near you.
-

Positive Changes for the New Year: Resolutions for Families
Ideas for families to consider as they take steps for better health, safety and wellness in the new year.
-

Tips for Staying Safe on the Slopes
Dr. Tony Woodward, medical director of Emergency Services at Seattle Children’s, offers tips to help kids enjoy the slopes safely.
-

Is it Growing Pains or Something More?
Learn about the causes of growing pains, symptoms, why they affect some children and not others, and when to call your child's doctor.
-

Coins, Blow Darts and Button Batteries: The Diary of an Otolaryngologist
Dr. Kathleen Sie emphasizes awareness of dangerous household items that can end up in children’s ears, noses, or throats offering advice for parents and caregivers to keep their kids safe.
-

Doctor Offers Tips to Prevent Overuse Injuries
To help keep kids healthy and active this season, here are tips for parents and coaches to make sure pain isn’t a part of a child’s sports season.
-

Doctor Explains Why Osteoporosis is a Pediatric Disorder, the Importance of Vitamin D
Osteoporosis is actually a pediatric disorder and by thinking about bone health at an early age, individuals can ensure they have strong bones later in life.
-

Discover the pervasive impact of added sugar in everyday foods beyond desserts and candy. Learn about health risks and recommended limits.
-

Debunking Three Common Myths About Eczema
Debunking common myths about eczema: It’s not always caused by allergens, regular bathing is okay, and treatment is essential for children’s well-being.
-

Making SMART New Year’s resolutions as a family
Making resolutions as a family can be a wonderful activity, but it’s important to think them through first before setting them in stone.
-

Doctor offers tips to keep kids safe this holiday season
To keep kids out of the emergency room this year, Dr. Tony Woodward recommends some basic safety tips to ensure an injury-free, but still festive holiday season.
-

“I’ll Have Scars, Too”: A Father-Son Bond More Than Skin Deep
Ryder's life was saved by a 12-hour surgery at Seattle Children’s. His father, Thomas, got a tattoo in solidarity with Ryder, matching the scar from his medical journey.
-

The Race to Save Sirish’s Brain
Sirish unexpectedly began developing seizures at age 11. Learn how teams at Seattle Children’s helped to protect his brain.
-

A New Neurosurgical Procedure is Bringing Promising Seizure Relief to Some Epilepsy Patients
Deep brain stimulation offers hope for children with epilepsy. Seattle Children’s leads in providing this life-changing treatment, reducing seizures by up to 50%.
-

Innovative Epilepsy Procedure Offers New Avenue of Treatment to Reduce Seizures
A cutting-edge procedure for epilepsy at Seattle Children’s, known as responsive neurostimulation (RNS), is offering hope and seizure reduction relief to some patients who are still looking for solutions after exploring other treatment options.
-

An Awake Brain Surgery at Seattle Children’s Stops Jasmine’s Seizures
Jasmine's journey: from Alaska to Seattle Children's for a life-changing surgery to remove a brain tumor and stop her seizures. A story of hope and healing.
-

Pride Month and Beyond: Finding Hope and Caring for All Kids
As Pride Month begins, legislation targeting LGBTQ+ rights emerges. Learn about the impact on gender-affirming care and Seattle Children’s Gender Clinic.
-

Highlights from across Seattle Children's Research Institute: equity initiatives improve infection rates; cell and gene therapy progress; malaria.
-

Discover how high school student Rocky Srinivasan's research on amino acids led to a nonprofit supporting orthopedic research and a book on scientific advancements.
-

Seattle Children’s Lead DIPG Researcher Attends Brain Cancers Forum at The White House
The White House recently convened patients, caregivers, oncologists, researchers and administration officials for the Cancer Moonshot Brain Cancers Forum to advance progress for patients with glioblastoma (GBM) and diffuse intrinsic pontine glioma (DIPG).
-

‘You Are a Miracle’: One Patient’s Journey with an Eating Disorder
Emme shares her personal experience at Seattle Children’s – from diagnosis to ongoing recovery, and the lessons learned along the way.
-
Antibiotic Resistance: Too Much of a Good Thing
Learn about the importance of appropriate antibiotic use, what antibiotic resistance is, and what we can do about it.
-

