How the Fetal Care and Treatment Center Is Focused on Expanding Services and Close-to-Home Care: A Q&A With Drs. Bettina Paek, Martin Walker and Bhawna Arya
February 1, 2023
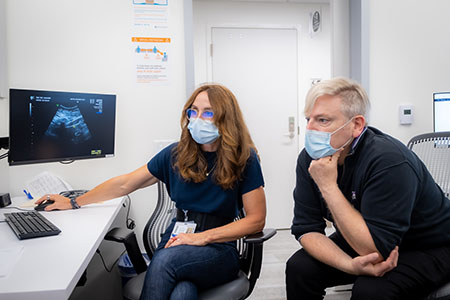 Maternal-fetal surgeons Drs. Bettina Paek and Martin Walker review a patient’s scan.
Maternal-fetal surgeons Drs. Bettina Paek and Martin Walker review a patient’s scan.
Last year, Seattle Children’s brought on board renowned fetal intervention specialists Drs. Bettina Paek and Martin Walker to lead Seattle Children’s and UW Medicine’s new Maternal Fetal Intervention and Surgery program alongside Dr. Rebecca Stark. As members of the Fetal Care and Treatment Center at Seattle Children’s, they are part of a multi-disciplinary team that offers fetal diagnosis and treatment and helps parents understand what to expect after their child is born. The team includes more than four dozen specialists in maternal-fetal medicine, neonatology, cardiology, urology, nephrology, neurology, otolaryngology, craniofacial, surgery, genetics, and radiology.
Over the last year, the Center performed 2,449 fetal echocardiograms across the WAMI region, more than any other provider group in the Pacific NW, with more than 99% accuracy of prenatal diagnosis of major heart conditions. Drs. Paek and Walker performed 34 laser ablation procedures for twin-to-twin transfusion syndrome (TTTS) at the University of Washington Medical Center Montlake Campus (UWMC), with dual survival for more than 90% of the procedures (compared to a national average of 60%).
Our Congenital Diaphragmatic Hernia Program (CDH) team, led by Dr. Rebecca Stark, diagnosed 16 babies with CDH who required newborn surgery and achieved over a 90% average survival rate, again significantly higher than the national average.
We spoke with Drs. Walker and Dr. Paek, as well as with Dr. Bhawna Arya, who leads Seattle Children’s fetal diagnosis program with Dr. Edith Cheng and fetal cardiology, to hear about what is coming in 2023 and answer questions commonly asked by community providers.
Q: Looking ahead at the field of fetal care and treatment, what is on the horizon at Seattle Children’s?
Dr. Walker: There are exciting new possibilities opening up for fetal therapies and surgery. Our Center, with its strong track record and firm support from hospital leadership, is set up to bring the latest advances to families in our region as they become available. The team we have here is amazing. In our first year at Seattle Children’s, one thing that’s been especially impressive to Bettina and me has been the huge enthusiasm from the nursing and anesthesia staff we work with at UWMC Labor and Delivery unit. They are immersing themselves in learning about fetal surgery and creating a great experience for families.
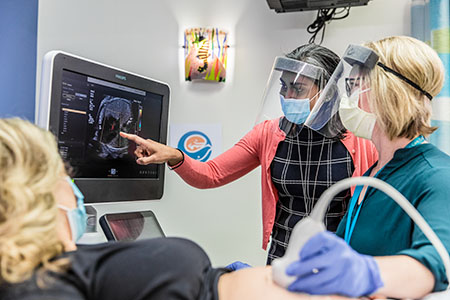 Pediatric cardiologist Dr. Bhawna Arya, director of Fetal Diagnosis, reviews a scan with a patient.
Pediatric cardiologist Dr. Bhawna Arya, director of Fetal Diagnosis, reviews a scan with a patient.
Dr. Paek: I agree. They have been amazing. We work with a group of nurses who are highly trained, intellectually curious, excited by innovation and very motivated to be part of something new. Many have volunteered their days off to take care of these patients and be involved in every facet of their care. It’s not just business as usual; they go above and beyond.
Dr. Arya: I’m excited that we are providing more services – including some of the most complex therapies and interventions available in maternal fetal medicine – AND more integration of our services. We now have a number of specialists embedded in the Fetal Care and Treatment Center. Having that combined expertise gives families the best possible experience. For example, if we see a patient with heart disease but our UW Medicine MFM specialists see renal or other problems on ultra sound, it’s easy to gain expertise from our other pediatric subspecialists to better prepare the family. A big part of my job that I love is collaborating with these other specialists – for example, urologists, nephrologists, and palliative care specialists — and escorting parents through important discussions about their next steps.
Dr. Paek: To Bhawna’s point, Martin and I have found what a benefit it is to have regular conversations with Seattle Children’s specialists who are experts in the challenges our patients face after the birth and during childhood. That’s a part of their care we weren’t as immersed in prior to joining Seattle Children’s. We all learn from each other. It helps us consider the whole picture for the family and be better able to answer their questions during pregnancy.
Q: How is Seattle Children’s making fetal care and treatment more accessible for families who live outside Seattle?
Dr. Arya: Bringing care closer to home is a high priority. In the Seattle area, we’ve expanded our fetal cardiology diagnostic services to our regional clinics in Everett, Federal Way and Bellevue, as well as Central and Eastern Washington. We also offer fetal diagnostic services in Montana and Alaska through our Heart Center clinics there. Part of my job is to support our Heart Clinic cardiologists so they can make a diagnosis and recognize when things are wrong with a fetal heart and help coordinate next steps for the team and the family.
