Spondylolysis and Spondylolisthesis
Contact the Spine Program
What are spondylolysis and spondylolisthesis?
Spondylolysis (spon-dee-low-LYE-sis) means spine defect. Children with this condition have a problem in the bones (vertebrae) of their lower back.
Doctors think the problem may be due to tiny cracks in the bones (stress fractures). Often, these cracks happen over time from using the spine.
Stress fractures in the spine are more common in children who play sports that make them arch their back a lot. Gymnasts, linemen in football, volleyball players and swimmers who do the butterfly stroke are most likely to have this problem.
Spondylolysis may lead to spondylolisthesis (spon-dee-low-lis-THEE-sis). In a normal spine, the bones are stacked on each other with disks in between. The disks absorb shock. When 1 of the bones slides forward, it is called spine slippage or spondylolisthesis. This can lead to problems with nearby nerves. This is rare in children.
Together, these conditions are the most common causes of ongoing (chronic) back pain in children. By the time they are 6 years old, about 6 in 100 children may have spondylolysis.
Spine Program at Seattle Children's
What are the symptoms of spondylolysis and spondylolisthesis?
In some children, spondylolysis and spondylolisthesis may not cause any clear symptoms. In others, spondylolysis can cause pain that spreads across the lower back. Pain may be worse when your child arches their back.
If your child has severe slippage, it can stretch the nerves in the lower back. This can lead to:
- Pain that goes down 1 or both legs
- A numb feeling in 1 or both feet
- Weakness in your child’s legs
- Trouble controlling bladder or bowel movements
How are spondylolysis and spondylolisthesis diagnosed?
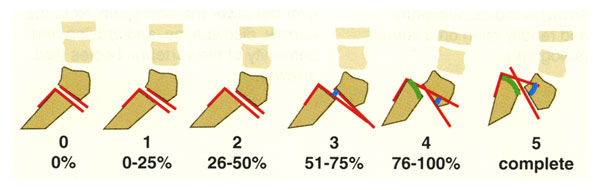
Examples of a bone in the spine sliding forward off the disk — from 0 (no slippage) to 5 (full slippage, or complete displacement).
Doctors look first for signs of cracks in the bones of your child’s back. We start by checking for these cracks because spine slippage usually happens to those who have the fractures first.
The doctor will ask your child if the pain is worse when they arch their back. This is a common sign of stress fractures. Most often, these fractures are in the lower part of the spine.
Imaging tests your child may need
Next, we most likely will take of your child’s spine. This helps doctors confirm if your child has a stress fracture. If we cannot see any cracks clearly on the X-ray, we may ask to do a .
If we find a crack in the bone, we will probably take a 3D image called a scan. It will give us an even better look at the fracture. This can help you and your child’s doctor decide on treatment.
How are spondylolysis and spondylolisthesis treated?
We use both surgical and nonsurgical treatment for spondylolysis and spondylolisthesis, based on how severe it is. Most children do not need surgery.
Physical therapy
At Seattle Children’s, we offer exercise programs to strengthen muscles in your child’s back and belly (abdomen). This helps support their spine and can help prevent more back pain. If an activity seems to be causing the problem, we may also ask your child to stop doing the activity for a while.
These steps may be all your child needs to relieve symptoms and heal stress fractures.
Bracing
For some children, back braces can take the pressure off the lower back and relieve pain. This can help them return to sports and school.
Braces flatten the normal curve of the lower spine. Your child will wear the brace as they move around during the day. Often, children can take the brace off at night to sleep. Sometimes, we ask children to wear the brace at night too. Usually, children wear a brace for 2 to 3 months.
As the pain lessens, your child can slowly decrease the amount of time they wear the brace. Read about braces and our other orthotics and prosthetics services.
Surgery
If your child’s pain lasts after physical therapy, rest and bracing, they might need surgery. We use surgery to fix the fracture or stop the slipping.
At Seattle Children’s, we offer 2 operations to treat these conditions:
- In 1 operation, the doctor repairs cracked bones by placing a metal implant across the fracture. They use a to help healing.
- In the other operation, for slippage, doctors join 2 or more bones (spinal fusion) to make your child’s back more stable. They may also be able to reduce some of the slippage. To do this, doctors place screws into the bones of your child’s lower spine and connect them with a rod. This holds the spine still. Next, they place a bone graft in the area to help the bones grow together.