PedAL Initiative ‘Dares’ to Transform Treatment and Care for Kids with Blood Cancer
Seattle Children’s leads the PedAL Master Trial, a groundbreaking global initiative focused on transforming treatment for pediatric acute leukemia, offering new hope with tailored therapies beyond standard chemotherapy.
-

Partnering with Biotechs to Save Lives
Seattle Children’s spin-out, GentiBio, partners with Bristol Myers Squibb in a multi-year collaboration, marking another milestone in the institute's efforts to develop life-changing therapies for children.
-

Leaving “No Stone Unturned” for Children with High-Risk Leukemia
Seattle Children’s High-Risk Leukemia Program brings together a team of top experts in all disciplines specific to a child’s unique high-risk leukemia needs to provide seamless, coordinated care from day one.
-

Read about Isaac as his dad shares how he and his family coped after his 17-month-old son was diagnosed with stage-4 cancer at Seattle Children’s that had spread through his tiny body.
-

Community Gathers to Cheer for Mercy on Her Way to Seattle Children’s for Last Round of Chemo
Follow Mercy's inspiring journey from fundraising for cancer research to her own battle with Hodgkin lymphoma at just 16. Her resilience, community support, and determination shine through as she fights cancer and dreams of becoming a cancer researcher.
-

Aliyanna Overcomes the Odds, Celebrates Her Second Birthday with Her Care Team
One mother's joy of expecting a baby girl turned to heartbreak when doctors discovered a cancerous growth on her daughter's spine during an ultrasound. Facing tough odds, she survived and is thriving.
-

Six Years Later: Immunotherapy’s Tiniest Trial Participant Is Living With “So Much Joy”
Maggie and Andy Oberhofer share their journey of hope and resilience as they turn to a groundbreaking cancer immunotherapy trial at Seattle Children’s to save their daughter Greta from relapsed leukemia.
-

Global Clinical Trial Aims to Improve Therapies for Pediatric Acute Leukemia
Seattle Children’s and The Leukemia & Lymphoma Society (LLS) are teaming up for a new global trial to improve treatments for kids with relapsed leukemia. Led by Dr. Todd Cooper, the trial will use advanced testing to find better treatment matches, giving hope for improved care.
-

Child Life Specialists Help Patients and Families Cope During Uncertain Times
Seattle Children’s Hospital remains a beacon of hope, where child life specialists like Riley Coyle turn challenges into uplifting experiences. Discover their enduring commitment to compassion and excellence.
-

How Seattle Children’s Turned One Family’s Devastation Into Hope
Seattle Children’s Prenatal Diagnosis and Treatment Program helped the Fannin family move toward a bright future after a routine ultrasound showed that their baby had a congenital diaphragmatic hernia (CDH).
-

Kawasaki Disease in Children With COVID-19
Dr. Michael Portman, pediatric cardiologist and director of the Kawasaki Disease Clinic at Seattle Children’s, explains concern that children with COVID-19 developed mysterious symptoms that mimic Kawasaki disease.
-

Baby Battles Fatal Heart Condition and Comes Out Unstoppable
Follow the inspiring journey of Nevaeh, born with hypoplastic left heart syndrome. Learn about her surgeries, milestones, and unstoppable spirit.
-
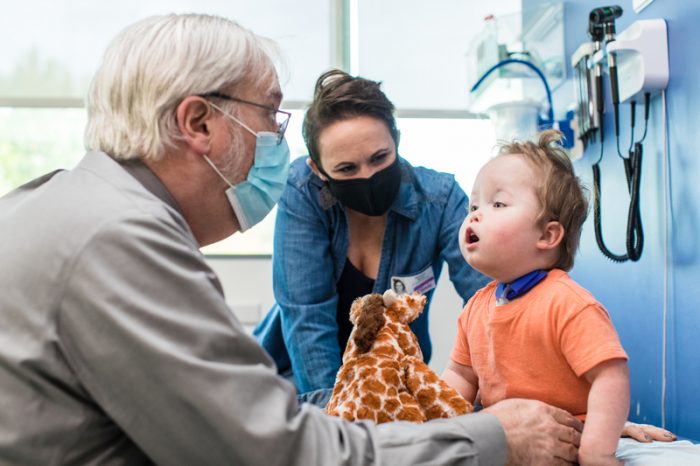
Malachi Stohr Is “Absolutely Amazing”
Witness Malachi’s inspiring journey with spina bifida. From harrowing moments in the PICU to the joy of milestones, find strength in his story.
-

