Seattle Children’s Brain Tumor Program
Contact the Brain Tumor Program
More experience treating children with brain tumors than any other hospital in the region
If your child or young adult has a brain tumor, our team has the medical and surgical expertise to help them not only survive but thrive. Seattle Children’s Brain Tumor Program cares for your child from diagnosis through all phases of treatment and follow-up survivor care, helping them grow up to be a healthy and productive adult.
Children treated at Seattle Children’s for brain tumors have survival rates that are consistently among the best in the country, and typically 10% higher than the national benchmark. U.S. News & World Report has recognized Seattle Children’s as one of the top 10 best children’s hospitals in the U.S. and the best in the Pacific Northwest. Both our Cancer and Blood Disorders Center and Neurosciences Center are ranked among the nation’s top pediatric centers for cancer, neurology and neurosurgery.

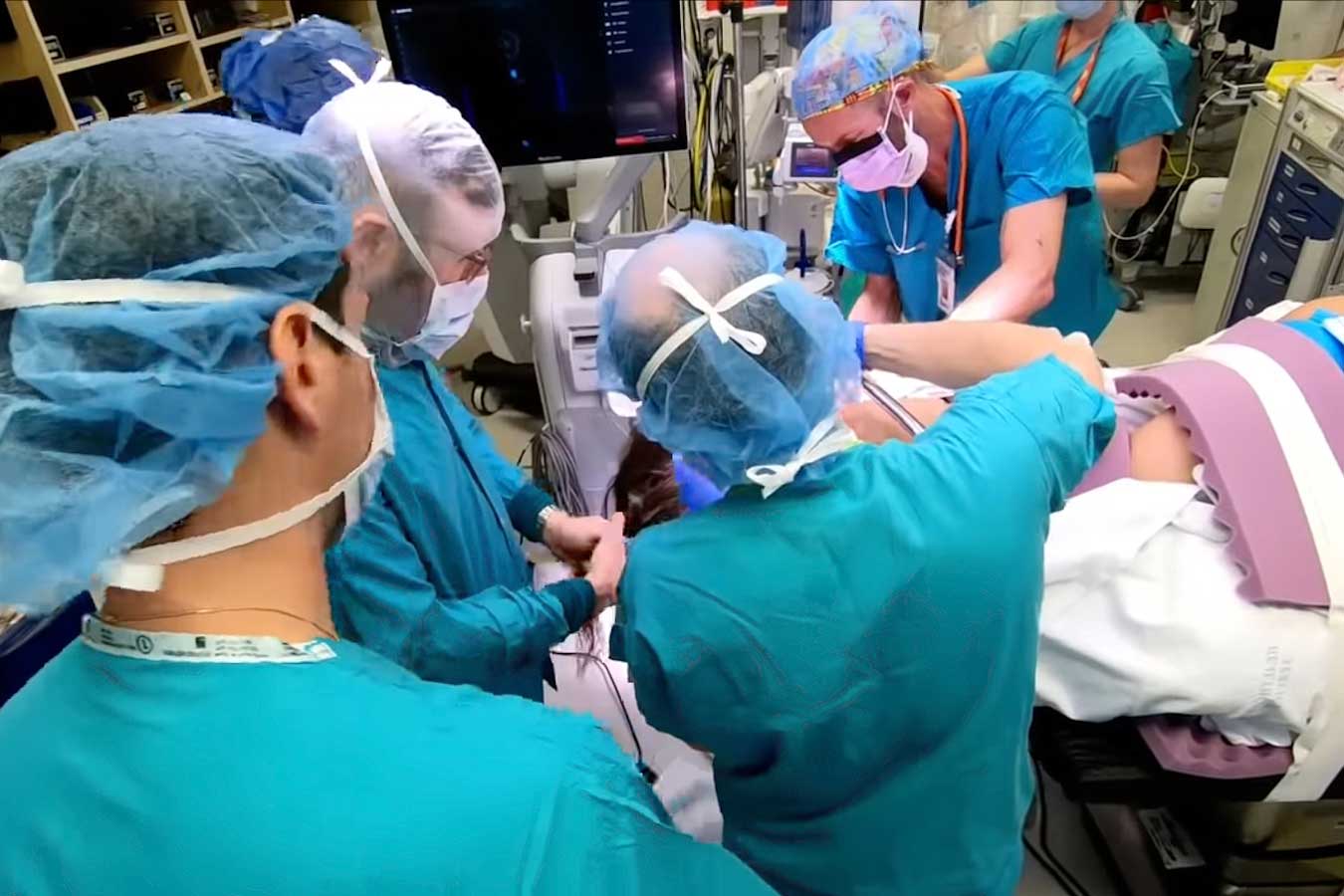
In July 2020, just after Aisley's third birthday, she began to experience concerning symptoms: headaches in the back of her head, lack of appetite, and vomiting.
