Hemangiomas
Contact the Vascular Anomalies Program
What is a hemangioma?
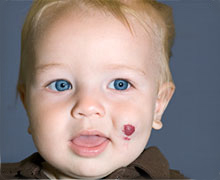
A hemangioma (hee-man-gee-OH-ma) is a tumor formed by extra blood vessels in or under the skin. Most hemangiomas are on the head and neck, but they can appear anywhere on the body. They are 1 of the most common skin problems in babies. Doctors do not know what causes them.
Most hemangiomas do not need treatment. But sometimes they cause problems with a child’s breathing, speaking, eating, vision or appearance.
Types of hemangiomas
The different types of hemangiomas need different treatment. Most often, when people talk about a hemangioma, they mean an infantile hemangioma.
- An infantile hemangioma (IH) appears within 2 months of birth. It keeps growing for the first couple of months after it appears, but rarely for more than 8 months. Then it begins a slow fading process called involution. This can last from 3 to 12 years. About 50% fade away by age 5. About 70% fade fully by age 7. Most hemangiomas are infantile hemangiomas.
- A congenital hemangioma is present at birth and grows as a child grows. This type is much less common than IH. A congenital hemangioma can shrink on its own (rapidly involuting or RICH) or be nonshrinking (noninvoluting or NICH).
If your child has more than 1 hemangioma on their skin, they have an increased chance of hemangiomas that affect organs inside the body. A large hemangioma can be a sign of rare conditions called PHACE syndrome and LUMBAR syndrome.
Vascular Anomalies Care at Seattle Children's
Experts from more than a dozen specialties work together in our Vascular Anomalies Program to make a care plan for your child.
Symptoms of a Hemangioma
Most hemangiomas in the skin look like discolored lumps, stains or raised areas. When a growth is below the skin's surface, it looks like a spongy mass filled with blood. Hemangiomas are most often on the head and neck, but they can appear anywhere on the body.
A hemangioma is rarely painful unless a sore develops on it. If the skin over the top of the hemangioma is hurt, it may bleed. If pressing on it does not stop bleeding within 10 minutes, call your child’s provider right away or take your child to the emergency room.
Diagnosing a Hemangioma
During your first visit to Seattle Children’s, the doctor will examine your child and ask about their symptoms and health history.
Sometimes we need to take pictures inside your child’s body. Imaging studies may include:
- Ultrasound
- MRI (magnetic resonance imaging)
- CT (computed tomography) scan
Sometimes, the doctor will cut a small piece of tissue from your child’s skin (biopsy) and examine it.
If your child has multiple hemangiomas (hemangiomatosis) on their skin, the provider may use ultrasound to check for hemangiomas inside the body (like on the liver) or for other medical problems (such as hypothyroidism).
Depending on the location and size of the hemangioma, we may assess your child for PHACE syndrome or LUMBAR syndrome.
Treating a Hemangioma
Your child’s care will depend on the type of hemangioma they have. Our team works with you to create the best treatment plan, based on your child’s medical needs and your family’s wishes.
Small hemangiomas often do not need treatment. Most go away on their own. Your child may need treatment if their hemangioma is:
- Large
- Causes problems with breathing, eating, vision or appearance
- Bleeds or has sores
While most hemangiomas fade over time, they can leave behind changes in skin color or texture, a fatty mass, a scar or extra skin. Early treatment can sometimes reduce the need for later treatment.
-
Regular check-ups
We will monitor your child’s hemangioma over time. We watch to see how it changes and whether it causes symptoms or bothers your child. If your child needs treatment, we partner with you to decide the best options.
-
Propranolol and other medicines
We may suggest medicine for your child, based on:
- The size and location of their lesion
- Whether the hemangioma bleeds or has sores
We will advise you on the best medicine for your child’s hemangioma.
For most children who need treatment for an infantile hemangioma (IH), we use propranolol first. This blood pressure medicine shrinks IHs in about 60% of patients. Propranolol does not affect congenital hemangiomas.
We use other medicines, such as:
- A beta blocker applied to the skin (topical timolol)
- Steroids
Seattle Children’s doctors were among the first in the region to use propranolol to treat IHs. We continue to study how well this medicine shrinks these tumors and improve how we use it. Propranolol can reduce the need for surgery and make needed surgeries less extensive because the tumor is smaller.
For a congenital hemangioma, we treat any sores that develop with antibiotic cream.
-
Laser treatment
Laser therapy uses light energy to quickly destroy the extra blood vessels. The type of light beam we use depends on the hemangioma. Pulsed dye laser treatment works well on bright red or dark (superficial) hemangiomas and hemangiomas with sores. Some children need multiple laser treatments over a period of time.