Minimally-Invasive Imaging and Laser Surgery Solve Elusive Epilepsy
Giorgia, 11, is among the 20 to 30% of children with epilepsy whose seizures do not respond to medication. Read how a minimally-invasive surgery got her back to living like a kid again.
-

From Stunning Diagnosis to Unexpected Hope: MEK Inhibitor Proves Amazing for Grace
Discover Grace's remarkable journey battling neurofibromatosis type one. From devastating falls to unexpected hope, thanks to MEK inhibitor.
-

How the OBCC Team Is Stepping Up, and Out, to Help During the Pandemic
The team at OBCC helped about 400 families by providing food security, financial resources, hygiene and family support thanks to partnerships with local food banks, Safeway, the Cliff Avril Family Foundation and other nonprofits.
-
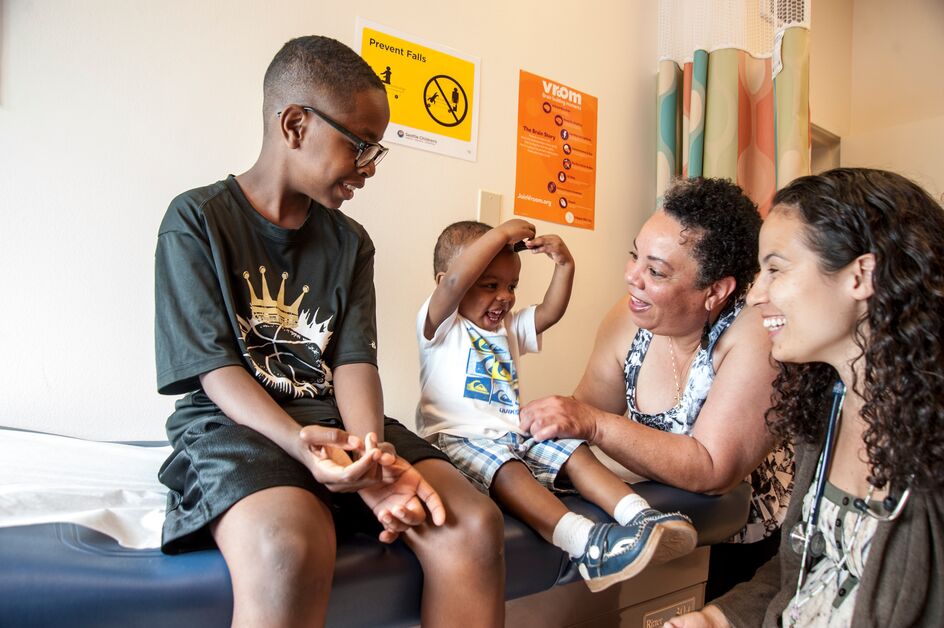
Boeing Donates $2.5 Million to Help Fund Vital Programs at OBCC
Today, Boeing has committed to investing $2.5 million to help fund vital programs at OBCC and a new, second OBCC to better serve under-resourced, ethnically diverse communities.
-

Families Raise Awareness of Rare, Underdiagnosed Lung Disease
Discover the courageous journeys of Isabelle and Elliot, both battling primary ciliary dyskinesia (PCD), and a researcher seeking better cures and treatments for kids like them.
-

Researchers Ready B Cells for Novel Cell Therapy
Scientists at Seattle Children’s Research Institute are paving the way to use gene-edited B cells to treat a wide range of potential diseases that affect children.
-

Returning to Sports Safely During COVID-19
Learn how to safely reintegrate your child into sports and activities post-COVID-19, providing peace of mind throughout the process.
-

Knox’s Heartfelt Care at Seattle Children’s Leaves Lasting Impact on Wenatchee Family
Discover how Seattle Children’s Fetal Care & Treatment Center provided expert care for Knox’s SVT, ensuring a healthy start to life. Read his inspiring journey now!
-

Seattle Children’s Experts Explain Why Kids and Teens Should Avoid Energy Drinks
Learn about the risks of energy drink consumption for children, including the dangers of caffeine and added sugars, and discover healthier hydration choices.
-

Are Children Making Antibodies That Will Protect Against Future COVID-19 Infections?
Discover how Dr. Janet Englund and Seattle Children’s Research Institute study COVID-19 in children, assessing antibodies and immunity.
-