Aisley had brain surgery to remove the tumor and the family received a devastating diagnosis – she had a very aggressive malignant embryonal brain tumor that could have been fatal.
Why choose our brain tumor program?
With the nation’s top leaders in pediatric brain tumor care and research, our Brain Tumor Program offers some of the most advanced treatments and clinical trials of any children’s hospital. If surgery is the best route to a cure, your child is in the hands of neurosurgeons skilled in innovative, . We perform significantly more neurosurgeries than any other children’s hospital in our region (Washington, Alaska, Montana and Idaho). More cases mean greater expertise and a sharper ability to determine if surgery is even needed — and that adds up to better outcomes.
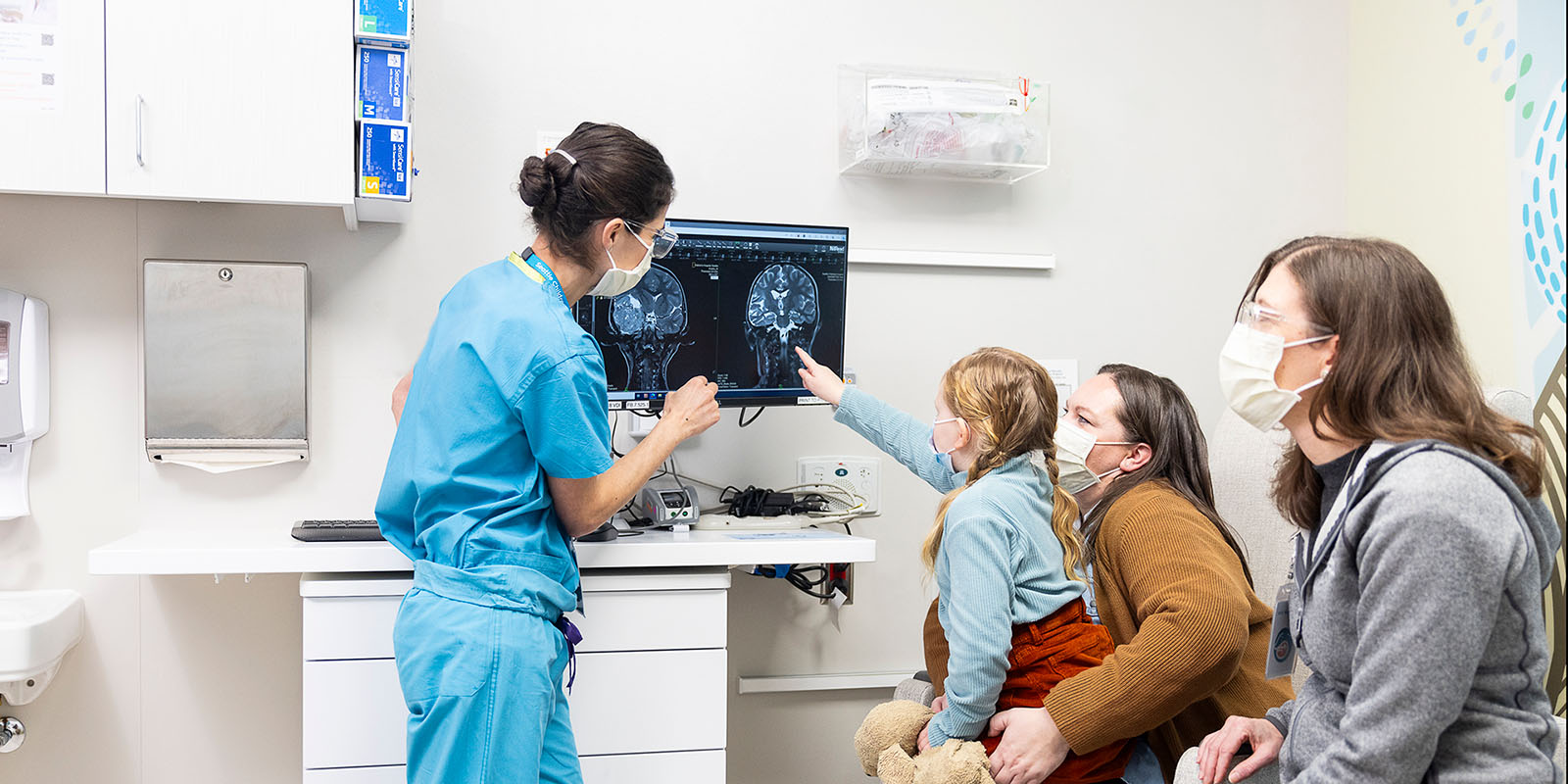
Precision medicine to personalize treatment
Seattle Children’s is at the forefront of precision diagnosis, using molecular profiling to identify a child’s tumor subtype and provide the best treatment. Few centers across the country can match our expertise.
Knowing a child’s brain tumor molecular subtype can open the door to treatment that increases survival, as shown in a clinical trial that charts a better course for kids with high-risk medulloblastoma.
State-of the art neuroimaging gives us detailed information about your child’s brain’s structure and how it works.

The state’s only comprehensive cancer center
Seattle Children’s partnership with Fred Hutchinson and the University of Washington is designated a comprehensive cancer center by the National Cancer Institute — the only one in Washington state. This partnership improves access to cutting-edge advances in basic science, new therapies and supportive care for your child.
Learn how we care for children and young adults with brain tumors.

Access to clinical trials offered only at top centers
Children we treat have access to new options in clinical trials that are often not available at other hospitals. These include CAR T-cell immunotherapy for especially hard-to-treat brain tumors like diffuse intrinsic pontine glioma (DIPG).
We offer research studies of novel therapies for children with all types of tumors. We are the only center on the West Coast that is a member of both the Pacific Pediatric Neuro-Oncology Consortium (PNOC) and the Collaborative Network for Neuro-oncology Clinical Trials (CONNECT).

Focused on long-term health
We take care of your whole child, looking ahead to a healthy future. If cancer or treatment may harm their fertility, we talk about options for fertility preservation.
After treatment ends, our Cancer Survivor Program will help keep your child healthy over the long term. We partner with the Survivorship Program at Fred Hutch to transition survivors to adult care when they are ready.
