
Heart Transplant Program
Contact the Heart Transplant Program
Delivering the Best Cardiac Care in the Pacific Northwest Before, During and After Heart Transplant
Seattle Children’s Heart Transplant Program treats infants, children, teens and young adults from birth through age 21 with heart failure. If your child needs a heart transplant, Seattle Children’s is the best place to be in the Pacific Northwest (PNW).
Since our program started in 1994, our team has done more than 300 pediatric heart transplants. We do the most heart transplants for kids of any hospital in the PNW, and our heart transplant survival rates are among the best in the nation. Optum’s Clinical Sciences Institute lists our program as a Center of Excellence.
Why Choose Seattle Children’s Heart Transplant Program
Seattle Children’s post-transplant 3-year survival rates, for both patients and grafts (donated hearts), exceed the national average.
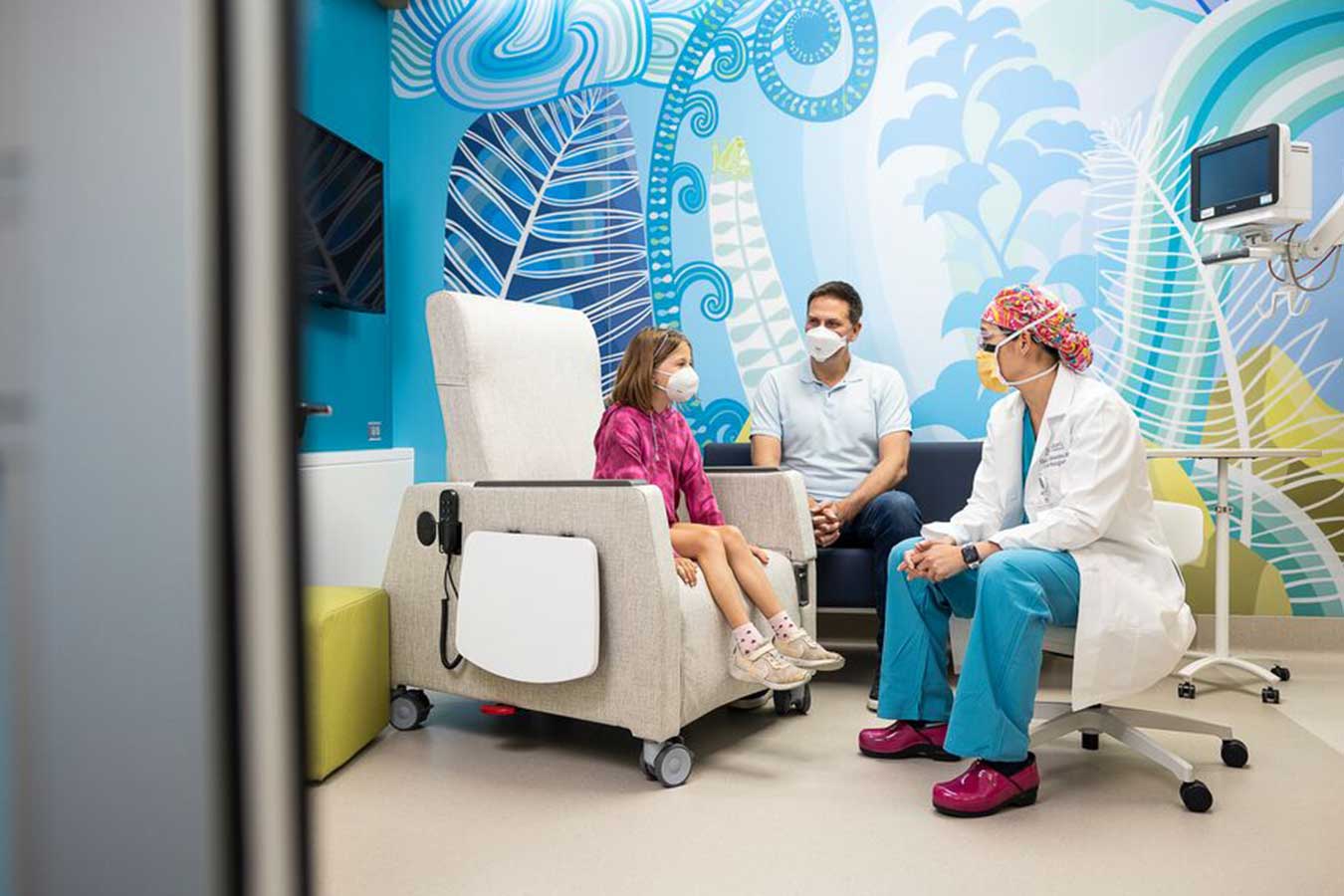
Setting Families Up for Success for 3 Decades
Transplantation requires a great deal of preparation and lifelong follow-up care. We are with you every step of the way — from evaluation, to getting on the heart transplant waiting list, through heart transplant recovery. Families come to us from Washington, Alaska, Montana, Idaho, Oregon, Hawaii and beyond for superior heart care.