Can a Greater Understanding of COVID-19 in Children Reduce the Overall Impact of the Coronavirus?
Dr. Leslie R. Walker discusses understanding COVID-19 in children to reduce its overall impact. Research efforts focus on immunological responses and potential vaccine development.
-
Scientist Develops New Way to Test for COVID-19 Antibodies
Discover Dr. Stephen Smith's groundbreaking method to test for COVID-19 antibodies, providing a reliable way to quantify immunity.
-

Hundreds gathered in Seattle’s Central District neighborhood to celebrate the Odessa Brown Children’s Clinic’s (OBCC) future location on 18th Ave. S. and S. Jackson St.
-

Celebrating Wizards of the Coast’s Generous Commitment of $5M to Seattle Children’s Autism Center
Seattle Children’s honored Wizards of the Coast for their $5M commitment to Seattle Children’s Magnuson by naming the Autism Center registration area and main waiting room.
-

Stage's diagnosis of mitochondrial myopathy brought unforeseen financial strain to his family. With Seattle Children’s Uncompensated Care program, funded by donations, they found relief, focusing on his care rather than financial worries.
-

Seattle Children’s Patients Get VIP Experiences at MLB All-Star Game
Two Seattle Children’s patients get once-in-a-lifetime experiences as a part of the festivities leading up to the MLB All-Star game thanks to MLB and MLB All-Star partners DQ and CMN.
-

Learn about the latest breakthrough in RSV prevention: a CDC-recommended vaccine for pregnant individuals. Led by Seattle Children’s researchers like Dr. Janet Englund, these studies show promising results in preventing RSV disease and hospitalizations in infants.
-

Learn about cyberbullying and how to protect your kids online. From spamming to doxxing, understand the different forms and how they can affect your child.
-

Summer Safety Reminders for Parents and Caregivers of Young Children
On the Pulse shares reminders to help keep young children safe from window falls and illness or death from being left in a hot car.
-

From Crisis to Happy Chaos: How Teamwork Made All the Difference
A family's inspiring journey overcoming crisis and embracing joy, featured on Seattle Children's Healthy Tides blog.
-

Dr. Molly Taylor is both a Seattle Children’s oncologist and a researcher who serves patients with cancer by studying how the body and mind intersect to impact survival.
-

From Feeling Helpless to Helping Others: Kinsey Dreams Big
From battling cancer to mental health advocate: Kinsey's journey inspires. With support from Seattle Children’s, she now pursues a career in pediatric mental health.
-

Honoring the Legacy of Dr. Peter Mansfield, Former Seattle Children’s Chief of Surgery
In honor of the late Dr. Peter Mansfield, former Seattle Children’s Chief of Surgery, his wife, Jackie Mansfield, has established a fund directly benefitting the Invent at Seattle Children’s Postdoctoral Scholars Program.
-

9 Questions Answered about Clinical Trials by a Seattle Children’s Cancer Expert
Dr. Tyler Ketterl, medical director of Seattle Children’s programs in Adolescent and Young Adult Oncology and Comprehensive Fertility Care and Preservation, to explain the basics of cancer clinical trials.
-

“At 17, My World Completely Changed”: Two-Time Cancer Survivor Shares Her Path to Wellness
Emma, a second-year grad student in health sciences, faced Hodgkin’s Lymphoma with determination. Seattle Children’s experts provided treatment, including fertility preservation.
-
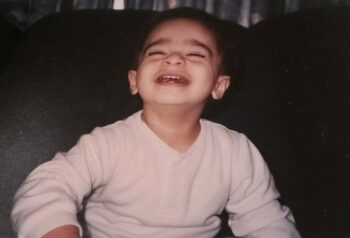
Family’s Pursuit of Hope and Better Medical Care Leads Them to Seattle Children’s
One Seattle Children’s patient shares their personal experience traveling across the world for medical care, navigating language and education barriers, and finding strength in transition.
-

Seattle Children’s Patients Help Create Out of this World Art Spacesuit
As part of a unique space-themed art project, Seattle Children’s patients are designing an art spacesuit that may one day have the opportunity to fly to space.
-

Seattle Children’s launches BrainChild-04, a groundbreaking phase 1 clinical trial targeting four antigens with CAR T-cell therapy directly to the brain for children with rare and recurrent brain tumors.
-

