Current Research
 Adults with cerebral palsy often report a decline in mobility as they age. About half of adults with CP who are able to walk during childhood are unable to walk outside their home by age 25. Our current studies aim to increase our understanding of how children with CP can maintain or increase mobility, particularly as they age. If you are interested in including your child as a participant, please follow the links to the study pages.
Adults with cerebral palsy often report a decline in mobility as they age. About half of adults with CP who are able to walk during childhood are unable to walk outside their home by age 25. Our current studies aim to increase our understanding of how children with CP can maintain or increase mobility, particularly as they age. If you are interested in including your child as a participant, please follow the links to the study pages.
A Study of Orthotics and Walking Activity in CP
An NIH Exploratory/Developmental Research Grant (R21)
 Our orthotics study invites participants with bilateral spastic CP to be specially fitted with custom orthotics using an algorithm that is the standard of care in the United Kingdom.
Our orthotics study invites participants with bilateral spastic CP to be specially fitted with custom orthotics using an algorithm that is the standard of care in the United Kingdom.
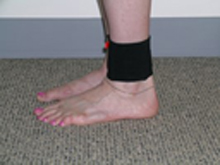
Fitting children with orthotics – plastic braces that slip into their shoes and support their legs below the knee – is a common practice used to optimize walking patterns of patients with CP. The idea is to correctly align the child’s legs and feet so the rest of the body can perform at its best. Despite their frequent use, there is no standard approach to the prescribing of orthotics in the United States.
 In addition, a pair of orthotics can cost anywhere from $3,000 to $5,000 and many insurance companies allow a child only one pair per year. When you apply that rule to growing children, it becomes a problem. Children who have ill-fitting, uncomfortable and ineffective orthotics are less likely to wear them. They walk less and they lose muscle strength and power even faster.
In addition, a pair of orthotics can cost anywhere from $3,000 to $5,000 and many insurance companies allow a child only one pair per year. When you apply that rule to growing children, it becomes a problem. Children who have ill-fitting, uncomfortable and ineffective orthotics are less likely to wear them. They walk less and they lose muscle strength and power even faster.
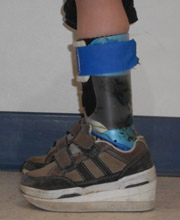
Our study is testing a potentially effective orthotics-fitting algorithm, the Ankle Foot Orthoses-Footwear Combination (AFO-FC), which is already the standard of care in the United Kingdom.
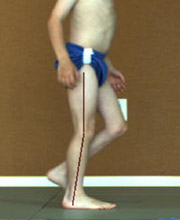 The AFO-FC method involves creating a mold of a child’s ankle, which is then used to assemble customized braces. These are complemented by modified shoes, which look like typical high-top sneakers but can have wedging inside or added to the sole. Clinical trial participants are analyzed in a gait lab when they first get their new orthotics and again three months later. Participants are sent home with a GPS tracker and pedometer on each ankle so we can measure how the orthotics are effecting the child’s walking activity outside of controlled, clinical settings. Parents are also given a camera and asked to take pictures that demonstrate how the orthotics have impacted their everyday lives.
The AFO-FC method involves creating a mold of a child’s ankle, which is then used to assemble customized braces. These are complemented by modified shoes, which look like typical high-top sneakers but can have wedging inside or added to the sole. Clinical trial participants are analyzed in a gait lab when they first get their new orthotics and again three months later. Participants are sent home with a GPS tracker and pedometer on each ankle so we can measure how the orthotics are effecting the child’s walking activity outside of controlled, clinical settings. Parents are also given a camera and asked to take pictures that demonstrate how the orthotics have impacted their everyday lives.
Many children wearing AFO-FC orthotics have improved their walking enough that they eventually no longer need braces. Results from this study could lead to a standardization of orthotics treatment in the United States.
If you are interested in knowing about this study, email Tony To.
PT3: Power Training Combined with Interval Treadmill Training to Improve Walking Activity in Cerebral Palsy
An NIH Research Project Grant (R01)
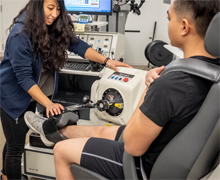 Our PT3 study invites participants to train like an athlete. It combines power training with strength building to discover which types of physical exercises can increase the amount of walking and levels of activity performed by children with CP.
Our PT3 study invites participants to train like an athlete. It combines power training with strength building to discover which types of physical exercises can increase the amount of walking and levels of activity performed by children with CP.
 Generating physical muscle force quickly (power) is a significant challenge for children with CP. Muscle power is what makes it easy for you to get up from the floor when you're three and then becomes harder when you're 13 and even harder when you're 33 and 63. Strength building exercises increase your force production. However, the ability to produce force quickly requires power, which is why athletes switch between strength building and power training exercises.