We will talk with you and your child about each option to decide which is likely to work best.
Why choose Seattle Children’s for treatment of spondylolysis and spondylolisthesis?
The Spine Program at Seattle Children’s brings together a team of specialists to treat spondylolysis and spondylolisthesis in children, teens and young adults. . Ours is the largest pediatric spine center in the Pacific Northwest. We offer the most comprehensive care for your child, no matter how complex their condition is. It’s why other hospitals in the region refer their most complex pediatric patients to us.
-
The experts you need are here
- The Spine Program team includes doctors, surgeons, and from Orthopedics and Sports Medicine.
- We can successfully treat these conditions in most children with methods other than surgery. Nonsurgical treatment often means physical therapy or a back brace. We have the largest team of physical therapists in the Pacific Northwest who specialize in the care of babies, children, teens and young adults. We also have onsite orthotists to build and fit braces for our young patients.
- If your child needs surgery, our orthopedic spine surgeons are leaders in their field. They have more training and experience with children’s complex spine conditions than anyone else in the area. Spine surgery for children is all they do. Each is .
- Spine conditions can affect more than a child’s bones, muscles and joints. That’s why we connect you and your family with any expert your child may need across Seattle Children’s. For example, we may involve Adolescent Medicine, Neurosurgery, Rehabilitation Medicine, Rheumatology and Pain Medicine.
-
Our approach to surgery increases comfort and reduces stress
- We believe that most back problems in children do not need surgery.
- Before we recommend surgery, we look at your child as a whole person. Your child’s team will take many factors into account. These include the degree of their spinal problems, the effects on their health and how much more they will grow. We also consider what results you can expect from treatment.
- Our new state-of-the-art operating rooms reduce stress and increase comfort for your child. The design lets you stay by your child’s side until they gently go to sleep before any spine surgery.
- Neuromonitoring helps us prevent a spinal cord injury during surgery. Our surgical spinal cord monitoring team leads the country in new ways to make back surgery safer.
- We have the technology and skills to use 3D imaging to guide your child’s surgery, if needed. This helps us place hardware, such as rods and screws, with precision. It also lets us see in real time the changes we make to your child’s spine. Based on your child’s needs, we may use or .
-
Care from birth through young adulthood
- We specialize in caring for kids. This means our experts have the knowledge, training and skills to treat the youngest patients, from babies through young adults. We take care to find out what is causing your child’s symptoms.
- Children and teens are still developing. When we evaluate your child’s spine, plan their treatment and provide their care, we carefully consider their growth. We think about how growth may affect your child’s spine over time. We also consider how their spine may affect the rest of their development and health.
- If your child needs imaging that uses radiation, we use the lowest amount possible (PDF) to make the best image. We have a low-dose radiation X-ray machine, called the EOS. It makes safer full-body images. We also have the largest group of board-certified pediatric radiologists in the Northwest.
-
Support for your whole family
- We know it can be stressful to have a child with a spinal condition and to find the treatment they need. Everyone at Seattle Children’s works to make your experience here as easy as we can on your whole family.
- Your child’s team does more than plan and provide care for your child. We also make sure you and your child understand your child’s condition and treatment options.
- Care is easier for you because your child’s team members from the Spine Program work closely with each other — and with other programs and clinics your child may need at Seattle Children’s.
- Seattle Children's supports your family with a range of resources. Our Child Life specialists, the Family Resource Center and Guest Services are here to help.
-
Research to improve care
- Members of the Spine Program team are leaders in research. We are always tracking the results of our patients’ care so we can be sure we are choosing the best treatment for each child. Your child’s care team may ask if you want to be involved in research. For example, we may ask to include data about your child’s condition and treatment in our studies.
- Our spine experts are part of national and international research groups. These groups study the latest treatment approaches and technologies. Together, we work to find the best and safest ways to care for children. We are part of the Pediatric Spine Study Group, Harms Study Group and Fox Congenital Spine Study Group.
- Learn more about current orthopedics research at Seattle Children’s.
Contact Us
Contact Orthopedics and Sports Medicine at 206-987-2109 for an appointment, a second opinion or more information.
Providers, see how to refer a patient.
Paying for Care
Learn about paying for care at Seattle Children’s, including insurance coverage, billing and financial assistance.