Read how Jiana's family navigated a rare neurological condition, hemimegaloencephaly, and opted for life-changing surgery at Seattle Children’s.
-

Amidst Ellia’s Cancer Treatment, the Yees Found a Way to Help Others
Ellia's inspiring battle against pediatric leukemia at Seattle Children’s inspires her family's fundraising efforts to support research, resulting in a transformative impact of on high-risk leukemia treatments.
-

More Than a Paycheck: Seattle Children’s Summer Scholars Program Provides Path to Science Careers
Seattle Children's Research Institute's Summer Scholars Program gives college students hands-on research experience alongside seasoned scientists, fostering career growth and promoting diversity in biomedical research.
-

Just How Bad Is Social Media for Youth Mental Health?
Dr. Yolanda Evans shares social media's impact on youth mental health, guiding parents to protect children and offering resources.
-
Top 10 Questions Kids Ask Before Surgery
A pediatric surgeon at Seattle Children’s, answers some of the most common questions he gets asked by patients and families before surgery.
-

Childhood Tics: Will My Child Outgrow Them?
Gain understanding and support for childhood tics with Dr. Dararat Mingbunjerdsuk. Find reassurance, diagnosis guidance, and essential resources.
-

‘Boys Will Be Boys:’ The Negative Effects of Traditional Masculinity
Gain insights from Dr. Tyler Sasser on redefining masculinity for healthier outcomes. Understand societal pressures and learn practical parenting strategies.
-

The 5 Most Common ADHD Questions Asked by Parents
Dr. Erin Gonzalez answers some of those most commonly asked questions by parents and caregivers of adolescents diagnosed with ADHD.
-

Children’s Soy Consumption Linked to Increased Kawasaki Disease Risk
Discover the risks of high soy consumption in children. Dr. Michael Portman's research sheds light on soy's link to Kawasaki Disease.
-

Mother of Micro Preemie Twins Shares NICU Advice
Amelia and Calvin are true fighters, overcoming the odds from birth as micro preemies. Their mom, Amanda, shares their family's experience in Seattle Children's NICU, along with advice for other parents.
-

7 Tips to Manage Your Child’s Routine During the Holiday Season
Discover expert tips on managing holiday stress for kids. Prioritize routines, set limits, and cherish family moments.
-
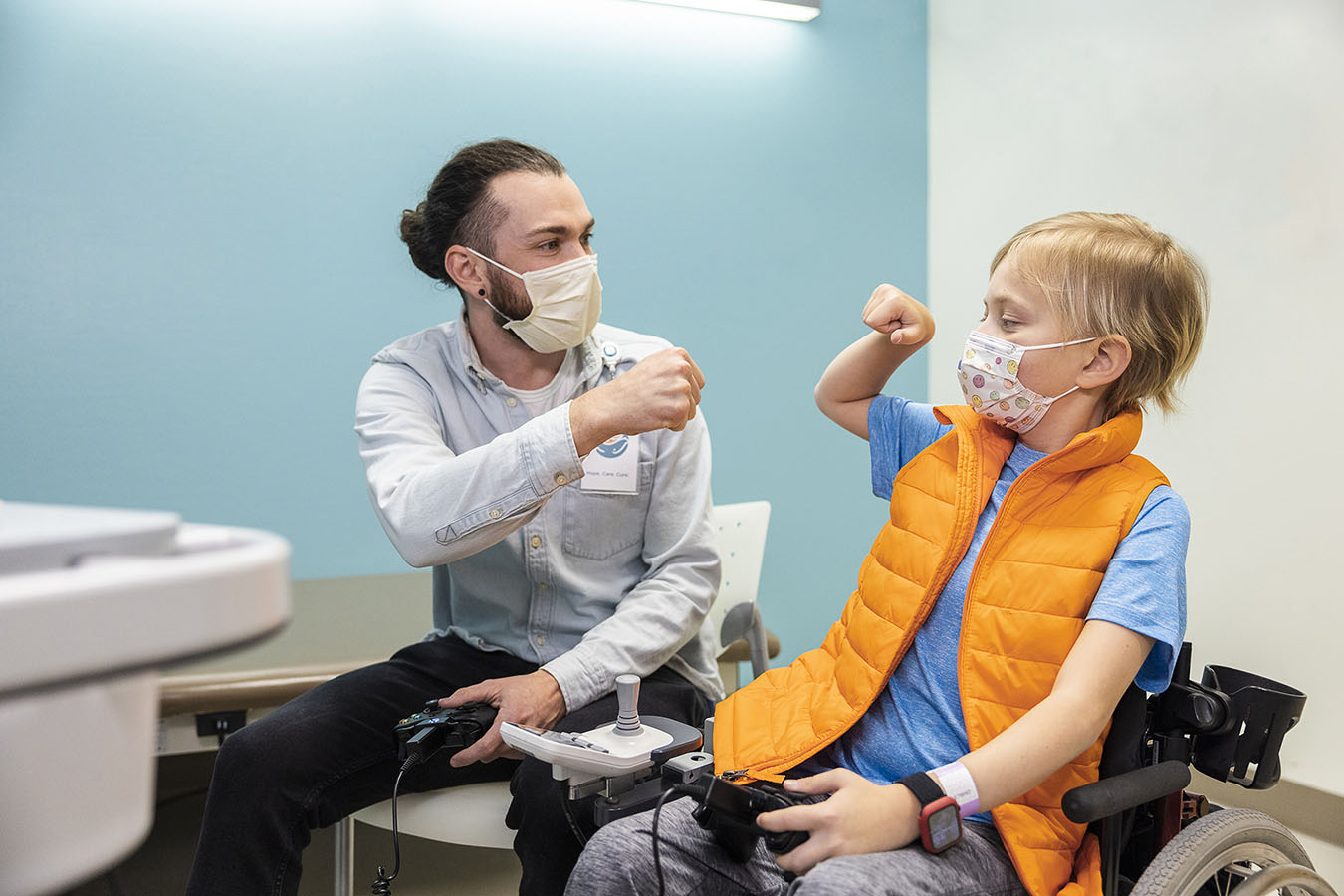
Tips for Raising Heart-healthy Kids and Teens
Seattle Children’s providers share their tips for helping kids and teens build strong, healthy hearts.
-

