Publication Q&A: Brain Researchers Offer Insights into Brainstem Region’s Role in Chronic Low Oxygen Levels, Disrupted Swallow
Published
Featured Researchers
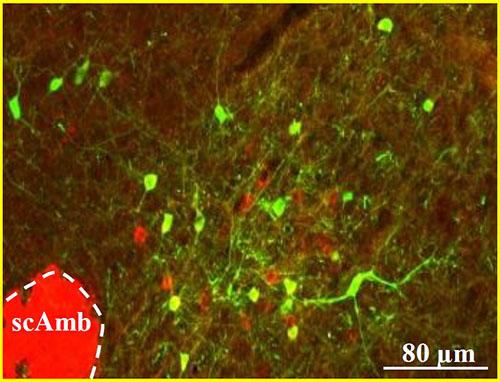 In a follow-up to earlier work, researchers in the Norcliffe Foundation Center for Integrative Brain Research (NFCIBR) tested the impact of chronic low oxygen levels on normal swallowing caused by alterations in a particular brainstem region. The findings are crucial for understanding the mechanisms underlying disordered swallow in obstructive sleep apnea and other breathing and neurological disorders.
In a follow-up to earlier work, researchers in the Norcliffe Foundation Center for Integrative Brain Research (NFCIBR) tested the impact of chronic low oxygen levels on normal swallowing caused by alterations in a particular brainstem region. The findings are crucial for understanding the mechanisms underlying disordered swallow in obstructive sleep apnea and other breathing and neurological disorders.
The National Institutes of Health-funded study was led by Dr. Alyssa Huff, a postdoctoral researcher in the lab of Dr. Jan-Marino (Nino) Ramirez, principal investigator and professor of neurological surgery at the University of Washington School of Medicine. Drs. Marlusa Karlen-Amarante and Luiz Oliveira, also Ramirez Lab postdoctoral researchers, contributed to the research.
What are the significant findings of this paper?
This research is a continuation of our 2023 findings where we discovered a brainstem region, the postinspiratory complex (PiCo), aids in coordinating swallow and breathing. In this study, we found that when exposed to chronic bouts of intermittent hypoxia (low oxygen levels), swallow activity is highly variable, indicating dysphagia (disordered swallow).
This tells us a few things: PiCo is not only involved in coordinating swallow and breathing, but it also helps to keep swallow motor activity (the activity of swallow-related muscles and nerves) working properly. Swallow-breathing coordination was not altered when exposed to chronic intermittent hypoxia; therefore, this function of PiCo was not disturbed.
We speculate that the disordered swallow associated with obstructive sleep apnea occurs due to changes in swallow function, rather than its ability to coordinate with breathing. The study offers insights into how and why dysphagia occurs in diseases and disorders associated with chronic bouts of intermittent hypoxia.
What does this research tell us that we didn’t know before?
Chronic bouts of intermittent hypoxia can occur in many diseases. While the use of chronic intermittent hypoxia (CIH) is traditionally experimentally used to study the effects of obstructive sleep apnea, CIH can occur in many pediatric disorders, such as Leigh syndrome, Rett syndrome, epilepsy, familial dysautonomia, congenital central hypoventilation syndrome, etc. This method gives us the opportunity to understand what happens to the brain and body when exposed to multiple intermittent bouts of low oxygen over a long period of time.
In 2022, we characterized the effects of CIH on the brainstem region known to control inspiration and how the changes in this region affect normal swallow production. We concluded that a specific subset of neurons in the preBötzinger complex altered the laryngeal function of swallow. Here, we repeated this study and looked at PiCo and showed that CIH affects PiCo’s ability to regulate not just laryngeal function, but also the muscles of the submental complex (the muscles under the chin).
What are the broad implications of this research?
Since CIH is a characteristic of many pediatric diseases and disorders, and many of these children suffer from dysphagia and feeding complications, we are one step closer to understanding the mechanisms responsible for normal swallow production.
What are the next steps and long-term goals for this research?
