Contact the Epilepsy Program
A team that works as one
Seattle Children’s epilepsy experts work seamlessly across specialties to deliver coordinated care for kids — from babies through teens. As Washington’s only Level 4 pediatric epilepsy center, Seattle Children’s provides the highest level of epilepsy care — designed specifically for kids.
Expert care, working together for your child
Epilepsy Services We Provide

First Time Seizure Clinic
We evaluate children who have had a seizure for the first time to learn more about the type of seizure, its cause and whether they may have epilepsy. It is important to determine if the seizure was provoked (caused by a temporary problem like a concussion or high fever) or is an epileptic seizure. Epilepsy is not the cause of seizures in up to half of children who visit our clinic.
- At your first visit, a neurology provider evaluates your child and talks with you about seizures.
- If needed, your child has an EEG, a painless recording of the brain’s electrical activity. The EEG may happen that same day or during a return visit.
- Some children return to see a neurologist or epilepsy specialist.
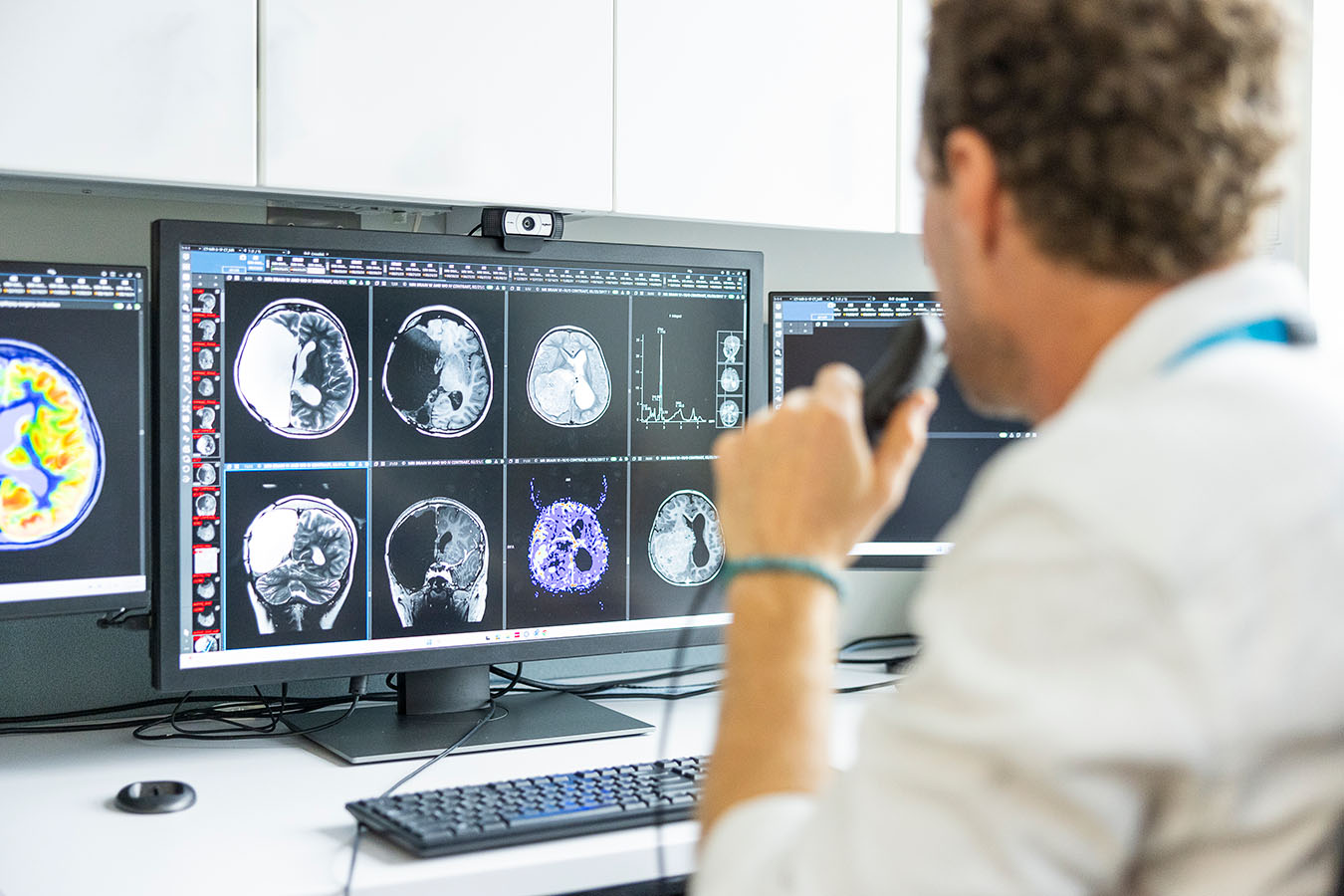
Advanced Epilepsy Diagnostics