Anxiety and Depression: The Most Common Questions Asked by Parents
Discover the key differences between anxiety and depression in children, common symptoms, treatment options, and when to seek help in this comprehensive guide from Seattle Children’s.
-

Neonatal Telehealth Takes Geography out of the Equation to Save Lives
Experience the miraculous journey of baby Maleila, whose life was saved by cutting-edge telehealth technology. Join her mother, Kelsey, as she recounts the harrowing moments and the incredible strength of her daughter.
-

Fighting to Give Every Child With Cancer a Chance to Become a Parent
Explore how Seattle Children’s urologist Dr. Margarett Shnorhavorian is revolutionizing fertility preservation for childhood cancer survivors like Taylor.
-

Living the Movie Wonder: How 13-Year-Old Nathaniel Found Freedom, Inspires Kindness
The movie “Wonder” sheds light on a rare craniofacial condition, Treacher Collins syndrome. Nathaniel and his family have no trouble relating to the storyline; they live it every day.
-

How Violence in Video Games and Media Harm Child Development
AAP's report urges reducing children’s exposure to violent media. Children are not only viewing violence, but with virtual reality games they are actively engaging in a realistic and immersive violent experience.
-

Seattle Children’s Therapeutic Gaming Program brings the power of video games, virtual reality and other therapeutic technology to enhance patient experiences and improve outcomes.
-

Students from Yale University Serenade Seattle Children’s Patients and Families
Seattle Children’s patients, families and staff were surprised by a pop-up performance from students in Yale University’s a cappella group, Mixed Company.
-

State to Use Dr. Sihoun Hahn’s Newborn Screening Test for Wilson Disease
Dr. Sihoun Hahn has pioneered a novel test to detect Wilson disease as part of newborn screening and to confirm cases that are hard to diagnose.
-
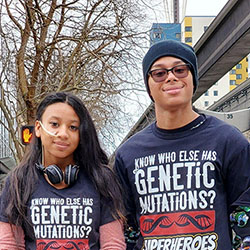
One Family, Two Children and a 16-Year Quest for Answers
After taking their children to countless specialistsfor over 15 years, family finally gets answers and a path forward thanks to Seattle Children's Biochemical Genetics team.
-

