Selective Dorsal Rhizotomy Helps Kids With Cerebral Palsy Gain Mobility and Independence
Seattle Children’s has the right mix of expertise to offer kids with spastic cerebral palsy a path toward independence.
More than anything else, 3-year-old Arabelle Laddusaw wants to run.
Her big brother, Richard, 15, promised that when Arabelle can run, he’ll teach her to play soccer. If it were just a matter of will, she’d already be out on the field.
Arabelle is “very stubborn and very determined,” says her mom, Christine Laddusaw. That’s a good thing, because before she can run, or even stand up, Arabelle has to relearn how to move now that her body’s perpetually rigid muscles have finally relaxed, thanks to a complex surgical procedure at Seattle Children’s.
Arabelle was born with spastic cerebral palsy (CP), a condition that made the muscles of her hips and legs inflexible and hard to control. It’s as if the message center between her brain and muscles were stuck in the “on” position.
Looking for better options
Spasticity makes it hard to isolate movements, but Arabelle was determined not to be left behind by her siblings. She learned to crawl by “bunny hopping,” drawing both legs up together. When she used her walker, her feet would cross, tripping each other up.
Although CP itself doesn’t worsen over time, persistent spasticity will stress and deform the joints, thus limiting range of motion. It can also cause chronic pain and fatigue – diminishing mobility even more. Laddusaw got her daughter into physical therapy as an infant and began to explore options.
2 in every 1,000 children are born with cerebral palsy
When Dr. Susan Apkon, a Seattle Children’s rehabilitation specialist, began seeing Arabelle in Billings, Montana (where the Laddusaws live), she gave her botulinum toxin and phenol injections to relieve the muscle tightness. But the shots were only a temporary fix. Once the medicine wore off, the spasticity would return and Arabelle would need another injection.
Apkon suggested the Laddusaws come to Seattle Children’s for a permanent solution that combines surgery (selective dorsal rhizotomy, or SDR) with weeks of intense inpatient occupational and physical therapy followed by months of outpatient therapy at home.
60% of abnormal sensory nerves are typically disconnected during a selective dorsal rhizotomy
For the right child, SDR is transformative,says Apkon. “But it demands an extraordinary commitment from the child and the family, who both have to be active participants in rehab. Fortunately, Arabelle has a huge drive to walk, she’s willing to follow instructions and tolerate hands-on manipulation by the therapists, and her mom is completely committed – plus, there are great physical therapists in Billings who can continue her rehab program after discharge.”
Complex surgery
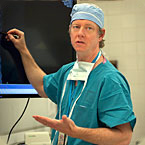
“There’s a whole host of kids who can benefit from this procedure,” says Dr. Samuel Browd. “Given the plasticity of young kids’ brains, you can alter the way the nervous system functions and retrain it. With a patient like Arabelle, not only are we reducing the complications that typically come with long-term spasticity, we’re also making it possible for her to walk independently.”
Neurosurgeon Dr. Samuel Browd likens SDR to the process of fixing malfunctioning wires that carry electricity into a house – it’s a matter of identifying which of those “wires” are acting up and leaving the others alone.
The team makes a small cut in the low back and exposes the nerve bundles beneath one vertebra. Then Browd and the electrophysiologist painstakingly test each bundle to accurately identify the nerves that control motion and the nerves that provide sensation. It’s the malfunctioning sensory nerves that cause spasticity, so Browd then uses tiny electrode hooks to stimulate the sensory nerves and determine which ones are responding abnormally.
“We go through a decision-making process 100 to 120 times during each surgery, discussing the result we get from testing each nerve and deciding which to cut and which to keep,”says Browd.
There’s no room for error – the nerves don’t grow back. Cut motor nerves instead of sensory nerves, and the corresponding muscles are paralyzed.
“Amazing” changes
It’s 2 p.m. and Arabelle is on the treadmill again, supported by a harness that holds part of her weight. Physical therapist Rachelle Steijn cajoles and coaxes, guiding the preschooler’s legs.
Arabelle is adjusting to what must feel like a new body, says Steijn, as her brain and spinal cord learn to respond to new input. “Once the spasticity is gone, the old ways don’t work anymore. She’ll need to take a thousand steps using this brand-new movement pattern before it becomes habit.”
It’s hard, tiring work. Arabelle also has to build strength. Now that her misfiring nerves have been cut, the weakness of the muscles is revealed – rigidity had been masquerading as strength. But after nearly three weeks of intense physical and occupational therapy, twice a day, six days a week, Laddusaw sees profound and exciting differences in her daughter.
“She’s already able to stand up on straight legs and to sit cross-legged – she could never have done that before – it’s amazing,” says Laddusaw. “I know we have a ton of work still. It’s a good thing we both have patience. I think she’ll be able to walk on her own within a year, I really do.”
Arabelle’s big brother Richard will be waiting, soccer ball at the ready.
New independence
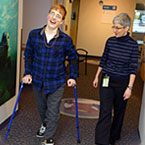
Though he is much older than the typical candidate for selective dorsal rhizotomy, 15-year-old Mark Simoneau successfully lobbied his care team, including Dr. Susan Apkon, for the procedure. “Now,” Mark says, “I’m lighter, more in control of myself.” He’s also free of the leg pain that used to keep him up at night.
Mark Simoneau doesn’t need a new pair of shoes this month. He didn’t need a new pair last month, and he won’t need a new pair next month.
Mark, now 15, used to blow through shoes every few weeks because he couldn’t lift his feet when walking, even when using crutches or a walker. “One pair only lasted five days!” Mark recalls with a rueful laugh. He was prone to falling, and endured painful leg spasms.
Thanks to a successful SDR procedure in August 2011, weeks of inpatient rehab and months of PT with therapists in Bellingham, Washington, Mark has a brand-new level of control over his body – and the independence any teenager craves.
“I had always been dependent on Mom to put on my shoes and leg braces,” says Mark. “Now I can finally tie my own shoes. Plus, the pair I wore home from Children’s lasted nearly a year!”
“Rely on myself”
Mark had tried other spasticity treatments over the years – PT, Botox injections, and the Baclofen pump, a hockey-puck-sized machine embedded in his abdomen to deliver medicine directly to his spinal cord.
Mark was much older than the typical SDR candidate, who is usually between 3 and 5 years old. Apkon worried that his muscles wouldn’t have enough underlying strength to regain his pre-surgery mobility even though the tightness and pain would be relieved by SDR.
“I really did not want that pump back in. I wanted to be able to rely on myself instead of a piece of equipment,” explains Mark, who experienced some serious complications with the pump. He wrote an essay about why he believed SDR was right for him, and convinced his parents and his care team that he was committed to what would surely be an arduous rehabilitation.
“I have always been dependent on Mom to put on my shoes and leg braces. Now I can finally tie my own shoes.”
Eighteen months later, Mark says it’s been worth the effort. It’s not just about the shoes, no longer falling all the time, or the hard-won ability to keep up with his friends as they walk around the mall. “This is about helping me to function in a normal life,” says Mark.
His dream is a career in sports, preferably football. “I know I won’t be able to play, but to be at the stadium as a coach or a broadcaster? That would be great.”
He’s on his way. A few months after leaving Seattle Children’s, Mark was on the field as the water boy for his brother’s football team. Closer to the action, closer to his dream.
Published in Connection magazine, April 2013