To help us understand your child’s seizures, make an accurate diagnosis and recommend the best treatment, we monitor them for several days in the hospital with EEG and video. In addition, we use state-of-the-art imaging like functional MRI to see where seizures start in your child’s brain and to protect areas that are important for speaking and moving. Genetic testing helps us diagnose children sooner and more precisely. Identifying the type of seizures your child has and if they have an epilepsy syndrome is the key to successful treatment. Learn more about how we diagnose and treat children with epilepsy.
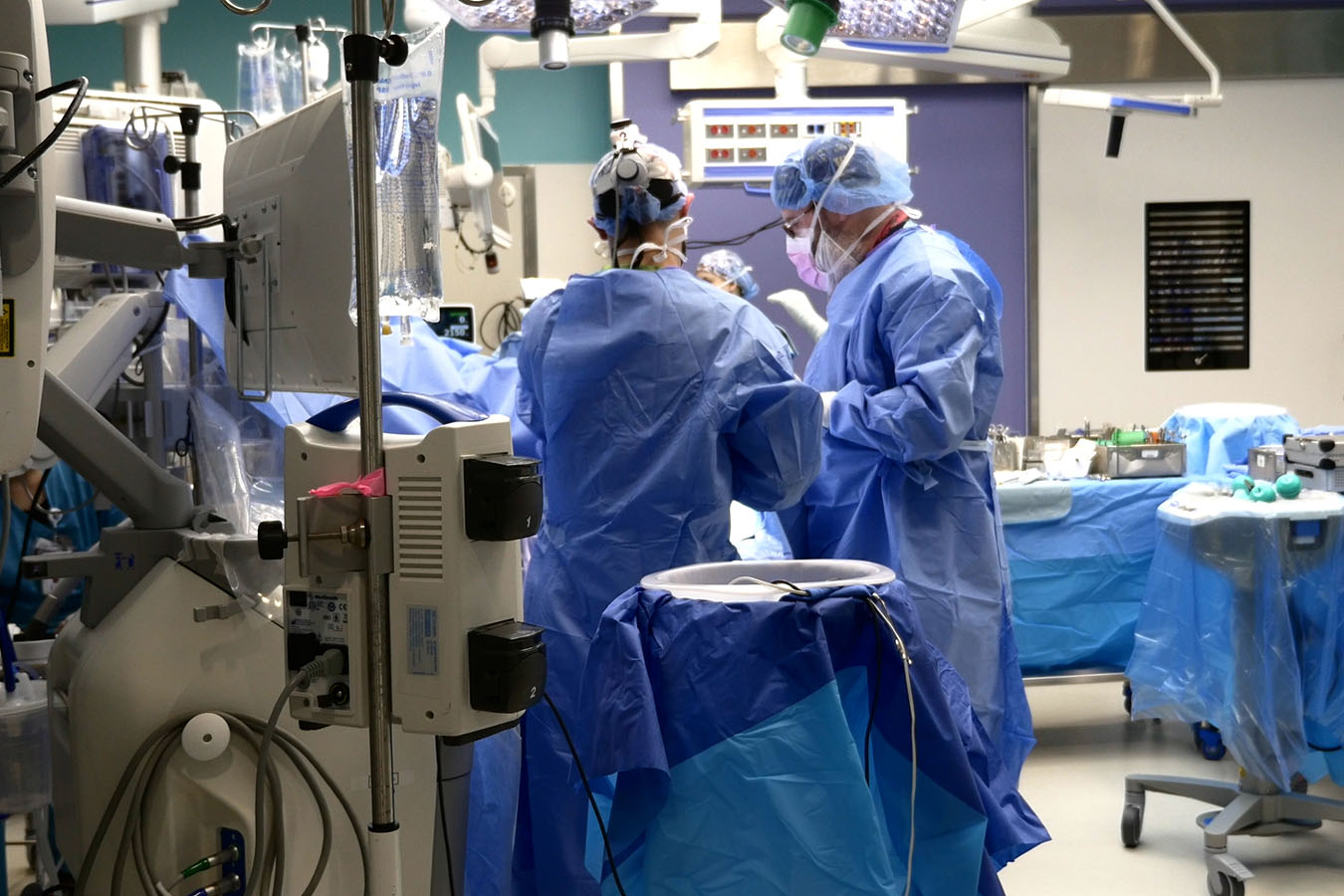
Epilepsy Brain Surgery Experts
We perform significantly more neurosurgeries than any other children’s hospital in our WAMI region. More cases mean greater expertise and a sharper ability to determine if surgery is even needed – and that adds up to better outcomes. Our skilled use of advanced technology makes brain surgery possible for more children, as well as safer and more precise. We provide the most innovative, minimally invasive surgeries offered by the nation’s top children’s hospitals, including laser ablation for epilepsy and procedures using the ROSA™ robotic surgical tool. These advances offer the chance to live seizure-free for some kids who have run out of treatment options. Read about how an awake brain surgery stopped Jasmine's seziures.
