Sleep Medicine
Contact the Sleep Medicine Program
Sleep medicine is the diagnosis and treatment of sleep-related conditions and sleep disorders, including problems problems breathing while sleeping (sleep apnea), falling asleep or staying asleep. Sleep problems can affect your child's ability to get the sleep needed for good growth, development and overall health. Sometimes, problems with sleeping contribute to learning, mood and behavior troubles during the day.
Why choose Seattle Children’s Sleep Medicine program?
Sleep conditions and disorders can vary significantly from patient to patient. Our multidisciplinary team and subspecialized care providers work together to ensure each patient and family receive the ideal care based on their own unique needs.
As the only exclusively pediatric-focused sleep center in the region, we provide comprehensive, compassionate and patient-centered care tailored to this unique population.
-
State-of-the-Art Pediatric Sleep Center
Seattle Children’s state-of-the-art Sleep Center, located in Bellevue in the Overlake Medical Pavilion, is the largest and premier pediatric sleep center in the region. The center is equipped with the latest sleep medicine technology and designed with a child in mind; our waiting rooms, overnight sleep suites, decor, artwork and furniture are all kid and family-friendly and provide a comfortable and calming environment.
Sleep Center features include:
- Six outpatient clinic exam rooms.
- Twelve spacious private overnight sleep study suites with sleeping accommodations for your child and one parent/caregiver. Each room features a large private bathroom with a toilet and sink, television, white noise machine and digital entertainment options for the family.
- Accommodations for children with medical complexity are readily available on site.
- Private showers and kitchen located in the family lounge area.
- Access to child life specialists at Seattle Children’s, a unique pediatric role focused on making your family’s experience at the sleep center a positive one.
- “Desensitization kits” are available to take home before a sleep study if your child has sensory processing issues or may be uncomfortable or afraid of wires or medical equipment. Kits include stickers and wires so your child can practice putting them on their body to get ready for their sleep study; it lets them feel these things in advance at home, in their own way, on their own time. We can also show your child pictures of what they will look like when they are hooked up to the sleep study equipment to help them feel more comfortable.
- Family-centered, coordinated care from our team of pediatric specialists. If your child is medically complex and receives care from multiple specialists either within or outside of Seattle Children’s, the sleep medicine team works with you and your child’s other providers to make sure your child’s care is coordinated.
- We are the largest pediatric-exclusive sleep medicine program and sleep center in the region. Our team of almost 50 includes eight sleep medicine doctors (including three neurologists trained in sleep medicine), four advanced practice providers (APPs), three registered nurses, two CPAP/BiPAP coordinators and 30 polysomnographic technologists. Our accrediting body, the American Academy of Sleep Medicine, only requires that we have one Registered Polysomnographic Technologist (RPsgT) on staff, but all 30 of our technologists are RPsgT credentialed. Learn more about our sleep medicine team.
Take a Look Inside our Sleep Center

Sleep Center lobby and check-in area.
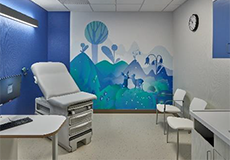
Outpatient clinic exam room.

Sleep study suite with pull-out sleeper bed for parent.

Each sleep study suite has a private spacious bathroom with a toilet, sink and changing area.

Showers are available in the family lounge area.