We are collaborating with NFCIBR’s Dr. Franck Kalume in looking at swallow-breathing discoordination in a small-animal model of Leigh syndrome. Difficulty swallowing hinders eating and is among the first clinical symptoms of Leigh syndrome. This model has similar symptoms as the patient population, such as swallow dysfunction and swallow-breathing coordination. We have begun looking at PiCo in the model and at therapies targeting this area to rescue swallow-breathing coordination in the model.
Additionally, we are studying swallow and breathing interactions in a small-animal model of Rett syndrome, using the same methods and techniques as the Leigh syndrome model to understand the neurocircuitry of swallow and its coordination with breathing. These two syndromes experience both chronic bouts of intermittent hypoxia and feeding and swallowing difficulties.
Our long-term goal is to understand the neural circuits and pathways involved in normal swallow production. Combined with the knowledge we gain from the alterations of brainstem regions in disease models, we can target these specific areas therapeutically to hopefully decrease or even eliminate dysphagia and aspiration pneumonia in these diseases and disorders.
Featured Researchers
Related Centers & Programs
Related Articles

Publication Q&A: ANKLE2-related Microcephaly: A Variable Microcephaly Syndrome Resembling Zika Infection
Published
Changes in the ANKLE2 gene cause a unique syndrome where children have microcephaly (small brain size) apparent either at birth or shortly after birth, with a broad range of other structural brain abnormalities.
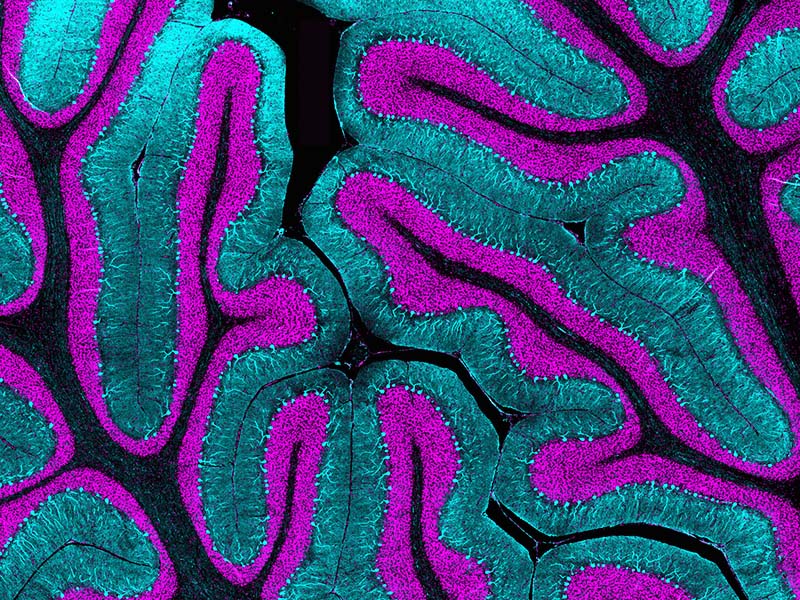
Pinpointing the Origin of Deadly Brain Tumors
Published
In two papers published in Nature, Dr. Kathleen Millen and her team are the first to identify the cells that give rise to the most aggressive forms of medulloblastoma.
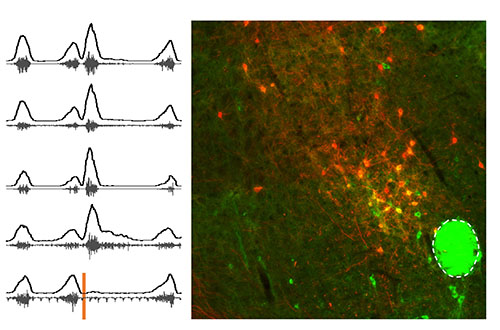
Brainstem Region Revealed to Play Role in Regulating Swallow, Breathing
Published
Seattle Children’s researchers revealed novel insights about PiCo, a brainstem region that aids the coordination of swallowing and breathing.