Along with expert surgical techniques, we have state-of-the-art , blood banking and medical treatment. So, we can do successful heart transplants for children who otherwise would not qualify.
We do heart transplants for newborns through young adults. Our 3-year heart transplant success rate is 96%, almost 10 points higher than the national average.
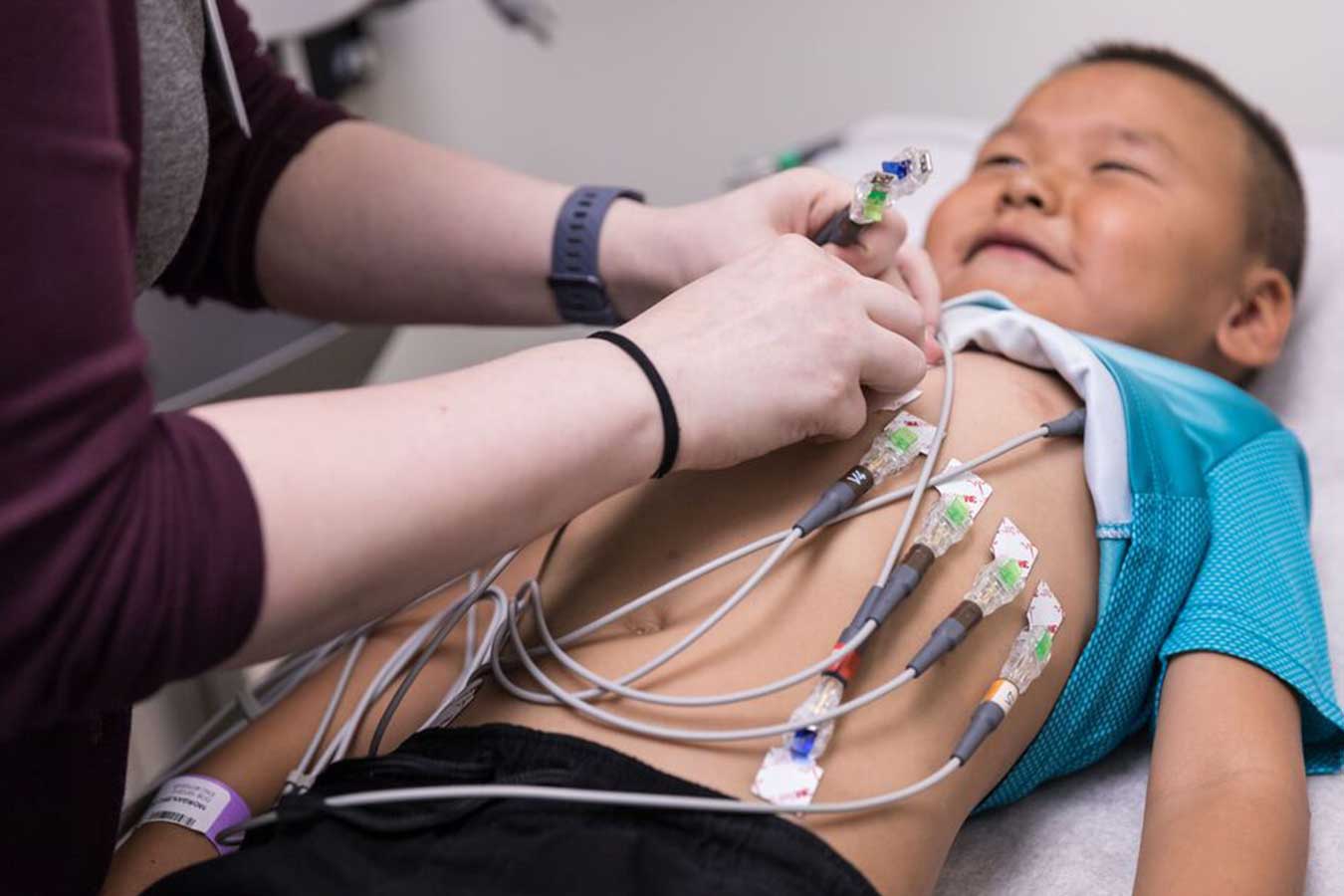
Advanced Therapies That May Help Avoid a Heart Transplant
Our Heart Failure Program is the only one in the PNW with the expertise to offer every type of therapy if your child’s heart cannot pump enough blood to meet the body’s needs. We have the medical and surgical expertise and the latest technology to handle the most complex cases. Often this means we can avoid or delay a heart transplant.
Doctors will first see if medicine, cardiac catheterization, heart surgery or a hybrid heart procedure can improve the heart enough. If these don’t work, your child’s doctors may recommend a transplant. This means replacing your child’s diseased heart with a healthy heart from a donor. A heart transplant in a child typically lasts well into adulthood.