I also make it a point to talk with NICU providers in our region and in outlying areas to see what the barriers are to keeping families close to home so we can address them whenever possible and help providers feel more comfortable caring for these patients locally. Not every baby with a heart condition or other abnormality needs to have a UW Medicine birth and be transported immediately to Seattle Children’s. Even some babies who require surgery in the first week of life can be born close to home, stabilized with medications and brought to Seattle Children’s after that.
Q: What services are available at the regional clinics?
Dr. Arya: Fetal echos and cardiology consultation are available at more than a dozen of our Seattle Children’s clinic locations throughout Washington, Alaska, and Montana. To meet the especially heavy demand in the Puget Sound region, we’ve added extra appointments (2 full days per week) in Bellevue and Everett. These are staffed by the same fetal cardiologists who see patients at Springbrook (next to the hospital).
Q: Do families have to give birth at UW Medicine?
Dr. Arya: It’s important for providers to know that one of our primary goals is to keep care as close to home as possible. We aim to keep OB care with the referring provider and to support moms in giving birth wherever they are most comfortable, unless their condition dictates otherwise. For certain high-risk births or when the newborn will need immediate care at Seattle Children’s, the birth needs to be at UW Medicine. But there are plenty of times when a birth closer to home is an option. We help families have agency in their pregnancy and birth as much as possible.
Q: What’s “see something, say something”?
Dr. Arya: It’s my shorthand for saying we want OBs to call us right away if you have uncertainty about your patient’s ultrasound. We and the UW Medicine MFM team are readily available to see your patient for either an ultrasound, a fetal echo, or both. It’s all we do every day…heart, heart, heart, and we’ve increased our fetal cardiology team over the past year, so your patients won’t have to wait to be seen. We are happy to get those calls. We can make a diagnosis in some cases as early as 14 weeks. Parents need time to learn about a diagnosis, process it and decide what to do and how they may need to support their child. A late diagnosis in some families can lead to an inability to make a timely decision about their pregnancy.
Dr. Paek: I’ll add we are happy to see all monochorionic twins. We work with our referring physicians and our UW Medicine MFM colleagues to craft individualized recommendations for complicated monochorionic twin pregnancies. We welcome providers’ calls about these cases. The vast majority of monochorionic babies will be healthy and normal but unless they are properly screened we don’t know which ones those are. Patients don’t have to have very sick twins to come and see us; they can come and see us for an evaluation even if they are an apparently healthy, normal monochorionic twins to see if we can offer any suggestions or to make a plan for the remainder of their pregnancy. We can do this virtually also.
Q: How is Seattle Children’s staying at the forefront of fetal medicine?
Dr. Arya: I serve on the board of the Fetal Heart Society, as does Dr. Nelangi Pinto, and am involved with several of their multi-center research projects. I’m currently leading a study of how the pandemic impacted fetal diagnoses and outcomes, because some pregnant women were discouraged from coming to doctors’ offices for safety reasons. We will apply what we learn to improve maternal-fetal outcomes in future public health emergencies.
Within our own Center, we have an 8-year-old database that is ripe for assessment that we query often with the goal of improving our diagnostic criteria, processes and outcomes and reducing disparities in fetal care. We look forward to sharing this information with our region’s OB and radiology teams.
Dr. Walker: Research is a high priority on the fetal intervention side too. We’ve prepared a research protocol to offer minimally invasive repair for spina bifida in the coming year or two. We’re also involved with research on the use of shunts to address fetal pleural effusion (water on the lungs) and bladder outlet obstruction. We’re very active in international research into monochorionic twins.
Dr. Paek: Another aspect of our research is that we perform simulations to practice surgical techniques as a team and to teach surgical techniques to other members of the team who are new to it. This gives us an improved ability to offer the newest fetal interventions as they become available.
Q: When sending a referral, should it go to UW or Seattle Children’s?
For a fetal abnormality, the patient can be referred to Seattle Children’s or UW Medicine. The maternal/fetal diagnostic workup will begin at either location as our teams are integrated with one another and we will ensure the patient receives comprehensive care at either location.
For a fetal intervention, the patient should always be referred to Seattle Children’s even if the fetus is 24 weeks or more. The fetal intervention consultations will begin at Seattle Children’s Springbrook location next to the hospital. If there is a need for a procedure on a fetus at 24 weeks gestation or more, the team from Seattle Children’s will work jointly with the UW Medicine team to schedule the procedure at the UW Medicine.
Q: If a patient needs to be seen quickly for fetal intervention and surgery, how available are you for urgent calls?
Dr. Paek: We see patients same-day or next day when it’s urgent. When it’s urgent, you don’t need to submit a referral first. Call our fetal intervention nurse coordinator, Melissa Dorn, at 206-987-4137, or you call Martin or me directly. My cell is 206-696-4404. Martin’s cell is 425-802-2201. We want and expect to be called for any urgent matter.
Q: Anything else you want our readers to know?
Dr. Walker: We welcome your requests for second opinions. We get referrals from outside of the Seattle Children’s system, whether it be locally from our military colleagues or from other practices in the region, all the way to people who are looking for a second opinion from California, Colorado or further east. Even if the family ends up keeping care close to home, sometimes they just want an outside perspective to make sure that their local team is on the right track.