A kitchen is available in the family lounge area.
-
Your child and family get support
At Seattle Children’s, your family has a full team behind you, from diagnosis through treatment and follow-up. From our appointment schedulers to our pediatric nurses, our team is specially trained to work with children and their families. Our facilities and equipment also reflect this kid-friendly, family-centered approach.
At our Sleep Center located at Seattle Children's at Overlake in Bellevue, we have designed our sleep lab so you or another adult family member has a place to stay with your child during the overnight sleep test.
-
The compassionate experts you need are here
Our team of experts focuses on how today’s treatments will affect your child as they develop and become adults. We base treatment plans on years of experience and the newest research on what works best — and most safely — for children, teens and young adults. This experience helps us monitor your child’s condition and work with you to decide on the best treatment.
Seattle Children’s offers the only sleep center in the region exclusively dedicated to caring for babies, children and teens. Our sleep program is accredited by the American Academy of Sleep Medicine.
-
We’re advancing research for children and teens
Our team is involved in research that is transforming the diagnosis, treatment and care of conditions affecting children, teens and young adults.
Conditions We Treat
We see children with a broad range of sleep disorders, including:
-
Sleep apnea
Sleep apnea refers to short pauses in breathing. Usually, these pauses are normal, but they can cause problems when they occur often.
- Obstructive sleep apnea occurs when your child's airway closes partway or all the way during sleep. This blocks air from getting in. The brain recognizes a breathing problem, and this can disrupt sleep. In children without other medical conditions, enlarged tonsils or adenoids may cause the blockage. The problem is most likely to happen during sleep when the throat muscles and tongue are most relaxed. Read more in Obstructive Sleep Apnea in Children. (PDF) (Dari) (Spanish) (Vietnamese).
- In children with central sleep apnea, the part of the brain that controls breathing doesn't start or maintain the breathing process as it should. This condition can affect babies, especially those who are born early (premature), because the breathing control center in the brain is not fully developed.
-
Parasomnias (sleep terrors and sleepwalking)
Parasomnias are disruptions in your child's sleep. These include sleep terrors and sleepwalking.
- Sleep terrors (night terrors) may seem like nightmares, but they are far more intense. During a night terror, you may not be able to comfort your child. Signs of a night terror are sitting up in bed, shouting or screaming. Learn more in Sleep Terrors. (PDF) (Spanish). While scary for parents, sleep terrors usually do not harm children.
- During sleepwalking, your child may seem confused or partly awake. They may either stay in bed or walk around without seeming to be aware of their surroundings. Learn more in Sleepwalking. (PDF) (Spanish).
Children will often not remember either sleep terrors or sleepwalking the next day. In some cases, these conditions may be a sign that your child has another sleep disorder. Learn more in Parasomnias. (PDF) (Spanish).
-
Excessive sleepiness
Young people with excessive sleepiness are often very sleepy during the daytime or sleep for very long periods at night. These disorders, sometimes called hypersomnia, are different than sometimes feeling tired after not getting enough sleep at night. Signs of this condition often appear during the teen years or early adulthood. Your child may nap a lot during the day, fall asleep at odd times or find it very hard to wake up after a long sleep. Excessive sleepiness may be caused by other sleep disorders, such as Narcolepsy. (PDF) (Spanish) or sleep apnea.
-
Insomnias
Insomnias are disorders that make it very hard to fall asleep or stay asleep. Most people have trouble sleeping once in a while. Babies and young children often wake up naturally during the night. When children have trouble falling asleep or staying asleep and the problem lasts a long time, it can be caused by an underlying sleep disorder. Learn more in Insomnia. (PDF) (Spanish).
-
Narcolepsy
Narcolepsy causes sleepiness that can't be controlled. People with narcolepsy, including children and teens, have "sleep attacks." Even if they have had a normal night's sleep, they may fall asleep without any warning during the day. These sleep attacks last from several seconds to a half-hour or more. Signs of narcolepsy often appear during the teen years. Learn more in Narcolepsy. (PDF) (Spanish).
-
Sleep phase (circadian rhythm) disorders