Providing Lifesaving Support Until a Heart Transplant Can Happen
Our Extracorporeal Life Support (ECLS) Program supports children whose heart or lungs are not working properly. It’s the largest pediatric ECLS program in the PNW.
We provide all types of ECLS for children, including extracorporeal membrane oxygenation (ECMO) and ventricular assist devices (VADs), like a Berlin heart. ECMO is a form of heart-lung bypass used to pump oxygen-rich blood through your child’s body when their heart cannot. A VAD is a mechanical pump implanted inside or outside your child’s chest. Both ECMO and VADs may help keep children alive until they can get a heart transplant. Children who need the highest level of care stay in our Cardiac Intensive Care Unit.

Shortening Wait Times With ABO Blood Group–Mismatched Heart Transplants
We offer ABO blood group–mismatched transplants so children do not have to wait as long for a heart transplant.
If a child has type O blood, some centers will only transplant a donor heart that is also type O. These children typically wait the longest for a heart donation. We will accept O, AB, A or B for children who don’t yet have antibodies to blood types other than their own. Our outcomes for ABO-incompatible transplants are as excellent as for ABO-compatible transplants.
We work with our blood bank to carefully prepare our patients so they can have an ABO-incompatible transplant. Our methods can help keep patients from forming that may attack the new heart (called rejection).

Reducing the Risk of Organ Rejection for HLA-Sensitized Patients
Children who have had many surgeries may form antibodies to certain human leukocyte antigens (HLAs). HLAs help define if an organ is a good match for a patient. If a child already has antibodies (they are HLA sensitized), they usually wait longer than others for an acceptable organ, and they are at higher risk for rejecting their new heart.
At Seattle Children’s, we have done heart transplants for children who are HLA sensitized and may offer this in properly selected cases. We use advanced techniques to decide on the best donor match for each child. After the transplant, we use leading-edge to keep the child’s immune system from rejecting the new heart.
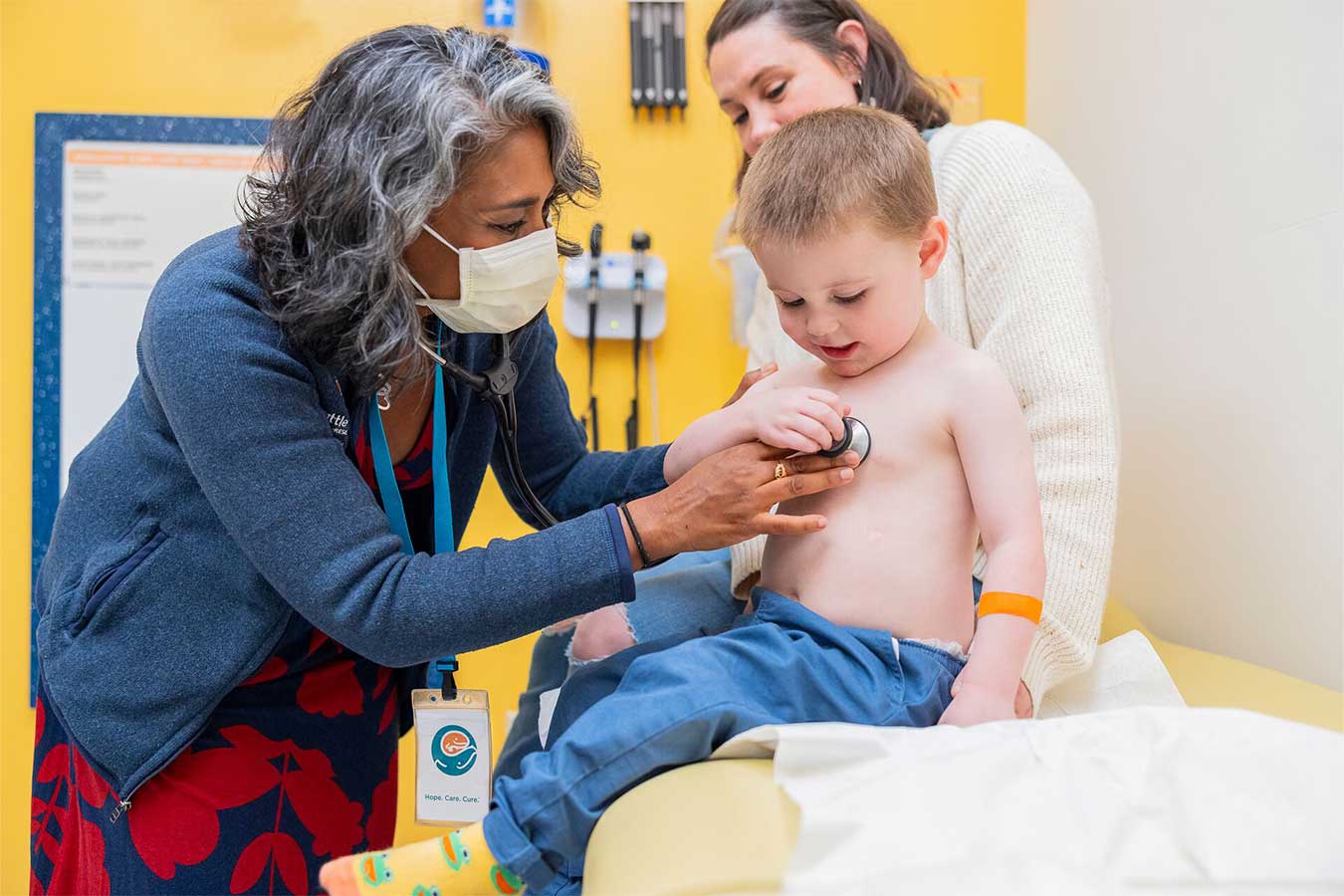
A Dedicated Heart Transplant Clinic to Meet Your Needs
We are committed to making sure your child has the best possible growth and quality of life. The Heart Transplant Clinic provides compassionate cardiac care and coordinates with other providers your child may need. Your child will visit this clinic for most appointments before and after their transplant.
We’re here to help you learn what to expect and how to prepare. Along with caring for your child’s health, we can help with questions about topics like insurance and the cost of a heart transplant.