Generating physical muscle force quickly (power) is a significant challenge for children with CP. Muscle power is what makes it easy for you to get up from the floor when you're three and then becomes harder when you're 13 and even harder when you're 33 and 63. Strength building exercises increase your force production. However, the ability to produce force quickly requires power, which is why athletes switch between strength building and power training exercises.
 Traditional CP therapies tend to focus on strength building as a kind of standard of practice. With this study, we're comparing strength training to power training, which is something that's considered outside the box for traditional therapies.
Traditional CP therapies tend to focus on strength building as a kind of standard of practice. With this study, we're comparing strength training to power training, which is something that's considered outside the box for traditional therapies.
We have already conducted lab-based power training trials that have produced some very positive outcomes for the participants’ walking activity. Participants became more powerful, their muscles got bigger and they began to walk more. With this study, we're trying to determine if power training can be effectively applied in clinic setting.
If you are interested in knowing about this study, email Sinear Sadang.
Short Burst Locomotor Treadmill Training Study (SBLTT)
An NIH Research Project Grant (R01)
 Our SBLTT study is a home-based intervention study that compares steady-state treadmill training (standard of practice) to a novel short-burst interval locomotor treadmill training program. Short-burst interval locomotor treadmill training (SBLTT) requires the participants to alternate back and forth between a really fast and slow walking speed. Pilot data from our previous R21 grant shows that the SBLTT actually improves the amount of walking kids do in the community.
Our SBLTT study is a home-based intervention study that compares steady-state treadmill training (standard of practice) to a novel short-burst interval locomotor treadmill training program. Short-burst interval locomotor treadmill training (SBLTT) requires the participants to alternate back and forth between a really fast and slow walking speed. Pilot data from our previous R21 grant shows that the SBLTT actually improves the amount of walking kids do in the community.
After each of four assessment visits, participants are asked to wear a StepWatch pedometer on one ankle and a GPS device on the other in order to track how much the kids are walking and where in the community they are taking these valuable steps. Pilot data suggests that participants partaking in the novel SBLTT program also end up walking more in their communities. In other words, SBLTT translates to community walking!
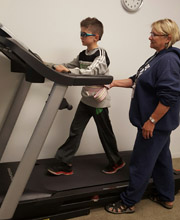 One of the unique features of the current study is that we bring the intervention to the families’ homes. Participants receive treadmill training 5 days per week for 8 weeks by a team of licensed physical therapists who come to the home to deliver the treatment, a total 40 total sessions treadmill training sessions. The study also requires four assessment visits at Seattle Children’s Research Institute in Downtown Seattle and that participants wear the Stepwatch and GPS devices for 7 days after each study visit.
One of the unique features of the current study is that we bring the intervention to the families’ homes. Participants receive treadmill training 5 days per week for 8 weeks by a team of licensed physical therapists who come to the home to deliver the treatment, a total 40 total sessions treadmill training sessions. The study also requires four assessment visits at Seattle Children’s Research Institute in Downtown Seattle and that participants wear the Stepwatch and GPS devices for 7 days after each study visit.
We are excited to learn if this intervention can be as effective when conducted in-home as it has proven to be in a lab setting.
If you are interested in knowing about this study, email Neil Panlasigui.
Pedal With Pete Award: Study on Joint Decision Making in Supported Mobility Devices
 The Pedal With Pete foundation awarded us a grant to study how decisions about different mobility devices and adaptive equipment are made on behalf of children with CP. Many children with CP never walk or walk for very few years in their life. Choosing the right adaptive equipment, like wheelchairs, power wheelchairs, walkers and other devices is extremely important.
The Pedal With Pete foundation awarded us a grant to study how decisions about different mobility devices and adaptive equipment are made on behalf of children with CP. Many children with CP never walk or walk for very few years in their life. Choosing the right adaptive equipment, like wheelchairs, power wheelchairs, walkers and other devices is extremely important.
We’re conducting the study through focus groups in Seattle, Los Angeles, Chicago and Boston. To learn more, email Kristie Bjornson.
Cerebral Palsy Research Network
 Seattle Children’s is an official regional site of Cerebral Palsy Research Network (CPRN), which seeks to improve outcomes that people with CP value most through high quality clinical research and quality initiatives.
Seattle Children’s is an official regional site of Cerebral Palsy Research Network (CPRN), which seeks to improve outcomes that people with CP value most through high quality clinical research and quality initiatives.
As a CPRN site, patients with CP receiving care at Seattle Children’s can have treatment data anonymously included in the CPRN registry. This enables clinician researchers across the country to find practice variation and create quality initiatives to improve outcomes for all patients regardless of where they are treated.
The many research institutions participating in CPRN are enabling a new level of collaboration between basic scientists and clinical researchers; helping focus research on solving the most important questions for the CP community. Learn more about Cerebral Palsy Research Network.