Most patients say the laser feels like a brief sting (like an elastic band snapping against the skin). To treat smaller growths in the clinic, we use a numbing cream on the skin, so the laser hurts less. We often treat children with larger lesions in the operating room under general anesthesia. We will talk with you to decide the best choice for your child.
We offer outpatient laser surgery (done while your child is awake) at our Seattle hospital campus, Bellevue Clinic and Surgery Center and North Clinic in Everett. We do laser treatments that need general anesthesia at our Bellevue center or Seattle hospital campus.
-
Surgery
Surgery to remove or reduce the size of a hemangioma may be the best option if:
- It causes serious problems, such as making it hard to see or breathe
- Treatment with medicine is not working
- The growth causes pain or bleeding
- It increases the risk of complications like blood clots
- Your child or family wants to remove the growth because of its appearance
Surgery may not be an option for some growths because of their size or location.
We use facial nerve mapping to make surgery safer when removing hemangiomas in the face. Before surgery, we use small electric pulses to map the exact location of the branches of the facial nerves. During the procedure, real-time feedback about nerve activity helps guide surgeons. The technique means shorter surgery time, with smaller cuts and near-zero risk of nerve injury.
Hemangiomas at Seattle Children’s
Our Vascular Anomalies Program is nationally known for treating children with hemangiomas and other vascular disorders. We are one of the largest and most experienced programs in the United States.
Families travel to Seattle Children’s for their child’s care because of our specialized expertise. We see nearly 2,000 children with vascular anomalies each year, more than any other hospital in the region.
For more information, contact the Vascular Anomalies Program by email or by calling 206-987-4606.
If you would like an appointment, ask your child’s primary care provider to refer you.
Providers, see how to refer a patient.
 “The care at Seattle Children’s was wonderful. We just felt a sense of relief, and we felt more knowledgeable after talking with the staff.” Emma’s mom, Donna West
“The care at Seattle Children’s was wonderful. We just felt a sense of relief, and we felt more knowledgeable after talking with the staff.” Emma’s mom, Donna West
-
The experts you need
- We have treated thousands of children for hemangiomas. Doctors with less experience might confuse a hemangioma for a different type of vascular anomaly, leading to the wrong treatment.
- We have the skill and experience to correctly diagnose your child’s tumor. If tests are needed to confirm it, we have a broad range of imaging studies.
- Our Vascular Anomalies team brings together experts from many fields of medicine. These include otolaryngologists, dermatologists, plastic surgeons, general surgeons, interventional radiologists, ophthalmologists and cardiologists.
- Our team helps set national standards for care of young people with vascular anomalies. We provide the most advanced treatments in our region.
-
The most advanced treatments and research
- Led by Dr. Jonathan Perkins, our physician-scientists identified a biomarker that can confirm the diagnosis of an infantile hemangioma and tell whether it is growing or shrinking. The team is working on ways to predict which children will benefit from propranolol, the current standard of care.
- Our doctors were among the first in the region to use the blood pressure medicine propranolol to treat infantile Propranolol is so effective that fewer children need surgery to remove the growths. We continue to improve propranolol treatment and ways to track if it shrinks a tumor.
- We perform more than 60 surgeries each year to remove hemangiomas. For children with tumors in the face, we use facial nerve mapping to greatly reduce the risk of nerve injury and scarring.
- Our physician-scientists do research to find better treatments and improve quality of life for children with hemangiomas. Learn more about vasular anomalies research at Seattle Children’s.
-
Team approach for complete care
- We schedule visits so your child sees all the specialists they need in as few days as possible. In some cases, we can consult via video phone calls with doctors or patients.
- Your child’s team will work together — and with you — to make a treatment plan that fits your child’s unique needs. Combining our skills helps make sure your child gets the very best care.
- As long as needed, our team keeps a watch on your child’s condition. We are always here to answer your questions and connect you to community resources.
-
We treat your whole child
- Our specialty is treating children’s disease while helping them grow up to be healthy and productive.
- Children do not react to illness, injury, pain and medicine in the same way as adults. They need – and deserve – care designed just for them. Our experts focus on how treatments today affect growing bodies in the future. We plan your child’s treatment based on years of experience plus the newest research on what works best – and most safely – for children.
- At Seattle Children's, we work with many children and families from around the Northwest and beyond. Whether you live nearby or far away, we can help with financial counseling, schooling, housing, transportation, interpreter services and spiritual care. Read about our services for patients and families.
Contact Us
If you have questions about a consultation or second opinion, email us or call 206-987-4606.
If you would like an appointment, ask your child’s primary care provider to refer you.
Providers, see how to refer a patient.
Paying for Care
Learn about paying for care at Seattle Children’s, including insurance coverage, billing and financial assistance.