Research to Make a Better Future Possible
Seattle Children’s heart doctors are leaders in international groups working to improve pediatric cardiac transplantation. We share our expertise and learn from the experience of transplant centers around the world. Together, we’re making a better future possible for young patients.
We also take part in multicenter research studies that give our patients access to new, better treatment options. For example, we continue to fine-tune treatment with medicines after transplant so a child does not reject their new heart and is less likely to have complications.
Learn more about heart transplant research at Seattle Children’s and how to participate in transplant research.
Meet Your Heart Transplant Team
Everyone on the heart transplant team is dedicated to helping your whole family return to an active, normal life.




Michael McMullan, MD
Division Head, Congenital Cardiac Surgery; Surgical Director, Cardiac Transplant; Director, Mechanical Cardiac Support and ECLS Services, Co-Director, Heart Center
View Profile



A Coordinated Effort
The same team of doctors, nurses and technicians will care for your child before, during and after transplant. Our highly skilled specialists are highly experienced in the surgical and medical care of pediatric heart transplant patients. They include pediatric:
- Heart surgeons
- Heart transplant
- Transplant nurses
They are further supported by:
- Infectious disease experts
- Blood bank doctors
- , , and feeding specialists
Meet the full Heart Center team.
Let’s Get You Where You Need to Be
Getting Care at Seattle Children's Heart Transplant Program
Patient Success Stories
Gabrielle's Story
For 8 years after having a heart transplant at Seattle Children’s as an infant, Gabrielle lived the life of a typical kid her age. Then, suddenly, unexplained fevers signaled a problem. Her transplanted heart had developed severe coronary artery disease. Now, after a second transplant, she’s thriving once again.
“If you do not know our family, you could not identify that she is a transplant kiddo. She loves school, Broadway shows, and has a whole gaggle of friends.”
~ Christen, whose daughter had 2 heart transplants at Seattle Children’s
Kaelyn's Story

After more than 500 days in Seattle Children’s Hospital attached to a Berlin Heart, Kaelyn finally received a donor organ and had a long-awaited heart transplant. Less than 2 weeks later, she was able to go home with her parents.
“She loves being outdoors. Just seeing her do the things she couldn’t do while she was in the hospital makes us extremely happy.”
~ Christine, who says her daughter got the best care possible at Seattle Children’s