Circadian rhythm disorders are disruptions in your child's regular daily cycles, including sleeping and waking. Most circadian rhythms are controlled by the "clock" in the brain that runs the body. Circadian rhythm disorders may be caused by a mismatch between the internal body clock's setting and conditions in the outside world - a common example is jet leg. They may also be a sign of a problem within the clock itself.
-
Sleep-related movement disorders
Sleep-related movement disorders involve simple movements that can disrupt sleep. Some examples include:
- Growing pains (benign nocturnal limb pain of children)
- Headbanging and bodyrocking are rhythmic movement disorders that usually involve some type of rocking, rolling or headbanging. Learn more in Head Banging and Body Rocking. (PDF) (Spanish).
- Periodic limb movement disorder (PLMD) is a sleep disorder that consists of repetitive leg movements that occur during sleep that interfere with sleep and cause daytime symptoms. Periodic limb movements in sleep (PLMS) are brief jerks of the foot or leg that typically happen every 20 to 40 seconds. Children with PLMS can have restless leg syndrome. Children with PLMS and daytime symptoms of fatigue, sleepiness or behavioral problems may have PLMD, which is diagnosed with a sleep study. Learn more in Periodic Limb Movement Disorder. (PDF) (Spanish).
- Children with restless legs syndrome (RLS) may feel the need to move their legs but may also have uncomfortable sensations in their legs that are often difficult to explain. The uncomfortable sensation or urge to move the legs is worse in the evening and during periods of rest or while lying down. Walking or moving the legs may relieve the symptoms. RLS is diagnosed by your doctor. Learn more in Restless Legs Syndrome. (PDF) (Spanish).
- Restless sleep disorder is characterized by frequent movements and repositioning during sleep that interferes with good sleep quality and causes daytime symptoms. RSD is diagnosed with a sleep study.
While the causes of these disorders are different, they all make it hard for your child to sleep.
Services We Provide
We offer testing (sleep studies), treatment and consultation for sleep disorders that affect babies, children and young people less than 18 years of age (ages 0 to 17). These services include:
-
Polysomnography (sleep study)
Doctors use polysomnography (sleep study) to identify sleep problems. During sleep, the body acts differently than while awake. A sleep study monitors your child's body functions during sleep, including sleep stages, eye movements, brain waves, muscle activity, breathing, body positions and heartbeat. Learn more about Sleep Studies. (PDF) (Simplified Chinese) (Somali) (Spanish).
-
Sleep study with CPAP, Bi-PAP or oxygen
Children usually have sleep studies with continuous positive airway pressure (CPAP) or bilevel positive airway pressure (Bi-PAP) after they have been diagnosed with obstructive sleep apnea or another breathing disorder during sleep. We offer overnight sleep studies at our Sleep Center at Seattle Children’s at Overlake in Bellevue location only.
During these tests, your child sleeps wearing a facemask hooked to a special CPAP or Bi-PAP machine that records the right amount of air pressure for your child. The results give us the correct air pressure setting for you to set up a CPAP or Bi-PAP machine in your home. A sleep study may also be done with extra oxygen to help your child's breathing.
-
Multiple sleep latency test
A multiple sleep latency test (MSLT) is a daytime nap study that gathers information about your child's body functions and sleepiness during the day. The test is usually done right after a polysomnography (PSG or sleep study). During the MSLT, your child will take a series of naps every 2 hours throughout the day. We offer the MSLT at our Sleep Center at Seattle Children’s at Overlake in Bellevue location only.
Scheduling an Appointment with Sleep Medicine
- If you would like a referral to Sleep Medicine, talk to your primary care provider. If you already have a referral, please call 206-987-5072 to schedule an appointment.
- If you already have an appointment, learn more about what to expect and how to prepare.
- Learn about Sleep Medicine resources such as useful links, videos and recommended reading for you and your family.
Telemedicine at Seattle Children’s
Your child’s first appointment in our clinic will be in person and take about 90 minutes. Later visits may be offered via telehealth (virtual). Learn more about telemedicine at Seattle Children’s.
Contact Us
For more information, contact Sleep Medicine at 206-987-5072. If you would like an appointment, ask your child’s primary care provider for a referral.
Providers, see how to refer a patient.
Paying for Care
Learn about paying for care at Seattle Children’s, including insurance coverage, billing and financial assistance.
Access Additional Resources
Get resources for patients and families, including information on food, housing, transportation, financial assistance, mental health and more.