Seattle Children’s Alyssa Burnett Adult Life Center Celebrates 10 Years
Learn how Seattle Children's Alyssa Burnett Adult Life Center and the community celebrated ten years of learning, connection and fun.
-

How to Do “Mental Health Check-Ins” With Your Child
Dr. Yolanda Evans, head of the Division of Adolescent Medicine at Seattle Children’s, and a parent herself, shares what mental health check-ins are and how can they be done effectively.
-
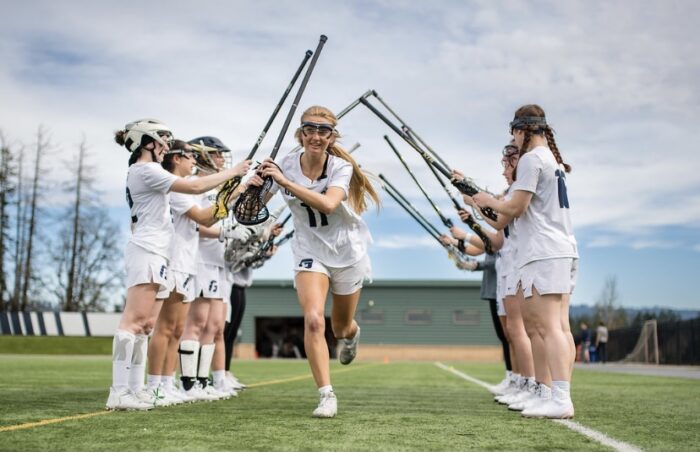
When Life Threw Lyla a Curveball, Seattle Children’s Helped This Athlete Get Back Out on the Field
A passionate lacrosse athlete with adolescent idiopathic scoliosis (AIS) got back in the game after spine surgery at Seattle Children's.
-

‘I Want to Hold Your Hand’: Two Generations Find Joy at the Alyssa Burnett Center
Established in 2014 thanks to generous giving, Seattle Children's Alyssa Burnett Center spreads joy to families like the Zenters.
-

In celebration of Autism Acceptance Month, Seattle Children’s Autism Center and Seattle Children’s Alyssa Burnett Adult Life Center students and families surprised by Seattle Seahawks mascot, Blitz.
-
Prescription Opioids and Pain Relief in Teens
Dr. Gary Walco of Seattle Children’s addresses opioid misuse among teens post-surgery. Learn risks, prevention, and safe prescribing practices.
-

Treatment Helps Kids and Teens Control Anxiety
Dr. Kendra Read from Seattle Children’s offers insights into anxiety in children and teens. Learn about symptoms, treatment, and tips for parents.
-

Smooth Milestone Transitions for the New School Year
Dr. Cora Collette Breuner from Seattle Children’s offers tips for transitioning back to school. Prepare for preschool, kindergarten, middle, and high school.
-

Safe Travel Tips for Active Families on the Go
Dr. Beth Ebel from Seattle Children’s provides essential tips for staying safe while on the move. Learn pedestrian, bike, and car safety practices.
-

Traditions, whether faith-based or not, teach values, build relationships, foster belonging, and create positive memories, impacting children's lives.
-

Dr. Cora Breuner separates bike safety facts from fiction and shares tips from the dynamic perspective of a provider, educator and parent.
-

Begin a Lifetime of Sun Safety Early in Childhood
Protect your child from skin cancer by starting sun safety habits early. Learn about UV exposure risks and layers of sun protection from Dr. Robert Sidbury.
-

Wilderness Safety Tips for Families
Discover essential wilderness safety tips from Dr. Douglas Diekema, a pediatrician and outdoor enthusiast. Learn how to prepare for outdoor adventures.
-

Abdominal Pain in Kids: Anxiety-Related or Something More?
Seattle Children’s gastroenterologist explains stress-related abdominal pain symptoms in kids, offers coping techniques, and shares red flags for parents.
-

How to Address Sexual Abuse With Children and Teens
Learn how to educate children about sexual abuse, recognize signs, and empower them to speak up. Essential guidance from Seattle Children’s experts.
-

Cutting to Cope: What is Nonsuicidal Self-Injury?
Learn about the rise in teen self-injury, its causes, and how parents can help. Insights from Dr. Yolanda Evans, adolescent medicine specialist.
-

After Tragedy, Family Raises Awareness for Drowning Prevention
Preventable drowning incidents, like Yori's, highlight the importance of water safety. Learn how to keep children safe near water.
-