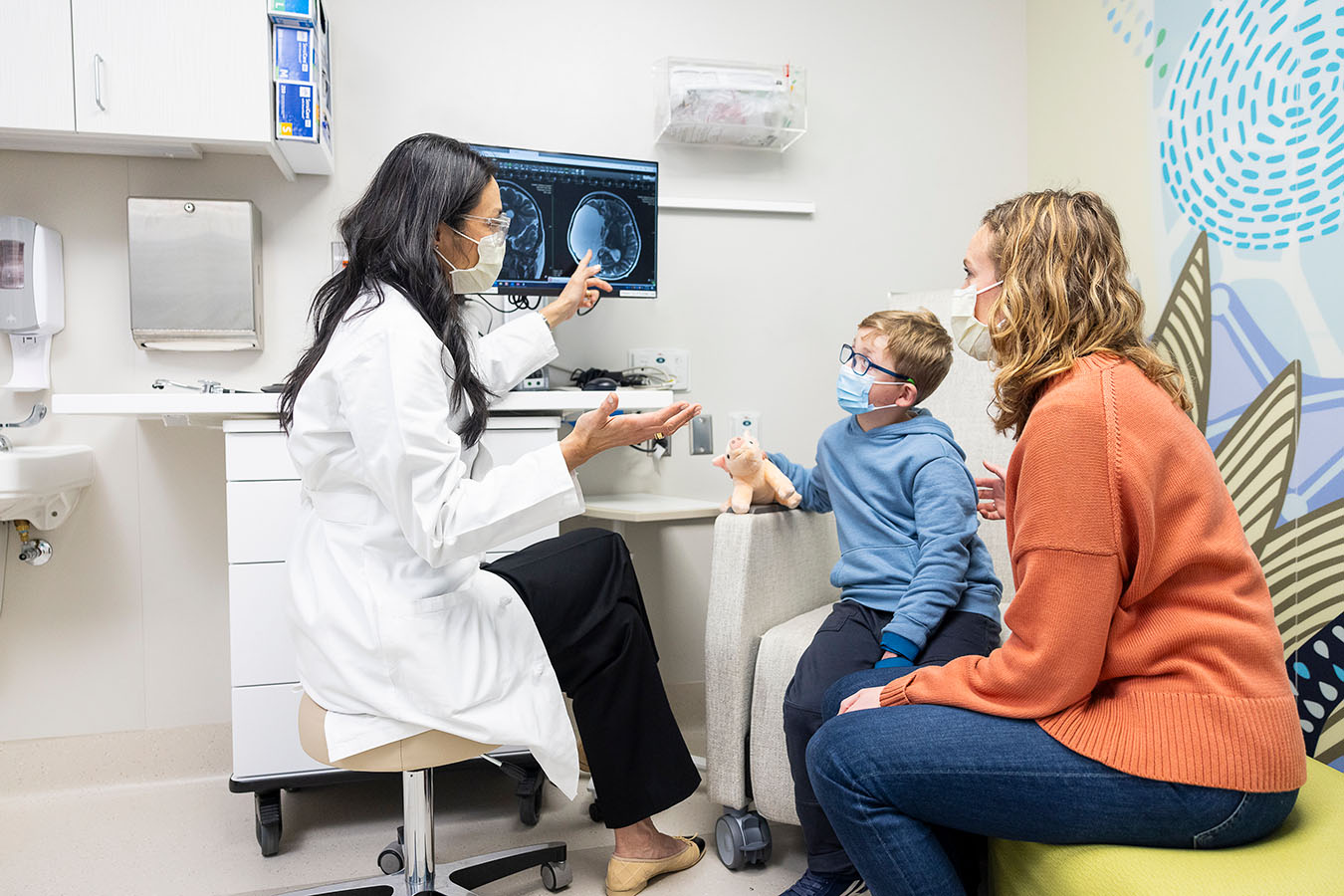
Meet Your Brain Tumor Team
Our Brain Tumor Program brings together a coordinated care team of experts, including pediatric neurosurgeons, neuro-oncologists and radiation oncologists. We see patients together in our weekly multidisciplinary Brain Tumor Clinic, and the whole team meets as a group each week at our Brain Tumor Board. Together, we review all the information on your child to develop their diagnosis and treatment plan. After the meeting we talk with you about the plan. Together, we build the best care plan for your child. Meet Your Team.
Conditions We Treat
Learn more about how we treat children and teens with all types of central nervous system tumors, including:
Low-grade glioma (glee-OH-muh) is the most common type of tumor in children. Low-grade means slow-growing.
Some types of LGGs are:
- Pilocytic astrocytoma (pie-LO-sit-ic ah-stro-sigh-TOE-muh)
- Pilomyxoid astrocytoma (pie-LO-mix-oid)
- Diffuse astrocytoma
It is very rare for a low-grade glioma to become life-threatening once it is properly diagnosed and treated. Treatment is aimed at preventing the tumor from affecting how your child’s brain works.