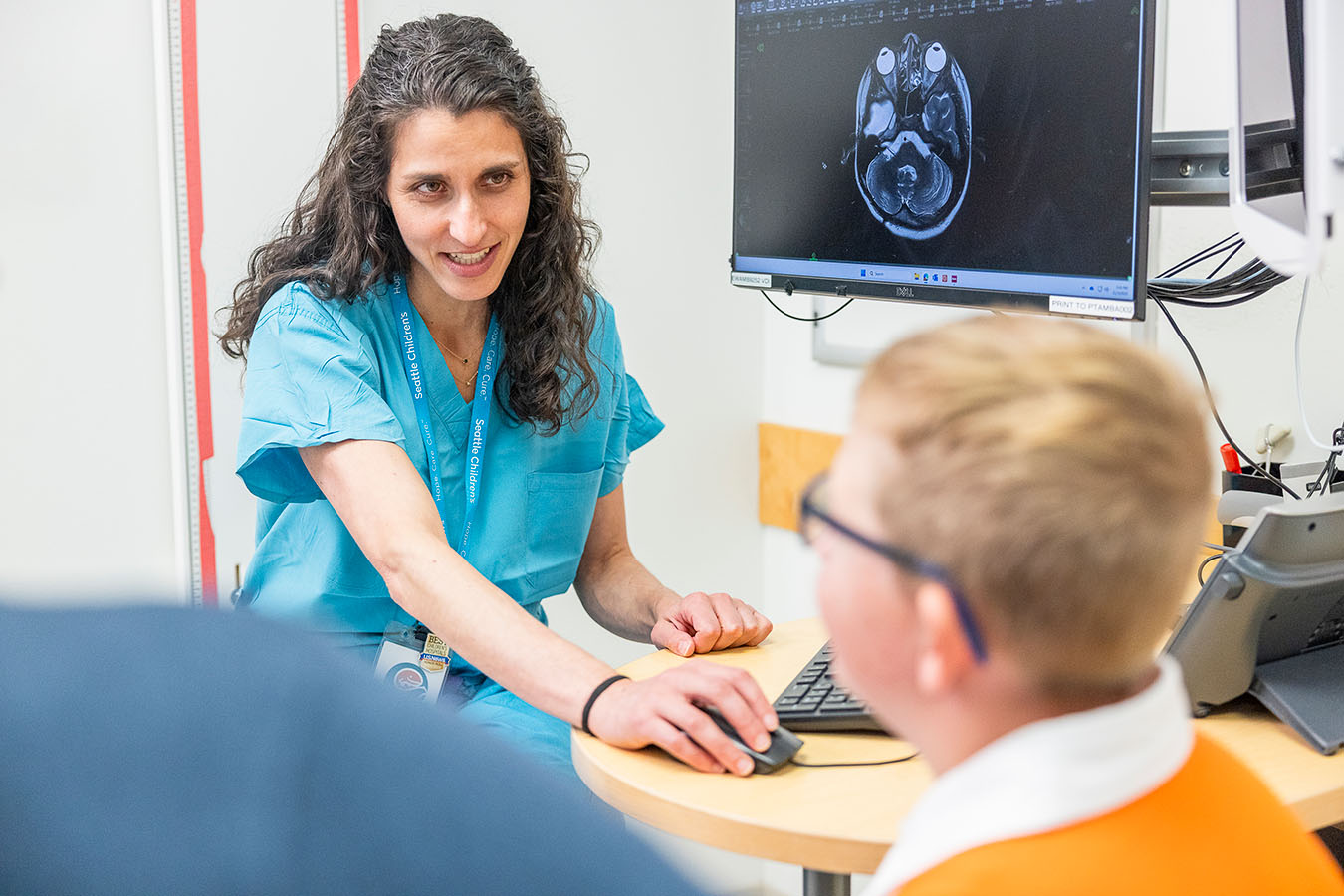
Epilepsy Research
The care we provide your child is advanced by our research in the lab and with patients. For example, our work to identify genes that play a role in epilepsy has opened the door to new therapies that help us personalize your child’s treatment. With the nation’s top leaders in neurological care and research, we offer patients access to promising new treatments being studied in clinical trials. Read more about our extensive epilepsy research.
Epilepsy Program Stories
Epilepsy Conditions We Treat
We see children with a broad range of neurological conditions that involve seizures, including:
Epilepsy Resources for Patients & Families
Support for your whole family
Learning that your child has epilepsy can be stressful for the whole family, which is why our program was designed with a complete support system. Our doctors, nurses, child life specialists and social workers help your child and your family through the challenges of their illness. Whether you live nearby or far away, we can help with financial counseling, school, housing, transportation, interpreter services and spiritual care. We also connect you to community resources and support groups.