What Parents Need to Know About Vaping
These highly addictive products are becoming more popular and readily available. Know what e-cigarettes are and how to discuss vaping with their children.
-

Climate Change Effects on Skin: A Q&A With Dr. Markus Boos
Learn from Dr. Markus Boos, a pediatric dermatologist, how climate change affects children's skin conditions and how to protect them from UV radiation.
-

Helping Kids Cope With Anxiety Over Distressing News
Advice for families whose children might experience heightened anxiety after a frightening news event.
-

Helping Families Navigate the Digital World
Dr. Dimitri Christakis discusses the impact of digital devices on children's development and offers insights on healthy screen use.
-

Expert-Tested Tools to Manage Your Child’s Mental Health
Help manage your child's mental health crisis with the Escalation Cycle. Learn the six stages and interventions to support your child's emotional well-being.
-

Cultivating a Healthy Environment for Our Children
How to make a difference, on a small and large scale, to create a sustainable and healthy environment for all.
-

Pools at Home: Safety Tips for Caregivers
Stay safe with temporary above-ground pools this summer. Learn about the unique drowning risks and essential safety precautions to protect your family.
-

Making Sense of Restless Sleep Disorder in Children
Learn about Restless Sleep Disorder (RSD) in children: symptoms, diagnosis, and treatment. Expert insights from Seattle Children’s to transform your child's sleep quality.
-

Family Joins Experts to Shed Light on Acute Flaccid Myelitis
Maxford's journey with Acute Flaccid Myelitis sheds light on this rare neurological condition. Learn about his recovery and what researchers are discovering about AFM.
-

Kids and Suicidality: The Behavioral Health Crisis Care Clinic Steps Into the Gap
Seattle Children’s Behavioral Health Crisis Care Clinic provides evidence-based treatment and renews hope for kids and families through mental health crisis and suicidal thoughts.
-

Vitamin D Levels During Pregnancy Linked with Child IQ, Study Shows Disparities Among Black Women
Study published in The Journal of Nutrition links maternal vitamin D levels in pregnancy to children's IQ. Lower levels found in Black pregnant women.
-

Dr. Markus Boos Discusses Rashes: What’s Normal and When to Worry
Discover how Dr. Markus Boos at Seattle Children’s approaches rashes with detective-like precision, providing insights into common conditions like eczema, HFMD, and psoriasis.
-
Pediatric Infectious Disease Doctors Answer Parent’s Most Common Questions about Vaccines Under 5
Experts assure vaccine safety and effectiveness, emphasizing their importance in protecting young ones from viruses.
-

COVID-19 Vaccines Now Available for Kids Under 5
Seattle Children’s became one of the first locations in the country to offer COVID-19 vaccinations to children ages 6 months to 4 years old.
-

Responding to Our State's Youth Mental Health Emergency
Dr. Alysha Thompson discusses the impact the pandemic has had on youth mental health and shares advice for parents.
-

Dr. Gina Sequeira discusses what gender identity is, explains gender related terms, and offers recommendations to caregivers to help them support gender-diverse children.
-

Spring Safety-Gear Check-Up: Bike Helmets and Life Jackets
Spring is a great time to check your family’s bike helmets and life jackets, to be sure they’re in good shape and still fit properly.
-
Discover Olive Ray, the fifth grader with an indomitable spirit. Despite facing brain tumors, she spreads joy, navigates clinical trials, and embraces life with sass and sparkle.
-

Seattle Children’s Launches First U.S. CAR T-Cell Clinical Trial for Children with Lupus
Seattle Children’s launches the first chimeric antigen receptor (CAR) T-cell clinical trial in the U.S. for children under 18 with the most common form of lupus.
Disclaimer
The information on the blog is for informational purposes only, and should not replace the relationship that exists between you and your healthcare provider. Never disregard professional medical advice or delay seeking care because of something you read in On the Pulse.
Call your child’s pediatrician or family physician if you are concerned about the health of your child, or if you’re looking for specific medical advice and/or treatment recommendations. Call 911 in the case of any emergency.
The opinions expressed on this site are the personal opinions of the original author(s), not of Seattle Children’s. The content is not meant to be an endorsement or representation by Seattle Children’s or any other party.
All content is copyrighted. Please read Seattle Children’s Terms of Use.