We may treat a low-grade glioma by surgery alone, depending on where it is in the brain.
Treatment options also include:
- Radiation therapy using very focused beams.
- Chemotherapy for children who need treatment other than surgery.
- Observation or “watchful waiting.” Some LGGs may not need any treatment. If that is the case for your child, the Brain Tumor team will keep a close watch.
HGGs can happen in any part of the brain or spinal cord. Most often we find them in the upper part or front of the brain (cerebrum). Diffuse midline glioma is 1 type of HGG.
Surgery, radiation therapy and newer medicines have improved survival for children with HGG.
Diffuse intrinsic pontine glioma (dih-FYOOS in-TRIN-sik PON-teen glee-OH-muh) starts in a central part of the brainstem called the pons.
The pons controls important functions like breathing and heart rate. DIPG can put pressure on the nerves that control movement of the face, eyes, speech and swallowing. Because of the location, it is currently not possible to remove all of these tumors by surgery. DIPGs are always considered high-grade.
At Seattle Children’s we can biopsy these tumors, then analyze them for genetic mutations. This helps us know if specific clinical trials or new treatments might help your child.
Treatment with radiation and chemotherapy often improves symptoms and prolongs life. Still, DIPG does eventually progress, and there are no standard therapies that cure it yet. This is why we offer research studies of novel treatments for children with DIPG or DMG with H3K27 alterations. We offer 1 of the only CAR T-cell immunotherapy trials for children and young adults with DIPG.
Some types of embryonal tumors (em-BRY-uh-nul) include:
- Medulloblastoma (meh-dull-oh-blas-TOE-muh)
- Pineoblastoma
- Embryonal tumor with multilayered rosettes (ETMR)
- Atypical teratoid/rhabdoid tumors (ATRT)
These high-grade tumors may grow quickly and always need treatment. In addition to surgery, we use a combination of radiation and chemotherapy for older children. We offer a “radiation-sparing” approach for young children. Research led by Seattle Children’s doctors has improved survival and changed treatment all over the world for children with embryonal tumors.
Ependymoma (eh-PEN-di-moh-ma) may happen in any area of the central nervous system.
Most children with these tumors are treated with surgery, often along with radiation therapy. Chemotherapy is effective for some children.
Tumors near or in the pituitary gland happen most often in teens or young adults. These tumors may cause hormonal changes or pressure on the nerves that control vision. Sometimes, pituitary tumors are noticed on an MRI (magnetic resonance imaging) for an unrelated reason such as headaches.
Pituitary tumors are almost never life threatening once properly diagnosed and treated. Your child’s doctor may recommend:
- Surgery.
- Medicine.
- Observation or “watchful waiting.” This means checking your child’s tumor regularly to see if it causes problems that need treatment.
Getting Care at Our Brain Tumor Program
Many children and families travel to Seattle Children's for brain tumor treatment and surgery. You can stay focused on your child while we help coordinate transportation and housing. We have lots of experience helping families make the transition back home safely.
Patient Success Stories
More than 80% of the children and teens we treat for brain tumors are cured.

“The surgery was risky and giving the green light was the most difficult decision I’ve ever made, but that day in January ended up being the happiest of my life. We never dared to think that the doctors could get 100% of Avery's tumor while protecting what made our daughter herself.”
- Kristie Berg, Avery's mom

“I was told it was about a two-year recovery process after surgery and that after two years, that was as good as I was going to get. But, every year, I somehow reach a new height.”
— Liesel, Seattle Children's patient and recent Harvard graduate
Seattle Children's Resources
Call the Brain Tumor Program at 206-987-2106 if you have questions or would like more information.
If you would like an appointment, ask your child’s primary care provider for a referral.
If you have a referral, contact the Brain Tumor Program at 206-987-2106 or by email.