- Ambulatory EEG Monitoring (PDF) (Somali) (Spanish) (Vietnamese)
- EEG Tests (PDF) (Spanish)
- EEG Prep Book: A short story about what it’s like to have an EEG (electroencephalogram) test at Seattle Children’s(PDF)
- Epilepsy Monitoring Unit Family and Visitor Guidelines (PDF) (Somali) (Spanish) (Vietnamese)
- Long-Term Video/EEG Monitoring (PDF) (Spanish) (Vietnamese) (Russian)
- Neuromodulation Program
- Neuropsychology Evaluation (PDF) (Russian) (Spanish)
- Prolonged Video/EEG Monitoring (PDF) (Spanish)
- Ketogenic Diet and Your Child (PDF)
- Seizure First Aid (PDF) (Amharic) (Arabic) (Russian) (Simplified Chinese) (Somali) (Spanish) (Ukrainian) (Vietnamese)
- Seizures and/or Epilepsy: Answers to Common Questions (PDF) (Amharic) (Arabic) (Russian) (Simplified Chinese) (Somali) (Spanish) (Vietnamese)
- Seizures from a Fever (PDF) (Russian) (Spanish)
- Water Safety for Children with Epilepsy or Seizures (PDF) (Amharic) (Arabic) (French) (Russian) (Simplified Chinese) (Somali) (Spanish)
- Your Child's Hospital Stay to Start the Ketogenic Diet (PDF) (Arabic) (Spanish)
Epilepsy Care Where You Need It



